 |
Race may impact a patient's vision-specific quality of life. Photo: Danica Marrelli, OD. Click image to enlarge. |
Preserving vision-specific quality of life (VSQOL) is a priority when caring for patients with eye disease, conducting public health prevention programs and designing clinical trials for ophthalmic interventions, and preventing visual field loss (VFL) may protect patients’ ability to complete visual tasks and their socioemotional well-being. To assess the impact of VFL on VSQOL by race, ethnicity and age, researchers recently studied cross-sectional data from three population-based, prospective cohort studies.
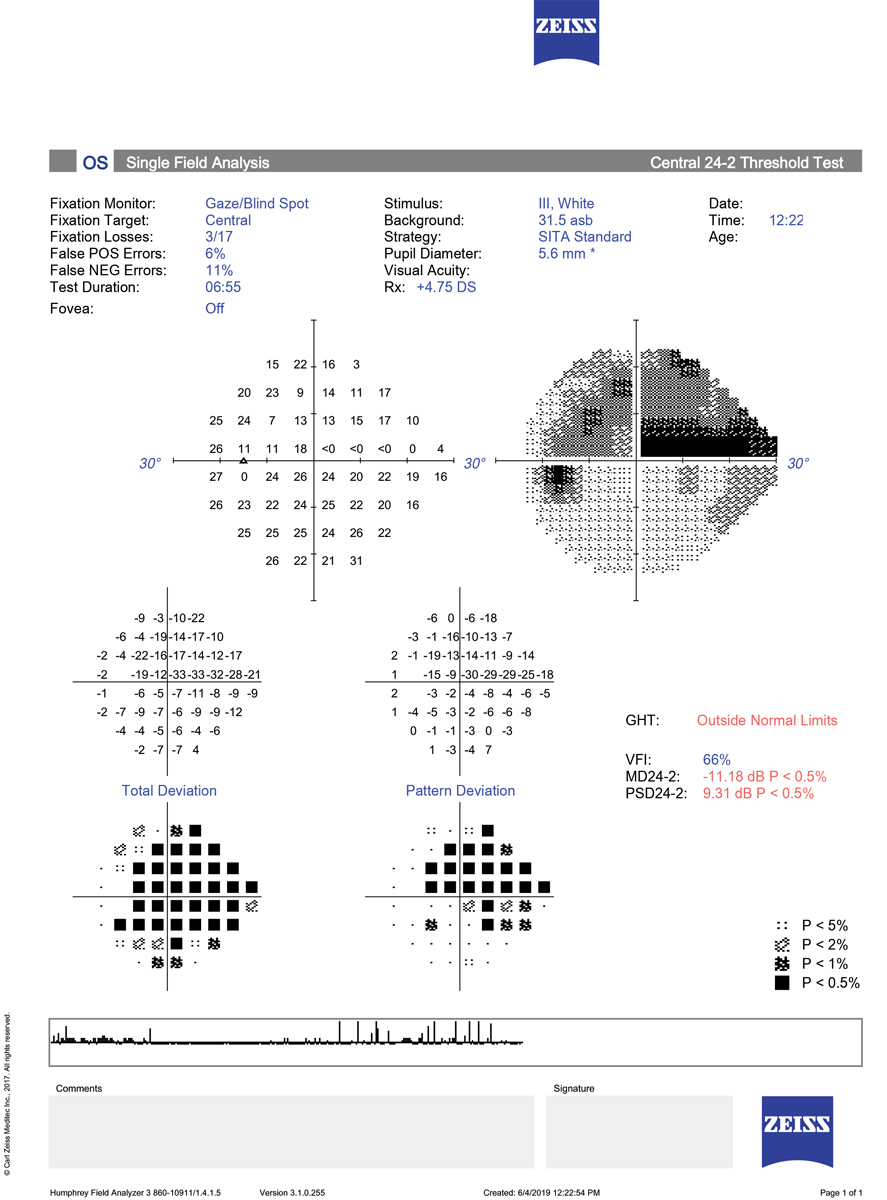
Over 17,000 participants in the Multiethnic Ophthalmology Cohorts of California Study included Americans of Latino, Chinese and African ancestry aged 40 years and older who completed comprehensive interviews and ophthalmic examinations from 2000 to 2018. VFL was measured using the Humphrey SITA Standard 24-2 test, multivariable linear regression was used to evaluate the impact of VFL in the better-seeing eye on self-reported VSQOL scores, adjusting for sociodemographic and clinical covariables, and hierarchical modeling was performed to determine the best-fit model after considering main effects and interactions by race, ethnicity and age.
The analysis found that race and ethnicity are important modifiers of the relationship between VFL and VSQOL even after adjusting for sociodemographic factors—education, employment and income. Latinos and Chinese Americans reported a greater change in VSQOL than African Americans for the same level of VFL.
Sensitivity analyses were conducted to further address whether the interaction by race and ethnicity in the association of VSQOL and VFL could be explained by measured sociodemographics.
“Racial and ethnic differences were diminished when restricting models to participants aged 65 years and older, suggesting that underlying differences associated with race and ethnicity have less influence on older populations with worse VFL,” the authors explained. “A survivor bias may contribute to older participants from all races and ethnicities having similar VSQOL responses to VFL. However, most differences persisted when restricting by sex, socioeconomic status factors, immigration status, depression and central visual impairment, suggesting that race and ethnicity have an enduring differential effect on the associations between VFL and VSQOL among specific subgroups.”
VFL had the largest effect on driving among all participants. Driving difficulty was the only VSQOL outcome modified by age; participants 65 years and older scored lower points.
VFL’s second largest effect was on vision-related role function, which indicates how vision inhibits participants from accomplishing as much as they would like and from working for longer periods of time, the authors explained. “Latinos and Chinese Americans reported significantly lower role function scores with VFL as well as lower educational attainment, annual income and health insurance,” they noted. “These cohorts were also predominantly immigrant populations compared with the African American cohort. Differences in how VFL affects the ability to complete visual tasks is likely due to differences in sociodemographics that persist even when adjusting for socioeconomic status and immigration.”
The authors suggested future clinical trials “include multiethnic samples to ensure findings apply to the increasingly diverse US population with respect to race, ethnicity, age and socioeconomic factors.”
Grisafe DJ, McKean-Cowdin R, Burkemper BS, et al. Visual field loss impacts vision-specific of life by race, ethnicity: the multiethnic ophthalmology cohorts of California study. Ophthalmology. December 30, 2021. [Epub ahead of print]. |

