 |
Q:
A scleral lens wearer presents to the clinic with significant corneal ectasia and what is believed to be a high amount of flexure (as opposed to residual astigmatism coming through). What is a method that can be used to help identify the issue for certain, and how can it be treated or solved?A:
“Flexure with scleral lenses is not unusual,” says Edward S. Bennett, OD, assistant dean for student services and alumni relations at the College of Optometry at the University of Missouri-St. Louis. “If diagnosed as such, [it] can be successfully managed.” Dr. Bennett adds that lens flexure can be most commonly diagnosed using keratometry or topography performed over the lenses while the patient is wearing them. Ideally, the results from the exams should demonstrate a spherical value like 43 x 43, while presence of a toric overkeratometry value of 43 x 44, for example, indicates flexure possibly caused by a steep base curve radius that leads to apical clearance, a thin lens design and/or the presence of a hyperpermeable lens material.
Stephanie L. Woo, OD, of the Havasu Eye Center specialty lens practice in Arizona, points out that there are several ways to reduce or eliminate lens flexure, most notably by increasing the center thickness of the lens. “This [method] works in some cases, but the oxygen to the cornea will be reduced,” she cautions, “so please take that into consideration. As I see more and more patients with lens flexure, I have come to realize [that] many patients ultimately need a toric peripheral curve due to the toric nature of the sclera.” She adds that most of her current patients are wearing a toric peripheral design, especially in the case of larger lenses over 15.5mm in diameter being prescribed.
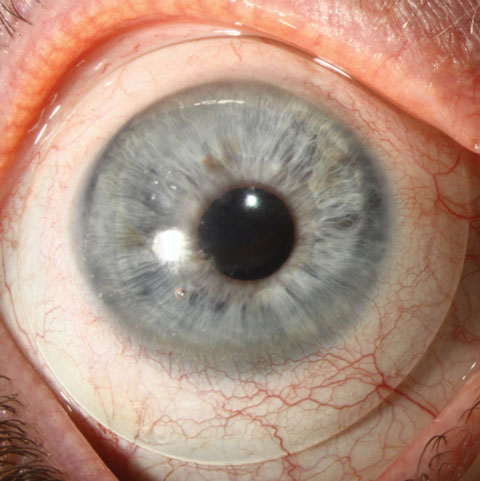 |
| Increasing center thickness is one way to reduce lens flexure, experts say, but it reduces oxygen transmission. Modifying the design by adding a toric peripheral curve may be a better approach. Photo: Christine W. Sindt, OD. |
Jason Jedlicka, OD, clinical associate professor and chief of the cornea and contact lens service at the University of Indiana, suggests a similar initial approach. “Any time visual acuity is reduced in a scleral lens, a spherocylindrical overrefraction should be done to determine if there is astigmatic correction that is unresolved,” he suggests. “If there is, determine if the astigmatism that is refracted is due to flexure, or bending of the lens on the ocular surface, or if it is due to residual astigmatism from the internal eye.”
When performing keratometry or topography over the lens, Dr. Jedlicka notes, practitioners should ensure that the patient does not widen their eyes too much during either test, as this can impact the measurements taken. Following the exam, “if there is an amount of toricity measured that matches the astigmatism in the overrefraction, then the problem is lens flexure,” he concludes, agreeing with Dr. Woo that adding thickness to the lens is a good solution to fix cases of low flexure (i.e., 1D or less).
However, for those patients who exhibit higher amounts of flexure, practitioners should consider adding back surface toricity to the scleral zone of the lens to allow it to better fit the eye and decrease pressure along the meridian of flexure. If even more significant flexure is present, the front optic of the lens can also be added to. Dr. Jedlicka points out that some lens manufacturers can make all three changes simultaneously, but that practitioners should exercise caution when asking for the front toric to be added as the placement of this feature prior to the other two possibilities can lead to overcorrection of the patient’s astigmatism.
Finally, Dr. Jedlicka says, in this particular case, if flexure is not ultimately the cause of the lens issue, the addition of a front toric with or without a back toric haptic to provide rotational stability is one solution that could fix the problem.
