First recognized nearly 50 years ago, obstructive sleep apnea has become an increasingly common condition in the United States.1 The reported incidence rate varies substantially—with a high of 9% in the female Caucasian population and 24% in the male Caucasian population.2 More than 80% of patients with OSA are believed to be undiagnosed, and many more are diagnosed but go untreated for a variety of reasons; just 10% of all OSA sufferers receive treatment.3
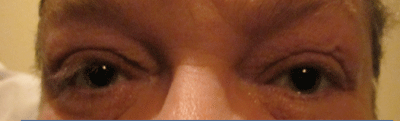
1. Floppy eyelid syndrome in a patient with obstructive sleep apnea.
What does this potentially deadly sleep disorder have to do with eye care? Well, the increasing prevalence of this condition in the US means you will more than likely see many patients with diagnosed, undiagnosed and/or untreated OSA in your office. And untreated sleep apnea leads to a host of systemic and ocular complications, so proper diagnosis and management are critical to the patient’s overall health.
While it is possible that you could play a role in spotting the condition, it is certain that you will have to deal with some of the complications that accompany the disease.
In this article, we’ll look at what OSA is and which patients may be at higher risk, as well as common systemic and ophthalmic conditions associated with sleep apnea.
What’s the Problem?
In patients with sleep apnea, the tissue of the soft palate collapses during sleep, partially occluding the airway. This obstruction leads to lapses in breathing and decreased oxygen saturation in the blood, which the brain senses. The body feels as if it needs to take a breath, so the patient gasps in an attempt to draw in more oxygen. Substantial snoring is almost universally present, and snoring that stops during prolonged periods of apnea (a Greek word meaning without breath) is a particularly distinctive symptom of OSA.
While most of the conditions we’ve discussed are associated with
sleep apnea itself, some complications can be encountered in the
treatment for this condition. For example, use of CPAP therapy can be
associated with ocular complications. Air can leak from around the edge
of the mask and be directed toward the eyes, leading to dryness and
irritation. Exposure of the eye to this air that has passed over the
mouth and nose also results in a higher rate of bacterial
conjunctivitis.34
The typical OSA patient tends to possess a distinguishing set of traits, sometimes referred to as “Pickwick syndrome”—after an overweight, chronically sleepy character in the Charles Dickens novel, The Pickwick Papers.1,4 Sleep apnea is highly associated with the obesity epidemic facing our nation—as many, but certainly not all, OSA sufferers are also obese.
Ophthalmic Complications Associated with CPAP Devices
The majority of patients with OSA are overweight individuals with a large neck circumference (usually greater than 17 inches). In addition, this condition afflicts males twice as often as females. African Americans are 2.5 times more likely to present with OSA than Caucasians.5 In general, the risk significantly increases with age and is higher in smokers.
Sufferers are often sleepy and tired during the day, and report feeling as if they did not sleep even when they have gotten the seven to nine hours of rest recommended for adults. What these patients don’t realize is that their sleep is often fragmented—disrupted each time the patient experiences an apneic event. Most OSA patients do not completely wake up during their nighttime episodes, so they are often unaware of what they are experiencing. Other individuals who sleep in the same room or share a home with these sufferers are more likely to be able to report the symptoms the patient is experiencing (e.g., snoring, waking up in the middle of the night and gasping for air).
Diagnostic Screening/Testing
Suspicion of OSA typically arises when patients experience the signs and symptoms previously discussed. Many different methods are used to make a formal diagnosis:
• Epworth Sleepiness Scale. This simple questionnaire is a very useful and cost-effective screening device. The patient self-reports the likelihood of dozing or falling asleep during various activities, such as reading, watching TV, riding in a car, etc. Each activity is assessed on a scale that ranges from never sleeping or dozing during the activity to having a high chance of doing so. An overall score is then tabulated and compared to a risk table.
• At-home sleep testing. At-home diagnostic testing for sleep disorders has become much more common in the past few years as more devices have become FDA approved and eligible for reimbursement. However, not all patients are good candidates for this type of testing and few insurance carriers cover it.
• Polysomnography. Polysomnography testing conducted in a sleep laboratory remains the gold standard in diagnosing OSA.6 The patient will need to stay overnight in a sleep laboratory and will be hooked up to sensors that measure various parameters regarding their sleep and oxygen levels. One of the most useful diagnostic measures obtained during polysomnography is the apnea-hypopnea index, or AHI. This index scores the number of disordered breathing events per hour and then assigns a ranking that ranges from not clinically significant to severe OSA.
