An 85-year-old Hispanic female presents for a comprehensive exam with no visual complaints. The exam is unremarkable, and IOP is 18mm Hg, but upon dilated fundus exam, you see large amounts of cupping. You suspect open-angle glaucoma, but how do you explain the lower IOP? And, given her advanced age, how do you best treat heror should you treat her at all?
Research presented at this years Association for Research in Vision and Ophthalmology (ARVO) meeting offers several possible answers. There were myriad findings on central corneal thickness (CCT), methods to predict a patients risk of developing glaucoma and ways to increase compliance among our patients.
CCT and Age
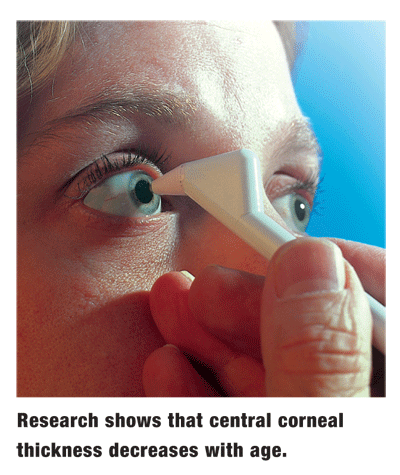 When results of the Ocular Hypertension Treatment Study (OHTS) were released in 2002, we became more aware that CCT impacts IOP measurements. Specifically, a thicker cornea might cause an elevated reading, while a thinner cornea might produce an artificially low reading. OHTS also told us that a thin central cornea itself is one of several risk factors for developing glaucoma.
When results of the Ocular Hypertension Treatment Study (OHTS) were released in 2002, we became more aware that CCT impacts IOP measurements. Specifically, a thicker cornea might cause an elevated reading, while a thinner cornea might produce an artificially low reading. OHTS also told us that a thin central cornea itself is one of several risk factors for developing glaucoma.
Weve assumed that, barring corneal disease, CCT remains the same throughout a patients life. Not so, according to researchers in
These findings emphasize the importance of measuring CCT in patients who are past 40, rather than allowing a normal IOP to lull us into a false sense of security. Although a patients IOP may appear to be normal or even lower than at previous exams, his or her cornea may have thinned with age.
In other findings, there may be an association between thin central corneas and retinal vein occlusions. A retrospective study of 37 patients (42 eyes) who had branch or central retinal vein occlusions found that the mean CCT was 523.25m in the affected eyes and 526.49m in the unaffected eyes.3080 The researchers compared this with a survey of 1,955 eyes, in which the mean CCT was 551.16m.
The association between CCT and both glaucoma and vein occlusion suggests that the trabecular meshwork is involved in both. More research is necessary to better understand the role of CCT in retinal vein occlusions, however.
Glaucoma Prediction
We continue to look for ways to predict who will convert from ocular hypertension to glaucoma. The Diagnostic Innovations in Glaucoma Study looked at whether long-term IOP fluctuations increased a patients risk.851 The researchers evaluated 105 ocular hypertensive patients, 24 of whom developed glaucoma during follow-up, and found that IOP fluctuation between visits was not a risk factor for conversion to glaucoma.
Other findings, however, may help us identify those patients at risk of developing glaucoma. These include:
Biomarkers. Plasma peptide patterns may help predict susceptibility to primary open-angle glaucoma and monitor the effects of treatment.5612 Researchers collected blood from 249 patients with POAG and 138 control subjects and found that the POAG patients had an elevated complement of C4b peptides. Further, mass spectrometry helped researchers correctly predict 96% of the subjects as having POAG or being normal based on peptide profiles.
More research is necessary to determine the significance of this finding. However, a blood test may one day help us predict which patients are likely to develop glaucoma.
Venous pulsation characteristics. These may help predict a patients risk for further cupping, say researchers from
In this study of 76 glaucoma patients and suspects (136 eyes), the researchers found that initial ODF measurement is strongly predictive of a patients risk for further optic disc excavation. Also, the change in ODF is independently associated with increased disc excavation.
