
All across the country, optometrists and ophthalmologists alike are making the effort to ensure that patients who need eye care receive it. Be it through a chapter of VOSH or through an NEI-funded study, eye-care practitioners are serving their patientsand raising the cry for others to help as well.
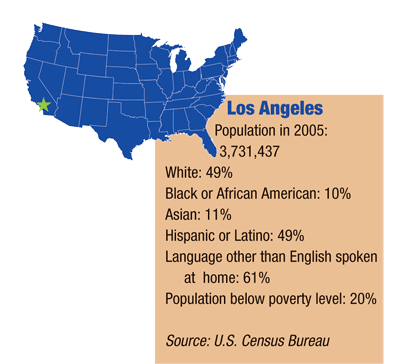 Los Angeles
Los Angeles
When ophthalmologist Rohit Varma first arrived in
Once settled in his new home, Dr. Varma started asking questions about issues such as the major causes of blindness for
So, Dr. Varma and his colleagues applied for a grant from the National Eye Institute for studying eye disease in the Latino population. The study was funded in 1999, and so began the Los Angeles Latino Eye Study (LALES), the most comprehensive and largest research project regarding eye disease in Latinos to date in the country.
Today, Dr. Varma, director of the ocular epidemiology center at the
What was equally surprising was that between 70% and 90% of these conditionsincluding diabetic retinopathy, open-angle glaucoma and age-related macular degenerationhad not been previously diagnosed; those patients in the study were unaware that they had eye disease.
Such findings from recent studies, like LALES and the Ocular Hypertension Treatment Study, clearly indicate that minority populations may be predisposed to certain eye care disease and conditions. And, since minority populations are expected to continue to experience rapid growth in the U.S. (see A Snapshot of Minority Populations in the U.S., below), the question for many is two-fold: Are optometrists doing enough now to serve these populationsand, will O.D.s be able to catch up and meet their needs in the future?
Whether in private practice or an academic setting, some O.D.s are making it a priority to heighten their awareness in serving the needs of this minority patient base. Others have dedicated their professional careers to working with minority patients, while still others volunteer in inner city clinics, homeless shelters or rural areas to provide vision services to the underserved and minority groups.
Despite the efforts, many say there is still much work to be done. All eye care providers need to do a lot more, Dr. Varma says.
LALES included more than 6,300 Latinos (primarily Mexican-Americans) age 40 and older from the
The study found that:
Latinos living in the
Many do not know that they have these conditions; one patient in five was newly diagnosed during the exam.
Almost half of Latinos with diabetes have diabetic retinopathy.
Of those with any signs of age-related macular degeneration, only 57% reported ever visiting an eye-care practitioner. Only 21% did so annually.
Of Latinos with glaucoma and ocular hypertension, 75% were undiagnosed before participating in the study.
Because vision loss can often be reduced with regular eye exams and treatment, Dr. Varma recommends implementing culturally appropriate programs to detect and manage eye disease in this population. This is especially important for Latinos as a whole, since they have a high prevalence of low vision, diabetic retinopathy and glaucoma, as demonstrated by LALES.
Some of the most important outcomes of LALES are that Medicare changed the screening benefit rule and added Latinos as a high risk group that could receive the benefit of a glaucoma screening, Dr. Varma says. But, he warns that the vision communityboth optometrists and ophthalmologistsstill needs to be educated on specific eye diseases. They are more likely to screen, and they are more likely to detect and treat it, he said.
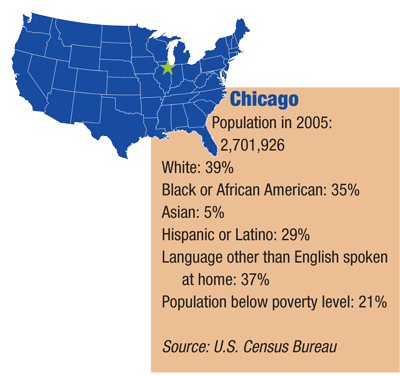
Chicago
As the principle investigator of the Illinois College of Optometrys Pediatric Outreach Program, optometrist Valerie Kattouf has spent much of her professional life providing comprehensive vision care to high-risk children. Dr. Kattouf leads a team of optometrists and students in partnership with early intervention programs throughout
Two-thirds of the children she sees are insured through Medicaid; the rest are uninsured. Dr. Kattouf sees children of many racial backgrounds. A good deal of the children I see are immigrants, she says. Whatever their ethnic makeup, many need treatment for vision concerns, she adds.
