Today, we follow a medical model designed specifically to facilitate the day-to-day management of glaucoma patients in an optometric setting. The transition into the medical model was a natural process that resulted from rudimentary changes in the core educational curriculum at optometry schools across the country, as well as various legislative activities in each state and the incorporation of optometric medical services into third-party payer systems.
For those of you who are well versed in the management of glaucoma and/or already have a large glaucoma patient base, you can stop reading here; you’ve already learned what it takes to develop this segment of your practice.
But, for those readers who are interested in developing a glaucoma specialty practice, or are at least interested in incorporating more glaucoma patients into your practice, keep reading. Here, I’ll outline what I believe are the necessary steps to build a large, successful glaucoma practice.
Three Important Pieces
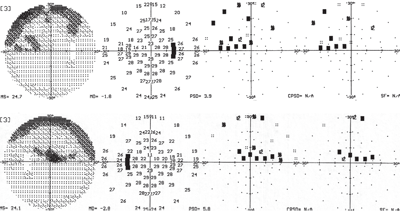
Any practitioner who intends to
establish a glaucoma specialty practice should purchase a conventional
white-on-white perimeter to help detect and track field loss.
To develop and manage a successful glaucoma practice, a clinician must:
• Show excellent clinical acumen.
• Secure appropriate office space and diagnostic technology.
• Effectively communicate with patients.
Let’s explore these three essential elements in greater detail.
Clinical Acumen
It almost goes without saying––in order to manage a disease process effectively, you must be well versed in all aspects of that disease. In most cases, mastery of such material begins in optometry school and continues throughout your career and attainment of continuing education credits.
But, there are several other ways you can expand your clinical knowledge and experience. For example, you can become a Fellow in the American Academy of Optometry or attend a glaucoma-specific symposium, such as the Optometric Glaucoma Society annual meeting. However, one of the best (and most underutilized) resources for information and research on glaucoma is your fellow colleagues.
Spend time in the offices of both ophthalmologic and optometric colleagues. While many of us would likely be comfortable “shadowing” an ophthalmologist, the same
cannot necessarily be said for a fellow optometrist. Keep in mind, however, that a fellow optometrist who already specializes in glaucoma management will more than likely be able to provide you with tremendous perspective in all aspects of establishing the groundwork for the development of a successful glaucoma practice. We’re talking about not only the medical decision-making process, but also about insights and suggestions that you won’t hear from an ophthalmologist, such as how to retain a glaucoma patient’s care in an optometric practice.
Visit fellow O.D.s who have large glaucoma practices. Ask them how they developed that practice. Ask them how long it took. Ask them what they believed was their biggest mistake in developing that practice. And, most importantly, ask them about the specific challenges to growing and maintaining their patient base. Their answers will be absolutely invaluable.
Technology and Office Requirements
If you’re in the early stages of developing a glaucoma practice, calculating your necessary equipment costs can be a daunting task.
At just about every major optometry conference, clinicians present glaucoma cases that rely heavily on visual field studies, imaging technologies and other specialized testing. Additionally, there are multiple versions of these diagnostic instruments as well as software packages that, when used collectively, help make a management plan easy to generate.
But, all these tools can easily overwhelm an inexperienced practitioner, and make him or her ask, “How can I afford all those instruments?” Clinicians in private practice, like myself, are constantly faced with the financial ramifications of incorporating new technologies. Often, this step may lead some clinicians to believe that the investment in equipment is far too expensive for the (at least initially) small number of glaucoma patients and that it won’t pay for itself in a reasonable amount of time.
The truth is, you can begin to develop your glaucoma practice without all the bells and whistles. There are many studies that attest to the validity and limitations of cutting-edge visual field instruments and imaging technologies.1-3 Keep in mind that most of these advanced imaging technologies have been in standard use for just 15 to 20 years or less. Those of us who have been in practice for more than 25 years can attest to the fact that you can have a successful glaucoma practice without all of those instruments. While they can assist us in making a diagnosis and creating a management plan, it is ultimately our clinical judgment that we base our treatment options upon.
That said, you must have a few pieces of equipment to offer an appropriate level of initial care:
• Tonometer. Fortunately, most clinicians have a tonometer. Goldmann applanation tonometry (GAT) has been the standard of glaucoma care for many years. While there are limitations to GAT, it does give us a reasonable idea of one of the most varied of all risk factors––intraocular pressure. Though non-contact tonometers may facilitate quicker patient interaction, I think that a Goldmann tonometer is a “must have” in any glaucoma practice.
