 |
When I started out as a fresh new OD, I thought ‘primary eye’ care meant doing the basics of vision care—refractions, spectacles, contact lenses and regular eye exams. Boy, was I wrong. It didn’t take me long to realize it means managing everything related to the eyes and vision that isn’t secondary care (e.g., a subspecialist) or tertiary (e.g., transplants, oncology). That’s a lot to be in charge of, as it includes everything from eye alignment to neurology to the diagnosis of rare diseases and malignant tumors. These days, primary care ODs even realize that electrodiagnostics and other advanced tools are essential to providing these key services. Here’s a look at some of the new technologies gracing a primary eye care office:
SightSync. This can detect and measure eye alignment in less than two minutes. The technology uses peripheral focus, and is objective and accurate for measuring horizontal phorias. It is also designed to transfer measurements into a spectacle lens called a neurolens, essentially a progressive prism created to correct the problem. In its pivotal study, 93% of patients had a reduction in symptoms and 74% stated the symptoms were eliminated or decreased substantially.1
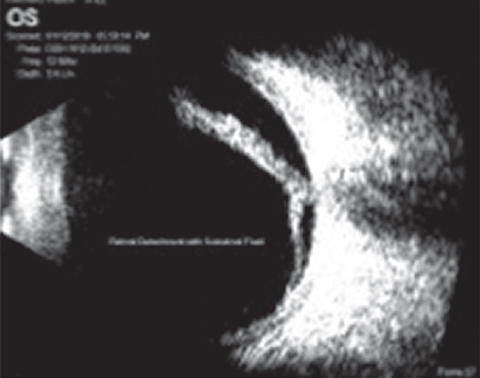 |
| This B-scan, taken with the Scanmate Flex, reveals a retinal detachment. |
Ultrasound. More than a decade ago when an A-scan/B-scan/ultrasound biomicroscope combination cost six figures, it didn’t seem to fit with primary eye care. Today, because of advances in technology, more ODs are adding this, gaining high resolution imaging for a tenth of the cost. Now it fits squarely into primary eye care and may become an essential piece of equipment necessary to practice at a high level.
Take, for example, something we see often: a choroidal nevus. How do you determine if it truly is just a nevus rather than a malignant melanoma? Two important determinants are the basal diameter and the elevation, both of which can be determined easily and accurately with B-scan ultrasound. A basal diameter that increases over time or an elevation over 2mm are significant signs of a potential melanoma (other signs include lipofuscin on the surface of the lesion, touching the optic nerve or the presence of subretinal fluid).
Ultrasound can help you confirm a retinal detachment, visualize the retina when there is no clear view (e.g., vitreous heme), assess axial length for cataract surgery, determine angle closure and narrow angles and detect iris cysts and tumors, to name a few. In my practice, we routinely have every patient diagnosed with a moderate or large nevi undergo ultrasound measurements and monitor for progression.
VEP/ERG. Visual evoked potential measures the signal passing through the optic nerve to the brain—an ideal tool when determining neuropathy. Another electrodiagnostic test, electroretinogram, can also help assess retinal function. Both technologies are now available in smaller, portable options, and are far easier to use than previous iterations. They can be integral to detecting and following glaucoma, early retinitis pigmentosa and diabetic retinopathy, for ex-ample, without the need for dilation.
Pupil testing. The days of the difficult swinging flashlight test may finally be behind us. Doctors and staff have always had difficulty with this, given that some patients have dark irides or the relative afferent pupil defect (RAPD) was small. A new device called EyeKinetix (Konan Medical) takes about 30 seconds and can determine the presence of a 0.5 RAPD, helping with an overall neuro assessment screening for the potential diagnosis of glaucoma (often being an asymmetric neuropathy).
Given these impressive technological advances, it may be time to consider advanced testing as truly primary eye care tests.
Note: Dr. Karpecki is a consultant for many companies mentioned here.
| 1. Miles C, Krall J, Thompson V, Colvard DM. A new treatment for refractory chronic daily headache. eyeBrain pivotal trial. January 2016. |

