An optometrist refers a cataract patient for surgery, and the ophthalmologist sits down with the patient and informs him that he could benefit from a premium intraocular lens (IOL) that will correct for the effects of presbyopia. Confused, the patient asks, “What is presbyopia, and what’s an IOL?” and, “Why didn’t my doctor tell me about this?”
Result: the patient leaves the office overwhelmed by the barrage of new information because they weren’t informed of the options sooner. It’s better all around if the patient had the chance to at least learn the basics from their optometrist.
“An example is a toric IOL,” says Paul M. Karpecki, OD, of Koffler Vision Group in Lexington, Ky. “Often, patients have better results from these lenses than any other options available, but may not pursue this option if they’ve not heard about it previously.”
Paul Ajamian, OD, who runs the Omni Eye Services comanagement center in Atlanta, has heard this scenario before. He says patients want to hear their IOL options first from their family doctor of optometry. ODs know their patients best because patients have gone to them the longest; in many cases, the relationship spans decades. Bottom line: Patients value your expertise and the connection you share with them.
“We’re looking for patients who have come to us after their optometrist has already talked to them about their refractive options,” says Dr. Ajamian. “Most surgeons worth their salt welcome that information from the OD because the OD knows the refractive and vision history, and lifestyle demands of patients, better than the ophthalmologist.”
But while there is nothing wrong with suggesting a specific lens if you have a good comanagement relationship with your surgeon, leave yourself some wiggle room; the surgeon might not use it or the patient may not be a good candidate. “Treat cataract surgery like retina surgery,” one ophthalmologist advises. “As a cataract surgeon, I would tell my patient with a retinal detachment to discuss the options with the retina surgeon, and I would refrain from giving retina guidance.” In other words: educate, don’t advocate.
While so-called premium IOLs (i.e., multifocals, torics, accommodating lenses) have been around for almost a decade, newer iterations perform better than their predecessors. The designs are more complex than monofocal IOLs, the patient selection criteria more stringent and patients need considerable prep to make an informed decision when they go in for surgery.
That’s where you come in.
Lens Discussion
There are many lenses on the market and ultimately choosing the right one is the responsibility of the comanaging OD and surgeon. Here’s how to help patients get acquainted with the newest IOL concepts and options.
• Torics. Toric IOLs are for astigmatic patients that need correction for 1.00D or above. Jonathan Stein, MD, an instructor at the NYU department of ophthalmology, suggests explaining to patients that toric lenses correct for distance, but not intermediate or near vision. Eric Donnenfeld, MD, Clinical Professor of Ophthalmology at NYU Medical Center, cautions against implanting them in patients with irregular corneas, such as keratoconus. Torics now come in cylinder options from +6.00D to +34.00D. The AcrySof IQ Restor IOL +3D (Alcon) and the Tecnis Toric Aspheric IOL (Abbott Medical Optics) both benefit from this wider range of potential correction, Dr. Donnenfeld says.
A sample conversation with the patient might begin like this: “The shape of your eye causes some blurriness that conventional IOLs won’t correct. Luckily, you have a lot of options to address it. Glasses or contacts would do a great job, but if you want to avoid that, you might be able to have it corrected surgically. New IOL designs build that correction in. For astigmatism under 1.00D, surgeons with access to a femtosecond cataract laser also can reshape your cornea during cataract surgery too.”
• Multifocals. These IOLs offer patients the greatest range of vision, says Dr. Stein. But they require some visual compromise and neuroadaptation. Early on, most multifocals came with +4D adds. Now, lower-add multifocal IOLs (e.g., add powers of +2.75D to +3.25D) expand the potential range of vision, Dr. Donnenfeld says. And some multifocal IOLs will soon come with a toric correction as well, he says.
Because multifocals split the light rays into two foci as they pass through the lens, the patient’s ocular anatomy needs to be free of any conditions that might reduce vision. Dr. Donnenfeld says patients should have good retinal and ocular surface function and tear film quality to be suitable candidates for multifocal IOL implantation. Patients with previous corneal surgery such as LASIK, or those with a history of epithelial basement membrane dystrophy, don’t do well with multifocals. Other comorbidities include glaucoma, macular degeneration, epiretinal membrane or diabetic retinopathy.
 | |
|
The lens used in this piggyback fit is well centered and showed adequate movement.
|
A sample patient conversation: “You’ve probably been wearing reading glasses since your 40s or 50s. If you’re happy with that, you can stay with them after the surgery. But some new IOL options could allow for less dependence on those readers—and maybe even eliminate them completely.” Be sure to fully educate about the potential for glare and halos in some patients during the adaptation period.
