 History
History
A 74-year-old white male presented for an annual ocular health examination. It was his first visit to our office, and his chief complaint was foreign-body sensation and tearing in both eyes. He had been using artificial tears b.i.d. O.U.
He did not report any other pertinent ocular history. His systemic history included hypertension and hypercholesterolemia, which was medically controlled with Vasotec (enalapril maleate, Merck) and Lipitor (atorvastatin calcium, Pfizer). The patient had no known drug allergies.
Diagnostic Data
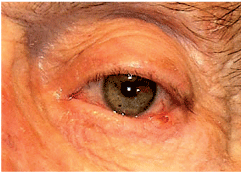
This 74-year-old male complained of foreign-body sensation and tearing in both eyes.
His best-corrected visual acuity was 20/25 O.U. at distance and near. The pertinent external examination findings involved the left lower lid, as demonstrated in the photograph. Also, we noted bilateral blepharitis.
The anterior segment examination revealed an iris nevus O.S., which the patient claimed had been present for several years. Additionally, we identified grade 1 nuclear sclerosis O.U. His intraocular pressure measured 18mm Hg O.U. The posterior segment findings were unremarkable in both eyes.
Your Diagnosis
How would you approach this case? Does this patient require any additional tests? What is your diagnosis? How would you manage this patient? Whats the likely prognosis?
Thanks to Marc Myers, O.D., of
Discussion
The diagnosis in this case is basal cell carcinoma (BCC). The lid lesion did not have an aggressive growth pattern, but did cause irritation and lash loss along the lid margin (maderosis).
When a suspicious lesion is seen involving the adnexa of the eye, such as a recurrent growth or a growth associated with maderosis, malignancy must be ruled out. Take the time to explain to the patient the differential diagnoses, available treatment options and potential outcomes. Also, recommend sun protection strategies.1-3
The most common primary skin malignancy is BCC. Less common malignancies include squamous cell carcinoma, sebaceous cell carcinoma, malignant melanoma and Kaposis sarcoma. Benign lesions that may present with a similar appearance include ulcerative blepharitis, chalazion, external hordeolum, keratoacanthoma, actinic keratitis and Bowens disease (multiple squamous cell carcinoma with bone and dental deformities).2
Our patient was seen by an oculoplastic surgeon, who agreed that the leading differential diagnosis was BCC. Treatment included surgical removal via a pentagonal incision involving the lower lid margin. Histologic testing confirmed our diagnosis of BCC. The surgeon also made a distinct point to review sun safety instructions with the patient.1-3
1. Leiter U, Garbe C. Epidemiology of melanoma and nonmelanoma skin cancer--the role of sunlight. Adv Exp Med Biol 2008;624(1):89-103.
2. Shields J, Shields C. Tumors and pseudotumors of the eyelids. In: Mannis M, Macsai M, Huntley A. Atlas of Eyelid and Conjunctival Tumors:
3. Bruce A, Brodland D. Overview of skin cancer detection and prevention from the primary care physician. Mayo Clin Proc 2000 May;75(5):491-500.