Common Treatment Options
The diagnosis of OSA is merely the beginning of the management challenge faced by health care providers and their patients. The most common intervention, use of a continuous positive airway pressure (CPAP) device, has a variable compliance rate due to a variety of factors.7 With CPAP therapy, the patient is fit with a mask that is connected to a machine creating a continuous flow of air. This continuous airflow forces the airway to remain open by preventing the soft palate from collapsing.
While CPAP devices can be very effective, they often require a great deal of fine-tuning to find a comfortable fit with the mask and the airflow pressure. In combination with a number of factors—such as uncomfortable mask wear, machine noise, nasal congestion, irritation of nose and throat—this adjustment process often leads to frustration and poor adherence to therapy.7
Some patients cannot exhale effectively against the pressurized airflow created by their CPAP device and must turn to the use of bilevel positive airway pressure (BiPAP) systems.8 These systems have a different setting for the airflow pressure during inhalation and exhalation.
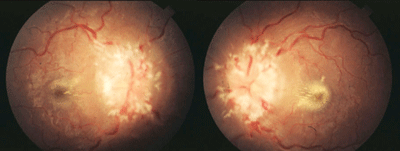
2. Papilledema is fairly common in individuals with OSA.
Fortunately, there are other therapeutic options available for OSA sufferers who need them. These include dental devices that thrust the lower jaw forward, and various surgical procedures designed to strengthen the soft palate or reduce the volume of the tongue.
In addition, patients may alleviate symptoms by making lifestyle modifications, such as losing weight, increasing physical activity, avoiding sleeping pills and alcohol before bed, and changing body positions during sleep.6
Systemic Conditions Associated with OSA
Because OSA leads to poor oxygen delivery to tissue and organs throughout the body, it is associated with a wide array of systemic conditions.
These include many common cardiovascular, endocrine and ischemic vascular diseases, such as heart disease, hypertension, stroke and diabetes.9 Some estimates suggest alarmingly high rates of OSA in common disease populations:5
- 50% of heart disease patients
- 60% of stroke patients
- 80% of patients with difficult to control hypertension
- 70% of obese individuals (often leading to type 2 diabetes)
With undetected and/or untreated sleep apnea, properly managing these comorbidities can be challenging to say the least.
OSA and the Eye
Failure to identify and manage underlying sleep apnea can also make it very difficult to appropriately manage secondary ocular concerns. A number of anterior and posterior eye conditions are associated with OSA, including floppy eyelid syndrome (FES), optic neuropathy, glaucoma, non-arteritic anterior ischemic optic neuropathy (NAION) and papilledema (disc edema secondary to raised intracranial pressure).10 Let’s take a look at how these conditions may present in the sleep apnea patient, as well as helpful treatment interventions.
Floppy Eyelid Syndrome
OSA is highly associated with both keratoconus and FES.10 While the direct link between these conditions and OSA remains elusive, the etiology may hinge upon increased matrix metalloproteinase.11 The decreased oxygen supply with OSA can lead to an increased production of matrix metalloproteinase, which, in turn, tends to decrease tissue elasticity.11,12 This is especially important in cases of FES.
While less than 5% of OSA patients develop FES, nearly 100% of individuals with FES suffer from OSA.13 Therefore, it is imperative that all patients with FES be evaluated for OSA if they have not already been diagnosed, especially if they report any of the commonly experienced signs or symptoms. Patients with FES have extremely loose, rubbery eyelids, which evert very easily upon contact with the pillow during sleep (figure 1). This leads to exposure keratitis and dryness, as well as mechanical keratoconjunctivitis, as a result of direct contact with surfaces. Patients experience irritation and dryness that is at its worst upon awakening but improves as the day goes on.
Another common finding with FES is lash ptosis, where the upper eyelashes point downward as the result of chronic lid eversion at night. Unfortunately, FES is underappreciated and often goes undetected, which leads to frustration in patients who cannot get relief from their symptoms. Because similar symptoms are also seen with dry eye syndrome and blepharitis, patients are commonly diagnosed with—and treated for—those conditions with limited success.