Dr. Kattouf recalls seeing one Indian boy who was not wearing glasses when she examined him. She found that he was a high hyperope (+8.00D). He was a very sweet boy, she notes. But, he was not attentive, and he was all over the place. His teachers said he was difficult in the classroom. His teachers and parents reported a dramatic improvement in his attention and behavior after he received the glasses. Vision problems such as these often go undetected because kids are quite adaptable and often exist in a state of blur, she says.
Dr. Kattouf has seen this happen repeatedly. One mother told Dr. Kattouf that she had difficulty controlling her very aggressive son. Upon examination, Dr. Kattouf found that he had high uncorrected myopia (-16.00D). When I put the glasses on him, he immediately relaxed, she recalls. He looked at me and said, Please dont take these glasses off.
Dr. Kattouf spearheaded the program in 2003; it was developed in response to the World Health Organizations efforts to eliminate preventable blindness by 2020 and the U.S. Department of Health and Human Services Healthy People 2010. She estimates that it has helped approximately 3,400 children. Of these, 18% need a refractive correction, which is a higher percentage than the average population, Dr. Kattouf says.
Whether optometrists decide to make a commitment to work with minority and underserved populations is a personal choice, Dr. Kattouf says. I think, though, that it is important that optometrists are aware that different populations have different needs, she adds.
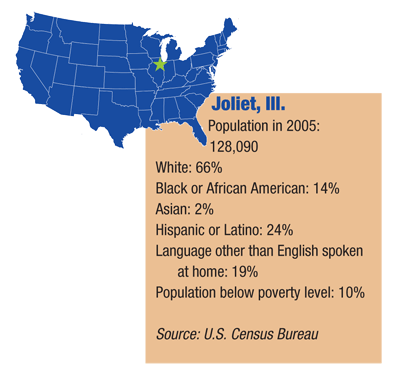 Joliet, Ill.
Joliet, Ill.
James R. Sanderson, O.D., is in private practice in the
The desire to help those in need in his own community hit home for Dr. Sanderson while working with his church group in a shelter in
Expanding on the clinic started by optometrist Sol Rocke at Pacific Gardens Mission, he and a group of optometrists and volunteers set up one-day clinics six times per year in
VOSH, Dr. Sanderson says, is his way of giving something back. He knows the time commitment it takes to volunteer, especially during overseas VOSH missions. While he uses his own vacation time and pays his own way for the trips, he knows the sacrifice this can be for others. Yet, he sees the need and knows more needs to be done to serve the underserved and minority populations in the country.
The working poor and underservedand especially the immigrant populationwill do nothing but grow, he says. The need for eye care is there. It is up to us to provide these groups with the basic eye care that they need.
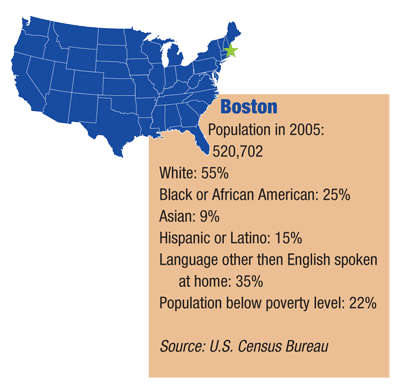 Boston
Boston
For over two decades, Roger Wilson, O.D., has been involved in community health partnerships as a clinician, educator, health services researcher and administrator. Today, Dr. Wilson is the vice president for Health Center Programs for the New England Eye Institute (NEEI), the clinical teaching arm of the New England College of Optometry, and the chair of the AOA Community Health Center Committee.
His passion for community health began in the Boston area more than 20 years ago, when he began his hands-on experience by serving underserved populations; minorities; the frail, disabled and elderly; and other members of Bostons diverse neighborhoods. I like to say that community health center optometry is where I grew up professionally, Dr. Wilson says. I began to understand the needs of communities and began to understand what vulnerability really meant.