Retinal arteriolar narrowing. Previous research has found that retinal arteriolar narrowing may precede the development of open-angle glaucoma (OAG), and the latest findings from the Blue Mountains Eye Study confirm this on a larger scale.3085
Researchers evaluated 2,328 participants who were considered at risk for OAG and measured arteriolar and venular diameters on digital retinal photographs. Seventy-eight participants (99 eyes), or 3.4% of subjects, developed OAG by the five- or 10-year follow-up exam. After adjusting for age and sex, the researchers found that narrower baseline arteriolar and venular diameters were associated with an increased risk of incident OAG. Incidence also increased with each standard deviation decrease in vessel diameter.
But, once researchers adjusted for IOP, use of glaucoma medications, vertical disk diameter, cup-to-disc ratio and baseline disk hemorrhage, the association between arteriolar diameter and OAG became borderline nonsignificant, and the association with narrowed venular diameter was no longer present.
Visual field loss. Researchers looked at three cross-sectional studiesthe Baltimore Eye Survey, the Salisbury Eye Evaluation and Proyecto VERto estimate the rate of worsening visual field damage among patients with OAG.4448 This presentation is significant because it provides comparisons among different groupsnamely white, black and Hispanic patients.
A significant finding: The progression rates of visual field loss are higher in Hispanic patients than they are in white or black patients. As the number of Hispanic patients we see grows, we must keep these findings in mind when treating glaucoma patients. Hispanics comprised one-seventh of the
Treatment Decisions
Once we diagnose the patient with glaucoma, we must decide how to treat the patientor whether to treat the patient at all. In a recent lecture, ophthalmologist George Spaeth said that our goal when managing glaucoma patients is not to reduce IOP or prevent damage to the optic nerve; rather, it is to help the patient go through life without visual disability.
In other words, we must not only consider the patients ocular health, but his or her quality of life. There are times when it might be acceptable not to treat glaucoma if the patient has no significant disability and is unlikely to develop significant disability during the remainder of his or her lifetime. (Of course, you should document this discussion in the patients chart.)
Three studies from Wills Eye Institute in
A second study evaluated how glaucoma patients self-reported quality of life related to their ability to perform tasks of daily living.1181 The researchers asked 194 glaucoma patients, ages 24 to 93, with varying degrees of vision loss to fill out the NEI-VFQ-25. Next, they compared these answers with both clinical measures and scores on the Assessment of Disability Related to Vision (ADREV), which includes such tasks as entering numbers on a calculator, recognizing facial expressions and finding objects in a room. None of the visual tests correlated strongly with the NEI-VFQ-25 scores, but the ADREV scores had stronger correlations. Measures such as ADREV, the researchers say, might be a better way of determining a glaucoma patients quality of life than vision-specific quality of life questionnaires.
A third study found that contrast sensitivity measurement may be more important than other methods when assessing the well-being of glaucoma patients.1607 Using ADREV, the researchers evaluated 194 glaucoma patients and found that each patients contrast sensitivity was closely related to his or her total score. Decreased contrast sensitivity, researchers say, may explain why glaucoma patients have difficulty performing the everyday tasks.
The take-home message from these studies: We should incorporate at least one of these tools to correlate the patients quality of life to his or her stage of visual impairment. The answers will tell us whether treatment will improve that quality of life.
Assuming we go on to treat the patient, just how much treatment should we offer? The Murcia Study suggests that patients are often overtreated.5585 Researchers from
Given these results, we should continually re-evaluate patients, especially new patients, to re-assess treatment. For example, you may have prescribed drops for a patient whose IOP is 25mm Hg only to discover at another visit that the patient has a high CCT. Now, you must ask yourself whether this patient still requires treatment.
Compliance
The success of any glaucoma treatment depends, in part, on patient compliance with medications and follow-up visits. But, results of the Belgian Compliance Study in Ophthalmology suggest that noncompliance may be a more significant problem than we imagined.4335 Of 731 patients who responded to a cross-sectional survey, more than half said they missed doses of their glaucoma medications in the previous two weeks; 39.7% missed one or more doses, and 12.3% missed two or more. Significantly more male patients and younger patients were noncompliant. Also, patients who had a higher number of daily doses of medication were more likely to be noncompliant.
These findings emphasize the importance of screening for compliance and finding ways to help patients adhere to their medication and follow-up schedules. For example, we might switch to drops that require once-daily dosing or combination drops when clinically appropriate.