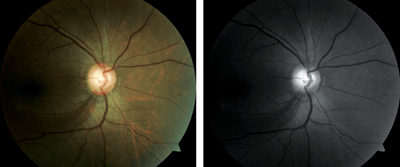
3. Normal-tension glaucoma with a retinal nerve fiber layer wedge defect in a patient with sleep apnea.
Appropriate management of FES is multi-modal. Patient education is critical, as is appropriate management of the underlying OSA. Nighttime lubricating ointments are applied to protect the ocular surface from both exposure and mechanical abrasion. A stiff sleep mask can be used to help keep the lids from everting when the face contacts the pillow. Wearing a sleep mask, however, can be difficult for patients who are already wearing a CPAP mask.
Also consider the benefits of a cylindrical or “dog bone” pillow—the design allows the patient to rest their cheek on the pillow without direct eyelid contact. The lids can be taped closed each evening to prevent eversion, but anecdotally, patients often do not comply with this recommendation long term due to inconvenience, discomfort or skin irritation from the tape. Some practitioners have reported success in recommending that their patients secure their lids closed with commercially available strips designed to open the nasal passages. In severe cases, surgical intervention may be warranted—lid tissue can be removed to tighten the lids and help to prevent spontaneous nighttime eversion. Unfortunately, in some patients the improvement is not permanent and the condition returns at some point after surgery.14
Papilledema
Papilledema is not a generic term that can be applied to any type of optic nerve swelling. Rather, papilledema is an optic nerve head swelling, most often bilateral, that is specifically the result of elevated intracranial pressure (figure 2). Optic nerve swelling that arises from any other etiology cannot be accurately referred to in this manner. Elevated intracranial pressure during the overnight hours can be seen in patients suffering from OSA.15 The elevated pressure, in turn, may result in mild to moderate papilledema with headaches experienced upon awakening.10
Most authors postulate that the elevated intracranial pressure overnight is the result of venous dilation caused by hypoxia and hypercapnia from apneic events.10 While the optic nerve swelling is easily visualized, the underlying phenomenon can be particularly challenging to detect because the intracranial pressure often returns to normal during waking hours.16 Therefore, confirmation may only be possible with lumbar taps performed during the middle of the night. Clearly this is a significant practical concern. Thankfully, intracranial pressure may return to normal with appropriate management of the underlying OSA using CPAP therapy.17,18
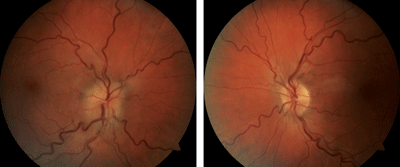
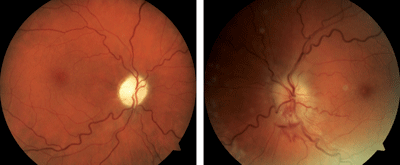
4, 5. Sequential NAION in a patient with sleep apnea. The patient presented with NAION OD (top) and upon work-up was subsequently determined to have OSA. She could not tolerate CPAP therapy, and several weeks later experienced NAION OS (bottom).
Clinicians should be particularly suspicious of OSA in males with papilledema and normal neuroimaging studies. These findings are often indicative of idiopathic intracranial hypertension, also known as pseudotumor cerebri. However, idiopathic intracranial hypertension is encountered far more frequently in females than it is in males, making it very important to consider alternative etiologies of increased intracranial pressure in male patients, especially older male patients.
Glaucoma
Though there are some contradictory studies, primary open-angle glaucoma and normal-tension glaucoma seem to be encountered more frequently in patients with OSA than in the general population.19-21 This is particularly true in the case of normal-tension glaucoma.22
At least one study has shown that the intraocular pressure does not elevate at night in OSA patients, so it is believed that the increased likelihood of developing glaucoma is the result of ischemia from poor oxygen delivery.23
Other reports, however, indicate that patients with OSA may experience significant 24-hour variations in their IOP with elevation possible at night.24 It is important for clinicians to consider OSA in patients with glaucoma, especially those with normal-tension glaucoma that is progressing in spite of optimal IOP control (figure 3). It is also wise to keep in mind the association between CPAP therapy and elevated IOP in some individuals.25
NAION
NAION has proven over time to be very highly associated with OSA, with multiple studies showing a clear correlation between the two processes.26,27 One study examined 27 consecutive patients diagnosed with NAION. Upon testing, the researchers found that 24 of them suffered from OSA.26 Another report revealed that 12 of 17 patients with NAION were diagnosed with sleep apnea after being evaluated, while just three of 17 matched controls were found to suffer from OSA.27 It is not surprising that sleep apnea is encountered with such regularity in patients afflicted with NAION. The damage to the optic nerve is the result of an ischemic event caused by poor perfusion, often in anatomically predisposed optic nerves with little or no cupping (figures 4 and 5).
