 A 79-year-old white female was referred for evaluation of a lesion in her right eye. The patient noted blurred vision in both eyes, which her primary-care doctor attributed to cataracts. However, her doctor discovered a suspicious yellow lesion in her right eye, and told her to seek a second opinion.
A 79-year-old white female was referred for evaluation of a lesion in her right eye. The patient noted blurred vision in both eyes, which her primary-care doctor attributed to cataracts. However, her doctor discovered a suspicious yellow lesion in her right eye, and told her to seek a second opinion.
Her medical history is significant for hypertension and headaches, for which she takes several different medications. The patient said she could not remember the names of the medications.
On examination, her best-corrected visual acuity measured 20/20 O.U. Confrontation visual fields were full to careful finger counting. Her pupils were equally round and reactive, with no afferent pupillary defect. Extraocular motility testing was normal. Anterior segment examination demonstrated early, non-visually significant nuclear sclerotic cataracts. Her intraocular pressure measured 17mm Hg O.U.
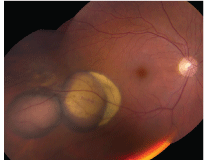
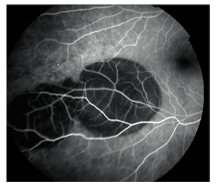
1,2. Note the lobulated lesion along the inferotemporal arcade O.D. (left). What does this represent? Right, a fluorescein angiogram of the lesion at 26 seconds.
Dilated fundus exam showed small cups in both eyes with good rim coloration and perfusion. We observed an elevated lesion located inferotemporally in her right eye (figure 1). Otherwise, both retinas were normal. We also performed a fluorescein angiogram in the right eye (figure 2).
Take the Retina Quiz
1. What does the elevated lesion represent?
a. Choroidal mass.
b. Vitelliform lesion.
c. Hemorrhagic detachment of the retinal pigment epithelium (RPE).
d. Serous retinal detachment.
2. How do you explain the yellow color of the lesion?
a. Exudate.
b. Pus.
c. Lipofuscin.
d. Dehemoglobinized blood.
3. What is the correct diagnosis?
a. Choroidal melanoma.
b. Choroidal hemangioma.
c. Extramacular disciform process.
d. Pattern dystrophy of the RPE.
4. How should this patient be managed?
a. Observation.
b. Plaque radiotherapy.
c. Enucleation.
d. Laser photocoagulation.
For answers, see below.
Discussion
The multi-lobulated elevated lesion along the inferotemporal arcade of the right eye represents hemorrhagic detachments of the RPE. Perhaps, the most important question: If it is a hemorrhagic detachment of the RPE, why is it yellow in appearance and not red? The answer: The lesion appears yellow because it has been present for a long time. We are not exactly certain how long the lesion has existed, but we do know that over time, trapped blood loses hemoglobin and takes on a yellow/white color. We call this appearance dehemoglobinized blood.
We also frequently see dehemoglobinized blood in patients who have experienced a vitreous hemorrhage. The hemorrhage initially appears red, but because the blood is slowly reabsorbed, it changes color and becomes dehemoglobinized. This can be confusing because we are not accustomed to seeing yellow/white hemorrhages.
The fluorescein angiogram of our patient confirms the presence of a hemorrhagic process, not a choroidal mass. The angiogram shows retinal circulation nicely; but below that, we see complete blockage of the choroidal detail due to the hemorrhage. If the lesion were a choroidal mass, we would see the intrinsic vascularity within the mass, not the blockage. Although fluorescein angiography does not completely rule out the presence of a choroidal mass, it greatly helps us make a correct diagnosis.
Standardized ultrasound may be the most helpful test in distinguishing a choroidal mass from another finding. We performed contact B-scan and diagnostic A-scan ultrasonography that showed a lobulated solid lesion measuring 2.2mm in elevation, with dimensions of 6.0mm by 10.0mm. It also showed low reflectivity, with an irregular internal structure and no vascular pulsations. The lesion was too small to differentiate it any further.
The biggest concern was that this finding could be some kind of a mass, such as a choroidal melanoma or a choroidal hemangioma. However, its clinical appearance is not consistent with either condition. Although choroidal melanomas can have low reflectivity on standardized ultrasound, they typically do not develop hemorrhagic detachments of the RPE. Rarely, they can lead to a vitreous hemorrhage as the tumor breaks through Bruchs membrane and tears the overlying retinal vessels.1
Additionally, choroidal hemangiomas typically have high internal reflectivity, which is inconsistent with the ultrasound results for our patient. Finally, adjacent to the elevated mass, lipid exudate can be seen diffusing out from the RPE detachment; exudate is not typically seen in a choroidal melanoma.
So, how do we use all this information to determine what is wrong with our patient? Based on the ancillary testing and clinical picture, the lesion likely represents an extramacular disciform processa choroidal neovascular membrane located outside the macular region, often in the peripheral retina.
Clinically, an extramacular disciform process resembles a yellow or red lesion in the peripheral fundus. It can be slightly elevated or flat. Also, it tends to be very hemorrhagic in nature, unlike what is seen in a choroidal melanoma.
Extramacular disciform lesions have the same pathophysiology as macular choroidal neovascularization associated with age-related macular degeneration, except disciform lesions are located away from the macula. Not surprising, the most common misdiagnosis for extramacular disciform lesion is choroidal melanoma. In one series, extramacular disciform lesions accounted for as many as 11% of all lesions simulating choroidal melanomas.2 In another series, 50% of patients with extramacular disciform lesions were referred with a diagnosis of choroidal melanoma.3
The prognosis for extramacular disciform lesions is generally very good. Because of their eccentric location, they are not usually a threat to visual function unless they bleed into the vitreous. As a result, these lesions can often be observed without treatment.
For more hemorrhagic lesions, off-label treatment with intravitreal Avastin (bevacizumab, Genentech) may eliminate the angiogenic factor that stimulates growth of the lesion and decrease capillary permeability. Often, these lesions will spontaneously involute and develop a disciform scar. The fact that these lesions grow smaller over time is extremely important in differentiating them from other similar-looking lesions, such as choroidal melanoma, which are more likely to increase in size.
We elected to closely observe our patient, and the lesion began to slowly involute during the next year. However, at a follow-up visit approximately 12 months after her first visit, we saw a large area of subretinal hemorrhage, indicating reactivation of choroidal neovascular membrane. We ordered an intravitreal injection of Avastin and the lesion rapidly involuted without any further complications.
1. Char DH. Choroidal simulating lesions. In: Char DH, ed. American Cancer Society Atlas of Clinical Oncology: Tumors of the Eye and Ocular Adnexa.
2. Shields JA, Augsburger JJ, Brown CG, Stephens RF. The differential diagnosis of posterior uveal melanoma. Ophthalmology 1980 Jun;87(6):518-22.
3. Bardenstein DS, Char DH, Irvine RA, Stone, RD. Extramacular disciform lesions simulating uveal tumors. Ophthalmology 1992 Jun;99(6):944-51.
Retina Quiz Answers: 1) c; 2) d; 3) c; 4) a.