The NEEI is a network of more than 40 eye care centers and programs that collectively receive approximately 75,000 visits a year. Such community collaborations are considered a unique national model, so the NEEI is playing a key role in the National Institute of Healths Healthy People/Healthy Vision 2010 national health agenda.
Also, students who participate in these clinical programs receive community-based health care training each year at the college. Through these affiliations, we are preparing optometrists to successfully practice in any modality, Dr. Wilson says. There is a misconception that community-based programs only teach students about treating the underserved and needy. Nothing is further from the truth, he stresses. Our students also learn about the best practices, compliance issues and how to be part of a front-line care-management team.
Community health settings also teach students about the social issues that impact the lives of their patients and provide them with the necessary tools that they will need to be successful in practice.
Also, Dr. Wilson explains, many patients cared for by the NEEI affiliates are far below the federal poverty level. You expect that, if people dont have good access to health care, the presenting health conditions are going to be more prevalent and more severe than in an uninsured population, he says. For example, we see more cases of diabetic retinopathy, glaucoma and cataracts. In children, we see more cases of uncorrected refractive errors, strabismus and amblyopia.
The clinics also care for people from diverse racial and ethnic backgrounds. So many languages are spokenespecially at community health centersthat students and staff doctors receive training in cultural competence. I cant say that every optometrist should get involved (in community-based health care), Dr. Wilson says. But, what I can say from experience is that I am a better optometrist, having been a part of our remarkable model of eye care delivery.
 New Orleans
New Orleans
When Hurricane Katrina slammed into the
In
Optometrist Victoria Weiss left her
During one of their volunteer trips to
When Dr. Weiss is not busy in her private practice or volunteering in nursing homes, she works with the
Volunteering in this country is less expensive and requires less time off from work than you would think, Dr. Weiss says. It is not as hard as you might expect; its a good experience to see people who really need your help and are from your own country and really appreciate your services.
 Bloomington, Ind.
Bloomington, Ind.
Edwin Marshall, O.D., is not a fan of the across the room diagnosis. The professor and associate dean for academic affairs and student administration at the Indiana University School of Optometry is an advocate of cultural competency. He urges all practitioners not to make assumptions of the individuals they treat based on appearance.
Take his mother, for example. Dr. Marshalls mother is an older African American retired school teacher who had to find a new general practitioner after a recent move. After seeing her new physician, she called her son to say that the doctors were different from where she came from, and the new practice didnt do as many tests as her previous practitioner.
After being encouraged by her son to ask more questions, his mother went back to her new doctor and asked about the low number of procedures. The physician responded that he would only do what Medicare paid for. After responding that she had money to pay for what Medicare would not cover, additional tests were done, only to find that she had polyps. Luckily, they were discovered early, and the physician was able to intervene in an appropriate and timely manner.
The doctor made an assumption, an across the room diagnosis that she is an African American female on Medicare, so she probably couldnt afford anything else, Dr. Marshall says.
Dr. Marshall has spent his professional career shining the light on issues such as cultural competency and access to care. He is the founding chair of the minority health advisory committee of the Indiana State Department of Health, past president of the Indiana Optometric Association and the Indiana Public Health Association, and a member of the Indiana Diabetes Collaborative.
His passion to provide greater access to care for minority and underserved populations led him to spearhead a program six years ago in
As we look at populations at risk, their growth and the health conditions under which they suffer are going to explode, Dr. Marshall says. We need to address the problems of the underserved a lot more effectively than we have done in the past.

Focus on the Future
As studies such as LALES have indicated, different minority populations are more prone to certain vision problems and diseases. And, both minority and underserved populations are expected to grow significantly over the next few decades. So, the question remains: Will optometrists and other health care providers be able to keep up?
There is a lot of back-and-forth on whether ophthalmologists or optometrists should treat certain conditions, Dr. Varma says. This battle is completely misplaced. If you find that 70% to 80% of a population has conditions that are previously undiagnosed, why is there a battle over the 20% to 30% who are already in the eye care system? Why arent there more programs to screen more persons so that we can bring the 70% to 80% who have undiagnosed treatable eye disease into the eye care system?

