 |
Q: I have a long-time contact lens patient who recently developed neovascularization and corneal haze. Could this be limbal stem cell deficiency?
A: “It absolutely could be—but it’s not necessarily one of the first things to consider,” says Will Smith, OD, of Advanced Vision Care in Los Angeles.
For instance, superior limbic keratoconjunctivitis (SLK) can have a similar appearance. “The way to differentiate between SLK and limbal stem cell deficiency is that SLK will stain with both fluorescein and lissamine green, but limbal stem cell deficiency will not stain with lissamine green,” he says.
Why? It has to do with the disease itself, Dr. Smith explains. In limbal stem cell deficiency, something goes wrong with the stem cell development process in the limbus—instead of becoming avascular corneal cells, the limbal stem cells develop as conjunctival cells, producing that neovascular and hazy appearance on the cornea. The etiology of the problem can be congenital (e.g., aniridia), acquired (e.g., chemical or thermal burns) or inflammatory (e.g., Stevens-Johnson syndrome).
In any event, lissamine green stains damaged and dead epithelial cells, as in SLK. But the cells in limbal stem cell deficiency are not damaged—they’re simply in the wrong location, so they won’t automatically stain with lissamine green.
Also, be sure to rule out infectious causes. Dr. Smith relates the case of a patient referred to his office with a presumed diagnosis of interstitial keratitis, which is generally due to a systemic inflammatory disease such as syphilis. “But other bacterial infections—such as tuberculosis, Lyme, even parasitic infection like Acanthamoeba—should be considered, too. In such cases, order lab work to rule out these causes,” Dr. Smith says.
In his patient’s case, the lab work showed that she did not have interstitial keratitis. Instead, a whorled keratopathy pointed to a different etiology.
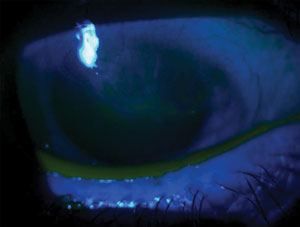 | |
| A whorled, vortex-like keratopathy is a clue to a limbal stem cell deficiency. |
Generally, the diagnosis of limbal stem cell deficiency is made clinically, Dr. Smith says. It’s often characterized by a whorling, vortex pattern on the cornea—which was indeed the case in this patient with presumed “interstitial keratitis.”
If you wish to confirm the clinical diagnosis, the gold standard test is corneal impression cytology, in which filter paper is placed on the patient’s anesthetized eye, then removed and sent off for histological analysis, Dr. Smith says.
Discontinue contact lens wear immediately. Contact lenses, especially for high myopes, can sit heavily on the limbus, which can foster hypoxia and mechanical irritation. (Indeed, contact lens wear can be one of the causes of limbal stem cell deficiency.)
Treatment involves maximum-strength, preservative-free anti-inflammatory therapy, such as preservative-free dexamethasone 0.1% or preservative-free prednisolone acetate 1% suspension, which must be ordered through a compounding pharmacy. Start at QID for one week, then BID for as long as necessary until the inflammation resolves.
Improvement will be slow. “I wouldn’t expect to see a whole lot of difference until about a month out,” Dr. Smith says. “We’ve had patients whose inflammation didn’t start regressing for four months.”
Upon resolution, vision usually returns to normal, although pannus and ghost vessels may remain on the cornea. If the patient wishes to return to contact lens wear, reconsider the lens modality, Dr. Smith says. Try a gas permeable lens or a scleral lens that vaults the limbus.
If the patient doesn’t improve, or if the disease is already severe, consider a referral to an anterior segment specialist who is familiar with the surgical option of limbal stem cell transplantation.
In either case, follow these patients closely, as limbal stem cell deficiency often recurs, Dr. Smith says.