• Slit lamp. Secondly, a good slit lamp lens is crucial for close inspection of the optic nerve. While there is tremendous debate among glaucoma experts concerning structural vs. functional change, the reality is that glaucoma causes characteristic damage to the optic nerve that is visible at the slit lamp. Close scrutiny of the neuroretinal rim, optic cup, retinal nerve fiber layer and retinal vasculature are critical in optic nerve evaluation.
There are several slit lamp lenses to choose from, and it doesn’t really matter which specific lens you select. The bottom line is that you must consistently use the same lens when evaluating all your patients, because each lens has different characteristics that may change the overall appearance of the optic nerve.
• Pachymeter. Since the results of the Ocular Hypertension Treatment Study (OHTS) were published in 2002, measurement of central corneal thickness has become the accepted standard in evaluating both glaucoma suspects and established glaucoma patients.4 Accurate and portable pachymeters are commercially available, so one instrument can serve the entire office. Though reimbursement is generally low for corneal thickness testing, a pachymeter is another “must have” device.
• Perimeter. In regard to visual field testing, an abundance of data highlights typical patterns of visual field loss associated with glaucoma.5-7 For many years, conventional white-on-white (WOW) perimeters, such as the Humphrey Field Analyzer (HFA, Carl Zeiss Meditec), have served as the workhorse of many glaucoma practices.
More recently, selective perimetry has been proven to detect early visual field defects in glaucoma patients much sooner than WOW perimetry. Such selective perimeters as the Humphrey Matrix Perimeter (Carl Zeiss Meditec) and the Heidelberg Edge Perimeter (HEP, Heidelberg Engineering) have been shown to reveal subtle defects earlier in the disease process.8
You don’t need advanced imaging
equipment to start a glaucoma practice. In fact, simple stereo
photography is one of the most effective ways to predict glaucoma risk.
So, what perimeter should a practitioner first get to facilitate the development of a large glaucoma practice? While selective perimeters do locate visual field defects earlier, I believe that each practitioner should purchase at least one conventional perimeter first—then add a selective perimeter in the future, when funding permits. While many practitioners with large glaucoma practices may disagree with this opinion, a WOW perimeter has several uses beyond glaucoma. For example, a conventional perimeter can be used to evaluate neurological field loss, acute optic nerve field loss and macular disease. In other words, it not only works well for glaucoma, but also can be widely used in general practice.
WOW perimeters may not detect the earliest glaucoma field defects, but they do find glaucomatous defects. Close analysis of the optic nerve at the slit lamp in conjunction with a perimetric study can yield a significant amount of data, which will help you confirm a diagnosis of glaucoma.
While the physical layout of most optometric practices meets the requirements necessary for successfully managing glaucoma, you should, however, have a room dedicated to visual field measurement. Sometimes, obtaining accurate visual fields is an arduous process for both the patient and the eye care professional performing the field study. In my experience, having the perimeter in an area with a lot of noise and distractions is frustrating for the patient. Having a quiet, tranquil place to obtain the visual field can make an unpleasant task seem much less frustrating.
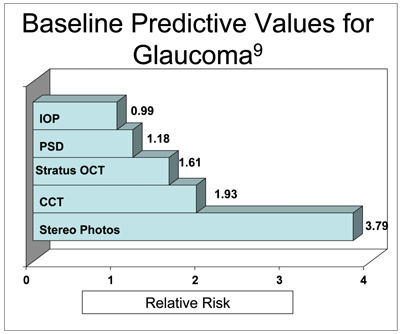
• Digital camera. One of the most important imaging devices for a developing glaucoma practice is a digital camera. While most lectures showcase optical coherence tomography (OCT) or Heidelberg Retinal Tomography (HRT, Heidelberg Engineering) imagery, a simple, digital stereo photograph of the optic nerve is very useful in following disease progression. In fact, one of the OHTS ancillary studies indicated that stereo photography was four times more reliable than IOP measurement and more than twice as reliable than a baseline OCT scan in predicting which patients will develop glaucoma (see “Baseline Predictive Values for Glaucoma”).9
Digital stereo photography is important in not only initially capturing 3D characteristics of the optic nerve, but also in being able to follow the nerve over time to assess its stability. While digital images do not necessarily quantify optic nerve characteristics, they are valuable in assessing qualitative features of the optic nerve. And, digital photographs ideally complement a physical examination of the optic nerve.