The majority of NAION patients first notice vision loss upon awakening in the morning.27,28 The decreased nighttime blood oxygen saturation OSA patients experience could contribute to acute ischemic events involving the blood supply of the optic nerve. All patients who are diagnosed with NAION should be questioned regarding a history of OSA, and sleep studies should be strongly considered if no previous diagnosis has been made.
Miscellaneous Retinal Conditions
There are at least three other retinal conditions that are more frequently present in patients with sleep apnea. Multiple reports have found retinal vein occlusions to present more commonly in patients suffering from OSA.29 In addition, diabetic patients with retinopathy are more likely to exhibit proliferative disease and macular edema when they concomitantly have sleep apnea, and those with proliferative disease have a greater chance of developing iris neovascularization.30,31 Recent reports have also linked idiopathic central serous chorioretinopathy to this condition, with treatment of OSA leading to rapid resolution of the chorioretinopathy.32,33
Obstructive sleep apnea has become a substantial health concern in the United States and many other countries. It has a significant, harmful effect on the entire body and the eye, and it is associated with a host of systemic and ocular conditions. Failure to diagnose and manage underlying sleep apnea can make it very difficult to properly control these associated conditions. It is imperative that eye care practitioners be aware of the signs and symptoms of sleep apnea, and of the effect that the disease has on the body and the eye.
Dr. Sutton is a clinical professor at Indiana University School of Optometry and Service Chief of the Indianapolis Eye Care Center in Indianapolis, Ind.
1. Gastaut H, Tassinari CA, Duron B. Polygraphic study of the episodic diurnal and nocturnal (hypnic and respiratory) manifestations of the Pickwick syndrome. Brain Res. 1966 Feb;1(2):167-86.
2. Young T, Palta M, Dempsey J, et al. The occurrence of sleep-disordered breathing among middle-aged adults. N Engl J Med. 1993 Apr 29;328(17):1230-5.
3. Young T, Evans L, Finn L, Palta M. Estimation of the clinically diagnosed proportion of sleep apnea syndrome in middle-aged men and women. Sleep. 1997 Sep;20(9):705-6.
4. Mokhlesi B, Tulaimat A. Recent advances in obesity hypoventilation syndrome. Chest. 2007 Oct;132(4):1322-36.
5. Nabili ST, Marks JW, ed. Sleep apnea. Available at:
http://www.medicinenet.com/sleep_apnea/article.htm. Accessed December 2012.
6. Usmani ZA, Chai-Coetzer CL, Antic NA, McEvoy RD. Obstructive sleep apnoea in adults. Postgrad Med J. 2012 Nov 17. [Epub ahead of print]
7. Selvaraj S, Humphreys J, Wilson J, et al. A retrospective study of factors contributing to the non-adherence and failure of treatment with continuous positive airway pressure (CPAP) in obstructive sleep apnoea (OSA) syndrome patients. Am J Respir Crit Care Med. 2012 May;185(1MeetingAbstracts):A6458.
8. Schafer H, Ewig S, Hasper E, Luderitz B. Failure of CPAP therapy in obstructive sleep apnoea syndrome: predictive factors and treatment with bilevel positive airway pressure. Respir Med. 1998 Feb;92(2):208-15.
9. Caples SM, Gami AS, Somers VK. Obstructive sleep apnea. Ann Intern Med. 2005 Feb 1;142(3):187-97.
10. McNab AA. The eye and sleep apnea. Sleep Med Rev. 2007 Aug;11(4):269-76.
11. Schlotzer-Schrehardt U, Stojkovic M, Hofmann-Rummelt C, et al. The pathogenesis of floppy eyelid syndrome: involvement of matrix metalloproteinases in elastic fiber degradation. Ophthalmology. 2005 Apr;112(4):694-704.
12. Tazaki T, Minoguchi K, Yokoe T, et al. Increased levels of activity and matrix metalloproteinase-9 in obstructive sleep apnea syndrome. Am J Respir Crit Care Med. 2004 Dec 15;170(12):1354-9.
13. Waller EA, Bendel RE, Kaplan J. Sleep disorders and the eye. Mayo Clin Proc. 2008 Nov;83(11):1251-61.
14. Ezra DG, Beaconsfield M, Sira M, et al. Long-term outcomes of surgical approaches to the treatment of floppy eyelid syndrome. Ophthalmology. 2010 Apr;117(4):839-46.