• Accommodating lenses. These IOLs avoid the trade-offs inherent in multifocality by flexing in a way analogous to the natural human lens, but offer a more limited range of correction. Two FDA-approved lenses, the Crystalens and its toric version, the Trulign Toric—both from Bausch + Lomb—correct for intermediate and distance vision but not near, says Dr. Stein. Patients do well with accommodating lenses, but will have more difficulty reading up close.
“Because they have very flexible haptics,” says Dr. Donnenfeld, accommodating lenses “are less predictable at achieving emmetropia and may require excimer laser enhancements more frequently to achieve optimal distance than a conventional IOL.”
You might follow the discussion of multifocals by segueing into a discussion of accommodating lenses. You could say, “The surgeon will want you to think about how much up close vision you need vs. intermediate vision. Think of it as cell phone vs. laptop. Which do you use more?” As always, stress that the surgeon will need to consider a variety of anatomical and visual factors when making the final call.
|
Comanagement Dos and Don'ts
• DO let the ophthalmologist know the type of lens(es) you discussed with the patient and document that in the patient’s medical records. The patient needs a basic understanding of what lenses or procedures they are candidates for before seeing the surgeon, according to Dr. Ajamian. • DON’T recommend presbyopic lenses for patients with macular degeneration, significant glaucoma or other ocular health issues, or who’ve had LASIK. Dr. Karpecki cautions that these patients have corneal wavefront aberrations already, and are best treated with monofocal lenses. • DON’T refer patients with advanced Fuchs’ dystrophy (indicated by morning blur lasting more than two hours; a failed cornea in the other eye after cataract surgery; pachs greater than 600µm to 640µm, depending on baseline; or specular microscopy less than 800µm) for cataract surgery. The patient must be corrected with DSEK and then undergo cataract surgery at a later date, according to Dr. Karpecki. • DO inform the surgeon of topography/keratometry readings for the degree of astigmatism. These measurements determine whether the patient may benefit from a toric IOL, according to Dr. Mann. And be sure to explain to patients what astigmatism is—many don’t know. • DO tell patients not to wear contact lenses for at least two weeks before undergoing their preoperative evaluation so the results of keratometry measurements and ocular surface readings won’t be skewed, says Dr. Mann. • DO bring up patient history to the surgeon. For example, a history of trauma means the zonules may have weakened, Dr. Karpecki says. Another example: the patient is on Flomax for benign prostate hypertrophy (BPH), which may cause floppy iris syndrome in some patients for whom the surgeon must choose the IOL carefully, he says. • DON’T refer patients for IOL surgery who have poor ocular surface health secondary to dry eye or meibomian gland dysfunction, says Dr. Karpecki. Treat the ocular surface disease first. “If a patient comes into my office and I measure osmolarity and it’s 330 or I see central corneal staining, I have to tell patients they’re not the right a candidate yet for surgery because we may not get the right calculations,” he adds. • DO inform patients you’ll be seeing them after surgery for postoperative care, says Dr. Whitley. Make sure they know you’ll share their care with surgeons. “We’re a surgical practice and we do everything to keep the referromg OD involved,” he says. “Tell patients you typically share in the care of postoperative examinations.” The decision on whether to be comanaged is up to the patient. However, it’s best to educate patients on your role in the perioperative process. |
The Right Attitude
You play a key role in explaining IOL choices to patients before they reach the ophthalmologist’s office, but the patient conversation can be daunting with so much ground to cover. You don’t want to spend 30 minutes discussing complex IOL designs, but you do want to introduce them.
Focus on outcomes, not technical specs, says Kevin Waltz, OD, MD, founder of Eye Surgeons of Indiana in Indianapolis. Resist the temptation to color a conversation with reports of bad experiences based on only a few cases, or with earlier generation lenses. The conversation needs the right balance—neither hype nor negativity about a particular lens, to help patients decide what’s best for them. “You want to undersell and overdeliver,” says Dr. Ajamian.
So, what’s the best way to talk about IOLs?
1. Know your surgeons. Stay current about the capabilities and outcomes of the surgical practices you refer to so that you’ll be able to tell the patient what to expect in a concrete way, says Dr. Ajamian. Find out what the surgeons’ IOL and surgical preferences are. “Spend some time with surgeons doing rounds at their office or going into surgery with them,” says Dr. Ajamian. “It gives you a good feel for what your patients will experience.”