• Advanced imaging technology. Invariably, any conversation about necessary technology for a successful glaucoma practice will include a discussion about advanced imaging technologies, such as OCT, HRT and/or scanning laser polarimetry (GDx Nerve Fiber Analyzer, Carl Zeiss Meditec).
These devices are very expensive, however, and they may be well outside the budget of a developing practice. Does this budgetary constraint mean that the practitioner should not treat glaucoma? Or worse yet, should the practitioner overextend himself into extreme debt to obtain such technology? No!
Nonetheless, as your practice grows and your patient base increases, you may wish to purchase a GDx, OCT or HRT. While GDx imaging is useful in the context of glaucoma, it has limited use in other posterior pole diseases, whereas OCT and HRT both have applications for optic nerve and macular diseases.
Patient Communication
Being able to communicate effectively with your patients is crucial to their long-term management as well as the long-term growth of your practice.
You have to look at the entire diagnosis of glaucoma, including the treatment process, from the patient’s perspective. To them, they have a potentially blinding disease. Their visual outcome rests squarely in your hands. While the actual management of chronic open angle glaucoma is not as dramatic as that portrayal—to the patient, it is.
This is a medical problem now, not an optical problem. At first glance, does your office convey a “medical” feel or an “optical sales” feel? How medically skilled does your staff appear to your patients? These are important issues, especially if a patient has been coming to a specific location for many years and sees it only as a place to pick up a pair of glasses.
To give you some perspective, think about what your primary health care provider’s office looks like and how his or her staff appears. Though it is not necessary to have a “sterile” (or boring) office appearance, heavily sales-oriented practices have greater difficulty making the transition to medically-oriented practices.
This is another reason why it’s particularly beneficial to visit optometric colleagues who have large glaucoma practices. See how they do it. Look at their staff. In particular, observe their techs—how do they dress and speak?
While the non-verbal communication of your office and staff is important, it pales in comparison to the verbal and non-verbal communication from you, the practitioner. While everyone’s chairside manner is different, you simply must gain the patient’s trust the first time any mention of glaucoma is made. Once the patient trusts you, he or she will follow your recommendations, be more compliant, stay with your practice and tell others about your services.
But, here is where it can become somewhat dicey. When glaucoma patients tell someone close to them that you are treating their vision-threatening disease, and that someone then eventually finds their way to your practice, everything is good. However, if a patient tells someone that you are treating his or her glaucoma, and that other person recommends that the patient see a “specialist,” he or she could suddenly experience a feeling of uneasiness. And, that uneasiness could make the patient less likely to return.
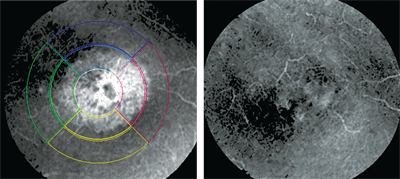
Once your practice is well established and funding permits, you may consider purchasing an advanced imaging device, such as an HRT-3.
If, however, the patient thinks back to the initial visit with you and the trust you established, he or she may be less likely to leave your practice. The patient may indeed seek a second opinion, but he or she will still have emotional ties to your office.
Without question, one of the more common mistakes new glaucoma practitioners make is the manner in which they explain a diagnosis to a patient. While trying to be compassionate, an inexperienced clinician may say, “Well, Mrs. Jones, I think that you may have glaucoma.” The patient heard two things: “think” and “may.” In other words, the patient might believe that you have no idea what is wrong. And, while you may not yet have all the diagnostic puzzle pieces in place, you must concentrate on the known facts.
So, be sure to say something like, “Mrs. Jones, preliminary testing indicates that you have some risk factors for glaucoma development, and you will need to return to the office within the next few weeks for further evaluation.” There is no need to explain the situation as if you’re justifying your internal thought process. You’re simply explaining what’s wrong with the patient and what steps you’ll take to solve the problem. Black and white, cut and dry. Sensitive, yet professional. Mrs. Jones has the risk factors; you are the messenger. She may be anxious about the news, and you can listen compassionately, but that doesn’t change the fact that she presented to you with a series of problems that puts her at risk.