A multifaceted intervention, including a motivational/educational video and visit reminders, may help improve compliance with follow-up visits, say researchers from Bascom Palmer Eye Institute in Miami and Johns Hopkins University in Baltimore.5577 When comparing 27 glaucoma patients who received such interventions with 10 patients who did not, those who received the interventions were much more likely to comply with follow-up appointments (23 out of 27, or 85%) than those who did not (seven out of 10, or 70%). Patients who had intervals of two months or less between visits also were more likely to keep appointments than those with an interval of more than two months (92% vs. 71%). A large-scale test is necessary to see whether intervention can produce and sustain better compliance rates for glaucoma visits, the researchers say.
Selective Laser Trabeculoplasty
One study compared the effectiveness of SLT when used following different types of glaucoma agents.3983 In a retrospective chart review of 203 eyes of patients treated with SLT over four years, its effectiveness at reducing IOP was greatest with carbonic anhydrase inhibitors or alpha-agonists. This was followed by beta-blockers. SLT had the least effect with prostaglandins. Further study is necessary, however, to evaluate the higher-order interactions seen in combination therapy.
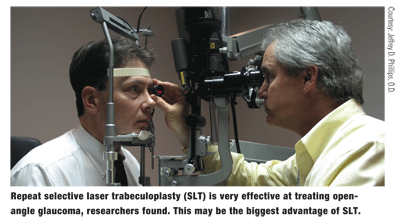
Meanwhile, researchers found repeat SLT to be very effective for treating OAG.3972 This, perhaps, is the biggest advantage of SLT. In this study of 29 patients with OAG, the procedure lowered IOP to 18mm Hg or less in 84% of eyes at three months following primary SLT treatments, 71% of eyes at six months, 64% of eyes at nine months and 59% at 12 months. Repeat SLT lowered IOP by 3mm Hg in 90% of eyes at three months, 81% of eyes at six months, 69% at nine months and 64% at 12 months. In both instances, results were achieved with no additional glaucoma medications, laser treatment or glaucoma surgery.
Dr. Cole is in private practice in
851. Medeiros FA, Ng D, Zangwill LM, et al. Long-term intraocular pressure fluctuations and risk of conversion from ocular hypertension to glaucoma.
1181. Richman J, Lorenzana L, Spaeth GL. The relationship between quality of life with disability and various aspects of reduced vision in patients with glaucoma.
1565. Warrian KJ, Lorenzana LL, Spaeth GL. Quality of life and the spectrum of glaucoma.
1607. Batiste CG, Lorenzana LE, Spaeth GL. Decreased contrast sensitivity is associated with increased disability in patients with glaucoma.
2879. Morgan WH, Balaratnasingam C, Hazelton ML, et al. Venous pulsation characteristics are predictive of increased optic disk excavation independently of intraocular pressure.
3080. Lee JK, Viriya E, Madu A, Mian U. Thin central corneal thickness: risk factor for retinal vein occlusions.
3085. Taylor B, Wang J, Rochtchina E, et al. Does retinal areteriolar narrowing precede the long-term development of open-angle glaucoma: Blue Mountains Eye Study findings.
3972. Mequio MJ, Hughes BA, Juzych MS, et al. Efficacy of repeat selective laser trabeculoplasty.
3983. Jindra LF, Gupta A, Miglino EM. Comparison of class of pre-procedure glaucoma monotherapy and effectiveness of selective laser trabeculoplastey.
4332. Lin N. Central corneal thickness (CCT) decreases with age.
4335. Vandenbroeck S, Dobbels F, Stalmans I, et al. Non-compliance, the blind spot in glaucoma treatment: results from the Belgian Compliance Study in Ophthalmology.
4448. Broman AT, Katz J, Munoz B, et al. Estimating the individual rate of progressive visual field loss among subjects with open-angle glaucoma in population-based cross-sectional studies.
5577. Ramulu P, Quigley HA, Friedman DS. A randomized controlled trial to increased compliance with glaucoma follow-up visits.
5585. Villegas-Perez MP, Calzado-Hinojosa J, Ortiz-Gomariz A, Miralles de Imperiral J. Overtreatment of glaucoma: the Murcia Study.
5612. Ng K, Crabb JS, Gu X, et al. Glaucoma biomarker discovery.

