Several treatments have been proposed and attempted for retinal artery occlusion (RAO), but none have been shown to be both effective and safe. In a new study in British Journal of Ophthalmology, researchers assessed the efficacy and safety of a standardized hyperbaric oxygen therapy (HBOT) protocol monitored by fluorescein angiography (FA) in patients with RAO and found it indeed to be safe and effective, with patients achieving a significant best-corrected visual acuity (BCVA) improvement.
 |
|
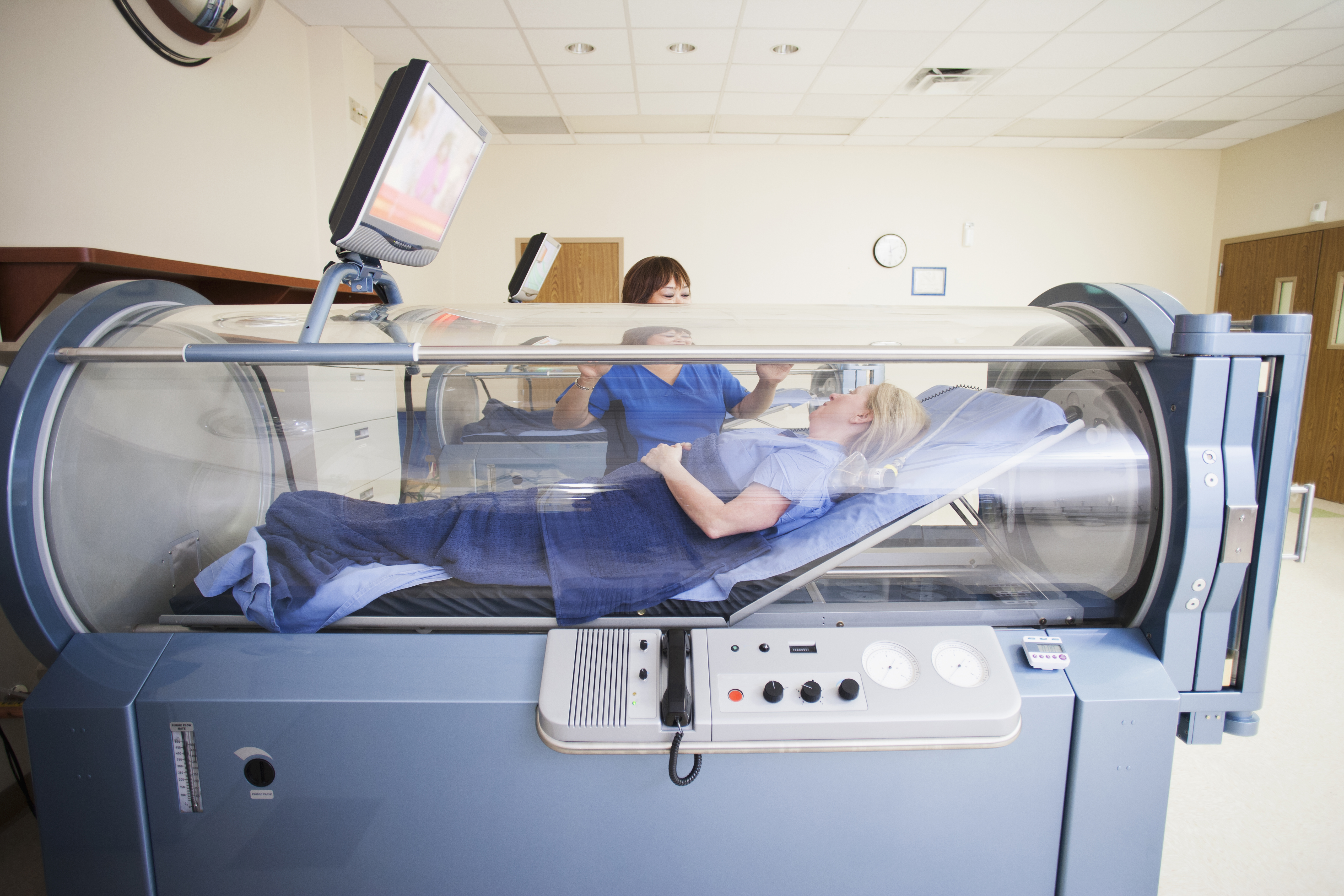
While time-consuming and intimidating to some, hyperbaric oxygen therapy was found to be a safe and effective method for improving visual outcomes in RAO patients. Photo: Getty Images. |
A total of 31 patients diagnosed with RAO within seven days underwent visual acuity measurement, FA, macular OCT and OCT angiography. They received two daily HBOT sessions (2.5 atmosphere absolute at 90 minutes) until revascularization assessed by FA. Follow-ups were scheduled at day 14, day 21 and one month. The main outcome measure was a BCVA improvement defined as a decrease ≥ 0.3 logMAR at one month, which was found in 48.4%, 52.6% and 41.6% of RAO, CRAO and BRAO patients, respectively. The use of antiplatelets and a poor initial BCVA were significantly associated with a gain ≥0.3 logMAR.
“Monitoring patients with FA to determine HBOT duration allows customizing treatment with good results despite late referral up to seven days after the onset,” the authors wrote in their paper. “About half of our patients achieved a significant BCVA improvement (≥0.3 logMAR), a higher proportion than without treatment (natural evolution of the disease).”
Based on the underlying pathophysiology that HBOT is thought to oxygenate the inner retinal layers through a passive diffusion from the underlying choroid and vitreous body, the authors decided to continue HBOT until revascularization of the central retinal artery.
“We hypothesized that two daily sessions had the advantages to provide (1) an immediate oxygenation of the retina via the choroidal vasculature and (2) a progressive retinal oxygenation through the vitreous body that could be considered as an oxygen reservoir allowing a slow and progressive release of the accumulated oxygen,” the authors explained in the article. “We assumed that the high number of sessions and the use of two daily sessions could explain why our results are similar to those of previous studies despite the inclusion of patients with symptoms for >12 hours (about two-thirds of our patients).”
No serious adverse events occurred, with only six patients experiencing minor barotrauma for which HBOT discontinuation was not required. Additionally, an association was found between the use of antiplatelets on referral and a better visual improvement.
“Although not recognized as a standard of care for CRAO, antiplatelets are widely prescribed for the secondary prevention of cardiovascular events,” the authors noted. “Here, we hypothesized that the use of antiplatelets could be associated with a smaller thrombus size, thus allowing better residual arterial flow and hyperbaric oxygenation of the inner retinal layers.
“Patients presenting with RAO should benefit from prompt HBOT whenever possible to maximize visual acuity gain,” the authors concluded.
Chiabo J, Kauert A, Casolla B, et al. Efficacy and safety of hyperbaric oxygen therapy monitored by fluorescein angiography in patients with retinal artery occlusion. Br J Ophthalmol. August 17, 2023. [Epub ahead of print.] |