There is a fine line between sounding confident and coming across as arrogant and defensive. A confident clinician lays out the problems in an understandable fashion and clearly explains the determined plan of action. Give the patient enough information to get the point across, period. Too much information overwhelms the patient and can make you sound as though you’re defending your thought
process.
A confident and experienced doctor will not sound defensive, aloof or distant, but simply direct and certain. Remember: Learning to choose your words and convey your thoughts appropriately will require practice and experience.
One thing that I often do during the initial discussion with particularly nervous patients who are at risk for developing glaucoma is put my hand on top of theirs and speak directly to them while looking into their eyes. Physical touch and eye contact portrays not only compassion and concern, but also firmness and confidence.
If a patient ultimately wants a second opinion, I encourage him or her to do so. I’ll make recommendations to ophthalmologic colleagues whom I believe will best handle the patient. I know in advance who those colleagues are and how they view optometric management of glaucoma. I always tell these patients that I understand their desire to get that second opinion and that “I encourage second opinions, because if both the first and second opinions are correct, both providers will come to the same medical conclusion.” This gesture, in turn, bolsters the patient’s confidence in you—the provider of the first opinion—once the second opinion is rendered.
When the patient returns for his or her subsequent work-up and the testing is completed, I enter the room and ask the patient why I asked them to return.
The patient’s answer gives me a feel for how much he or she understands about what is happening and, in turn, shows the patient that I want him or her to know what is going on.
Repetition, consistency and continuity of care visit-after-visit add to the patient’s sense of confidence in you and your office. Patients like being comfortable with their doctor. Once they’re comfortable with your care, they’ll be your patients for the long run.
But, once they become your patient for the long run, it is your job to then watch them closely and monitor their condition. Give them a heads-up that their medications may need to be changed. Inform them that they may be facing surgery. Offer them reassurance. Give them confidence. Provide them with expert care.
If you can do all of these duties successfully, you’ll look around one day and find that you have a successful glaucoma practice.
Dr. Fanelli is the president and clinical director of Fanelli Eye Associates, a glaucoma specialty practice in Wilmington, N.C. He is the author of Review’s “Glaucoma Grand Rounds” and has specialized in glaucoma care for 25 years.
1. Oddone F, Centofanti M, Iester M, et al. Sector-based analysis with the Heidelberg Retinal Tomograph 3 across disc sizes and glaucoma stages: a multicenter study. Ophthalmology. 2009 Jun;116(6):1106-11.e1-3.
2. Mwanza JC. Reproducibility of peripapillary retinal nerve fiber layer thickness and optic nerve head parameters measured with Cirrus HD-OCT in glaucomatous eyes. Invest Ophthalmol Vis Sci. 2010 Jun 23. [Epub ahead of print]
3. Alencar LM, Zangwill LM, Weinreb RN, et al. A comparison of rates of change in neuroretinal rim area and retinal nerve fiber layer thickness in progressive glaucoma. Invest Ophthalmol Vis Sci. 2010 Jul;51(7):3531-9.
4. Gordon MO. The Ocular Hypertension Treatment Study: baseline factors that predict the onset of primary open-angle glaucoma. Arch Ophthalmol. 2002 Jun;120(6):714-20.
5. Li SG, Spaeth GL, Scimeca HA, et al. Clinical experiences with the use of an automated perimeter (Octopus) in the diagnosis and management of patients with glaucoma and neurologic diseases. Ophthalmology. 1979 Jul;86(7):1302-16.
6. Flammer J. Quantification of glaucomatous visual field defects with automated perimetry. Invest Ophthalmol Vis Sci. 1985 Feb;26(2):176-81.
7. Arnalich-Montiel F. Performance of glaucoma progression analysis software in a glaucoma population. Graefes Arch Clin Exp Ophthalmol. 2009 Mar;247(3):391-7.
8. Giuffrè I. Frequency doubling technology vs. standard automated perimetry in ocular hypertensive patients. Open Ophthalmol J. 2009 Mar 24;3:6-9.
9. Lalezary M, Medeiros FA, Weinreb RN, et al. Baseline optical coherence tomography predicts the development of glaucomatous change in glaucoma suspects. Am J Ophthalmol. 2006 Oct;142(4):576-82.

