 |
Q:
A 57-year-old female presented with a painful stye and tears running down her face for several days. Where do you go from here?
A:
“When a patient presents with a painful, red eye with epiphora, there are a multitude of differential diagnoses that come to mind,” says Shundale Mixon, OD, a staff doctor at the North Georgia Eye Clinic in Clayton, GA. “Put on your detective hat and dig deep for information,” she advises. Ask if this has happened before and inquire about any history of previous eye infections, surgeries or procedures, as well as the time course of the redness, pain and tearing.
 |
|
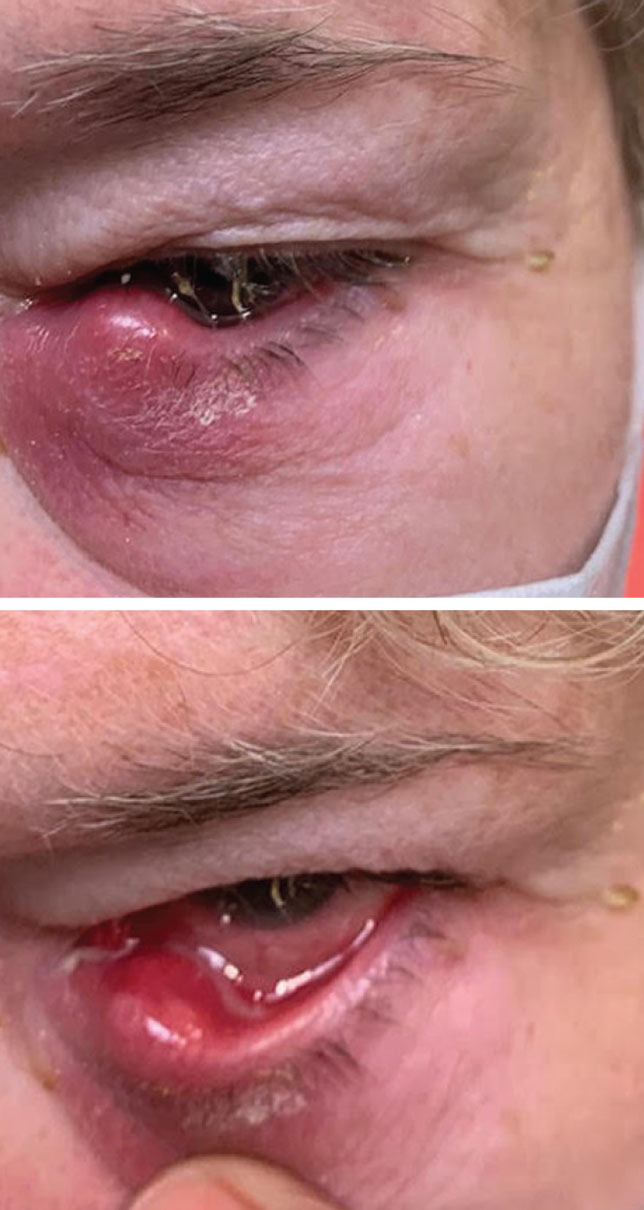
While initial presentation mimicked a chalazion, examination uncovered canaliculitis (bottom). Click image to enlarge. |
Bumps in the Road
A chalazion or hordeolum from meibomian gland disease is often the culprit when you see a lump or bump. But don’t label everything a stye without thinking it through, Dr. Mixon warns. If the lesion is near the punctum, your differential should include two additional disorders, dacryocystitis and canaliculitis, she points out.
Dacryocystitis is inflammation of the nasolacrimal sac that may be caused by a nasolacrimal duct obstruction. Symptoms include a painful, red and swollen tear sac that may produce a pus-like material that seeps out of the punctum when pressure is applied. When discharge is present, there may be an associated conjunctivitis observed. The underlying bacteria that may be responsible for dacryocystitis include Staphylococcus aureus, Staphylococcus epidermidis and Pseudomonas aeruginosa.
Canaliculitis is inflammation of the canaliculus and is associated with redness, tearing and tenderness upon touch. Some common causes include infection or a retained punctal plug. Symptoms appear very similar to dacryocystitis except that in canaliculitis the punctum and canaliculus are red and swollen, whereas the punctum and canaliculus are normal in dacryocystitis and the tear sac is red and tender. Those signs help differentiate these two conditions. The most common bacterial culprit responsible for canaliculitis is Actinomyces israelii.
Dr. Mixon emphasizes that, in this case, it was the repeated questioning about the dry eye history that revealed the fact that punctal plugs had been placed in the inferior punctum of both eyes about a year ago. The punctal plug of the patient’s left eye had lodged down in her canaliculus, which resulted in an eventual external lid infection known as canaliculitis.
Treatment Protocols
Dacryocystitis and canaliculitis management includes an oral and topical antibiotic, warm compresses over the affected site and dacryocystorhinostomy to remove the foreign material. Beta-lactam agents are the first choice for systemic medications due to their ability to inhibit the synthesis of the peptidoglycan layer of bacterial cell walls.
This patient was given amoxicillin-clavulanate 875mg/125mg TID for 10 days and a topical fourth-generation fluoroquinolone, 0.6% besifloxacin ophthalmic solution, QID OS to cover the associated bacterial conjunctivitis. She was referred to an oculoplastics specialist for a dacryocystorhinostomy procedure, and the punctal plug was removed.
When you have a red eye, always obtain a good case history to help narrow down your list of differentials. It can save you valuable time and visits. Not all stye-like lesions are really styes, so make sure that your diagnosis makes sense. “If tearing is the chief complaint, ask if the tears run down the face or just ‘well up’ in the eye,” Dr. Mixon says. “If the former, think about a drainage problem and evaluate the punctal openings, lid apposition to the globe and canalicular and nasolacrimal duct system.”
Dr. Ajamian is the center director of Omni Eye Services of Atlanta. He currently serves as general chairman of the education committee for SECO International. He has no financial interests to disclose.