15. Sugita Y, Iijima S, Teshima Y, et al. Marked episodic elevation of cerebrospinal fluid pressure during nocturnal sleep in patients with sleep apnea hypersomnia syndrome. Electroencephalogr Clin Neurophysiol. 1985 Mar;60(3):214-9.
16. Bloomfield RL, Felts JH, Burkhart JM, Cashwell FL. Optic disc edema in a pickwickian man mimicking hypertensive crisis. J Clin Hypertens. 1987 Mar;3(1):27-30.
17. Lee AG, Golnik K, Kardon R, et al. Sleep apnea and intracranial hypertension in men. Ophthalmology. 2002 Mar;109(3):482-5.
18. Javaheri S, Golnik K. Resolution of papilledema associated with OSA treatment. J Clin Sleep Med. 2011 Agu 15;7(4):399-400.
19. Geyer O, Cohen N, Segev E, et al. The prevalence of glaucoma in patients with sleep apnea syndrome: same as in the general population. Am J Ophthalmol. 2003 Dec;136(6):1093-6.
20. McNab AA. Floppy eyelid syndrome and obstructive sleep apnea. Ophthalmol Plast Reconstr Surg. 1997 Jun;13(2):98-114.
21. Mojon DS, Hess CW, Goldblum D, et al. High prevalence of glaucoma in patients with sleep apnea syndrome. Ophthalmology. 1999 May;106(5):1009-12.
22. Mojon DS, Hess CW, Goldblum D, et al. Normal-tension glaucoma is associated with sleep apnea syndrome. Ophthalmologica. 2002 May-Jun;216(3):180-4.
23. Goldblum D, Mathis J, Bohnke M, et al. Nocturnal measurements of intraocular pressure in patients with normal-tension glaucoma and sleep apnea syndrome. Klin Monbl Augenheilkd. 2000 May;216(5):246-9.
24. Lundmark PO, Trope GE, Flanagan JG. The effect of simulated obstructive apnoea on intraocular pressure and pulsatile ocular blood flow in healthy young adults. Br J Ophthalmol. 2003 Nov;87(11):1363-9.
25. Kiekens S, Veva De Groot, Coeckelbergh T, et al. Continuous positive airway pressure therapy is associated with an increase in intraocular pressure in obstructive sleep apnea. Invest Ophthalmol Vis Sci. 2008 Mar;49(3):934-40.
26. Palombi K, Renard E, Levy P, et al. Non-arteritic ischaemic optic neuropathy is nearly systematically associated with obstructive sleep apnoeas. Br J Ophthalmol. 2006 Jul;90(7):879-82.
27. Mojon DS, Hedges TR 3rd, Ehrenberg B, et al. Association between sleep apnea syndrome and nonarteritic anterior ischemic optic neuropathy. Arch Ophthalmol. 2002 May;120(5):601-5.
28. Hayreh SS, Podhajsky PA, Zimmerman B. Nonarteritic anterior ischemic optic neuropathy: time of onset of vision loss. Am J Ophthalmol. 1997 Nov;124(5):641-7.
29. Chou KT, Huang CC, Tsai DC, et al. Sleep apnea and risk of retinal vein occlusion: a nationwide population-based study of Taiwanese. Am J Ophthalmol. 2012 Jul;154(1):200-5.
30. Shiba T, Sato Y, Takahashi M. Relationship between diabetic retinopathy and sleep- disordered breathing. Am J Ophthalmol. 2009 Jun;147(6):1017-21.
31. Shiba T, Takahashi M, Hori Y, et al. Relationship between sleep-disordered breathing and iris and/or angle neovascularization in proliferative diabetic retinopathy cases. Am J Ophthalmol. 2011 Apr;151(4):604-9.
32. Sancho-Chust JN, Chiner E, Lopex-Lizcano R. Central serous chorioretinopathy as first sign of sleep apnea-hypopnea syndrome. Arch Bronconeumol. 2010 Aug;46(8):449-50.
33. Jain AK, Kaines A, Schwartz S. Bilateral central serous chorioretinopathy resolving rapidly with treatment of obstructive sleep apnea. Graefes Arch Clin Exp Ophthalmol. 2010 Jul;248(7):1037-39.
34. Sutton B, Alexander L. Sleep apnea and ocular issues: An Optometric Retina Society white paper. Optometric Retina Society website. Available at:
www.optometricretinasociety.org. Accessed December 2012.

