The ability of optical coherence tomography angiography (OCT-A) to visualize microvasculature within different layers of the retina makes it useful in assessing various posterior segment diseases, one being papilledema due to idiopathic intracranial hypertension (IIH). Researchers recently identified several peripapillary and macular OCT and OCT-A characteristics that present during different stages of this widely known but under-investigated condition.
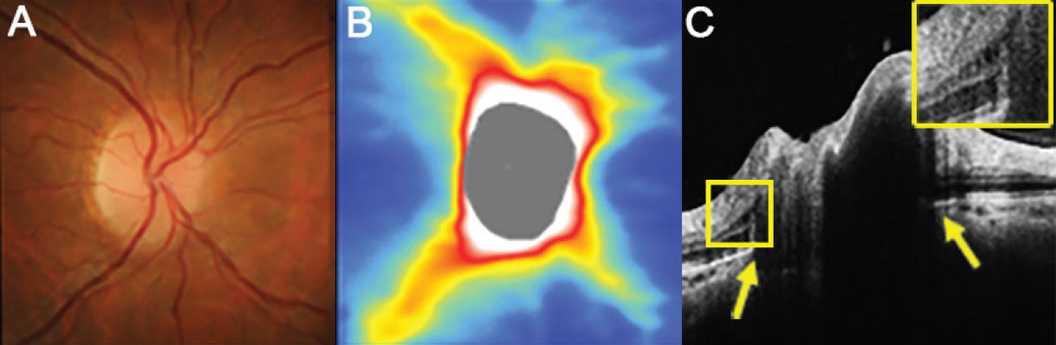 |
| Patients at all stages of papilledema had significantly reduced GC-IPL compared with controls, with the thinnest GC-IPL found in the atrophic group. In these images, (A) the right disc has minimal visible cup with some subtle blurring of the superonasal disc margin, (B) OCT thickness heat map shows thick superior and inferior RNFL and (C) a high-density OCT line scan shows anterior protrusion of Bruch’s membrane at its opening (yellow arrows) and intraretinal cystic spaces temporal to the disc margin (inset). Photo: Henrietta Wang, BOptom (Hons). Click image to enlarge. |
The prospective, observational study included IIH patients with papilledema divided into three groups: early/established papilledema, chronic papilledema and atrophic papilledema. At baseline and three months, OCT was used to evaluate peripapillary retinal nerve fiber layer (RNFL) and macular ganglion cell inner plexiform layer (GC-IPL). Additionally, peripapillary and macular perfusion was documented at superficial retinal, deep retinal and choriocapillary levels using OCT-A.
At three months, RNFL showed significant thinning in all groups, with the atrophic group demonstrating the maximum amount of thinning. The researchers explained in their paper on the findings that “although early/established cases showed thicker RNFL related to disc edema, cases in the atrophic stage showed RNFL thinning due to long-standing edema and consecutive optic atrophy.”
At baseline, patients in all stages of papilledema had significantly reduced GC-IPL compared with controls, with the thinnest GC-IPL found in the atrophic group (72.35µm, 77.05µm and 52.75µm for early/established, chronic and atrophic papilledema, respectively, compared with 84.45µm for controls). At three months, atrophic papilledema patients experienced further deterioration in GC-IPL to 50µm, on average.
Using Image J analysis on OCT-A images, the researchers observed a significant decrease at different levels in the peripapillary and macular perfusion at baseline, especially in the atrophic group. Average visual acuity at follow-up showed a weak negative correlation with baseline RNFL and GC-IPL, as well as a moderately negative correlation with baseline superficial peripapillary retinal perfusion. Increasing grade of papilledema and superficial peripapillary retinal perfusion also showed a significant negative correlation.
Based on this data, the researchers concluded that GC-IPL may be helpful in identifying early damage in papilledema, even in the presence of thicker RNFL.
“As the structural and vascular changes set in early in papilledema, prompt and aggressive treatment irrespective of the grade of papilledema is mandated,” they wrote in their paper. “OCT and OCT-A are not only useful tools to detect these early structural and vascular changes but also help predict the final visual outcomes in papilledema due to IIH.”
Pahuja A, Dhiman R, Aggarwal V, Aalok SP, Saxena R. Evaluation of peripapillary and macular optical coherence tomography angiography characteristics in different stages of papilledema. J Neuro-Ophthalmol. June 26, 2023. [Epub ahead of print]. |