2. Introduce them to your preferred surgeon, suggests Walter Whitley, OD, Director of Optometric Services at Virginia Eye Consultants, a tertiary referral center in Norfolk, Va. Explain why you choose to work with that particular surgeon, the IOL options your surgeon implants and any relevant details about their surgical approach, especially if they incorporate the femtosecond laser into the procedure.
3. Obtain educational tools from the surgeon for the patient to read or create your own, adds Dr. Whitley. If you have an ongoing referral relationship with a surgical practice, sync up your educational efforts with theirs. That could include profiles of the surgeon’s outcomes, the various advanced technology IOLs available and any innovative technologies or lenses they use, and what to expect in the post-op period. When the patient does their homework, they’ll make a better decision.

|
|
|
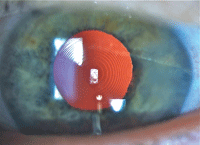
A toric IOL, situated in the eye.
|
Matching Patient Personalities with IOL Options
Making IOL recommendations requires understanding patients’ personalities. The key: Never guarantee anything, says Dr. Ajamian. Instead, find out each patient’s goals and expectations. Here are some common patient personality types and how best to approach them:
1. Perfectionists. Patients expect perfect vision after IOL surgery. But never promise complete independence from glasses. Patients may still not be able to read up close and could experience halos and glare at nighttime, according to Dr. Karpecki. Or they may need glasses for protection against macular degeneration after surgery. Patients with astigmatism can expect to have clear vision without glasses, but may still need reading glasses. Those who like to read can benefit from multifocals, and will have clear distance vision, but need reading glasses for small print, says Dr. Karpecki. Ask the patient two questions: “Is it important for you to have clear vision? Is a low risk of halos or glare OK?”
2. Hard-to-please patients. “If you have a patient who’s very particular—who is very difficult to please with spectacles-—I’d be cautious about recommending a multifocal in this patient,” says Daryl Mann, OD, chief manager of South East Eye Specialists in Chattanooga, Tenn. If the patient had multifocal glasses or contact lenses in the past, they may be a good candidate for a multifocal IOL, especially if they don’t like the thought of reading glasses.
3. Creatures of habit. Patients accustomed to wearing glasses or contacts to perform certain tasks would not be good candidates for certain types of lenses, according to Dr. Waltz.
If a patient is used to monovision contact lenses before cataract surgery, chances are they’ll want to continue that after cataract surgery, according to Dr. Ajamian.
If the patient is used to taking their glasses off to read, they’ll balk at a multifocal or accommodating IOL, says Dr. Waltz. He puts them in a special file because they have specific needs. He typically leaves the patient plano for distance and nearsighted to allow to stay as they were.
“They’re telling you they’re a creature of habit, and my habit is to take off my glasses and I don’t mind doing that,” says Dr. Waltz. “So if you make me change my habits, I’m not a very happy creature.”
|
A new category of presbyopia-correcting IOLs undergoing FDA trials would allow added near vision with fewer halos and less glare, says Dr. Stein. These are called extended depth-of-focus IOLs; investigational designs include the Symfony IOL (Abbott) and Adaptis shape-changing lenses (Hoya). The Calhoun Light Adjustable Lens—also advancing in FDA trials—allows the surgeon to implant the lens and return to the patient later to adjust for power, cylinder and higher-order aberrations, says Dr. Stein. Elenza, a new player in this market, is developing the Sapphire Autofocal, an IOL that lets the surgeon adjust for near, intermediate and distance vision with an “electro-active switchable element,” according to its website, www.elenza.com. |
Breaking the News About Out-of-Pocket Costs
The out-of-pocket costs to patients for these lenses can be steep. While that discussion is best left to the surgical practice, you should at least explain the concept of patient-shared billing so they know they’ll be expected to cover what insurance does not.
1. Put a positive spin on it. It’s going to allow them to see better for the rest of their lives, says Dr. Ajamian. For example, you could say, “If this is something you want, it’s worth finding a way to pay for it.”
2. Finance it. Recommend financing companies such as Care Credit. “It’s like leasing a car,” says Dr. Ajamian. If you can’t pay cash for the car, you take out a loan or lease it; and isn’t your vision more important than a car?”
3. Be transparent. Always tell patients there are additional costs for premium IOLs that health insurance does not cover, according to Dr. Ajamian. Have an idea of the exact costs, copays and facility fees of the surgeon. Your office staff can go over an itemized list of the additional costs if your patient is interested in a particular lens.

