
History
A 73-year-old white female presented complaining of dry, scratchy eyes. These symptoms, which were worse in her right eye than her left, had been bothering her for six months.
Her ocular history was remarkable for primary open-angle glaucoma O.U. Her systemic history was remarkable for diabetes, hypertension and osteoarthritis, for which she used appropriate systemic medications.
Diagnostic Data
Her best-corrected acuity was 20/30 O.D. and 20/25 O.S. Pupils were equal and round, with no evidence of afferent pupillary defect. Extraocular muscle movements were full and unrestricted. Slit lamp examination revealed diffuse punctate keratitis that was greater O.D. than O.S. Intraocular pressure measured 16mm Hg O.D. and 15mm Hg O.S.
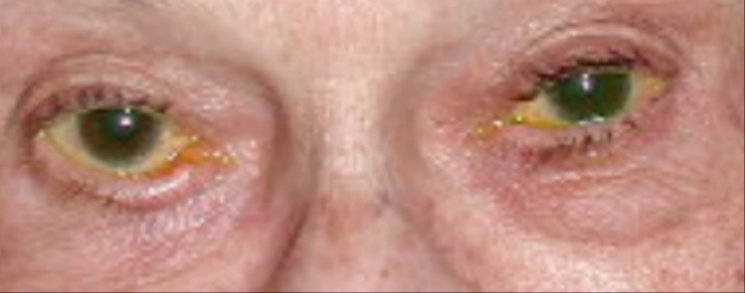
Dilated fundus examination revealed notching of the inferior temporal rim with a corresponding area of nerve fiber layer dropout in both eyes. The photograph below shows the pertinent external examination findings.
A 73-year-old white female patient presented with complaints of dry, scratchy eyes.
Your Diagnosis
How would you approach this case? Does this patient require additional tests? What is your diagnosis? How would you manage this patient? What is the likely prognosis?
Thanks to Dr. Steven Shehan, O.D., of
Discussion
The patient in this issue has ectropion of the right lower lid. Given the risk of severe keratopathy, symblepharon formation and scarring, we referred her to an oculoplastic surgeon for a routine surgical repair, which was completed without complication.
The outward turning of the lid margin typically occurs in the lower lid but can also occur in the upper lid.1 Ectropion is more common in patients of non-Asian decent.1 It can occur in patients of all ages and needs to be distinguished from eyelid retraction.1
There are several possible forms of ectropion:
Involutional ectropion, which is the most common form of ectropion.1,2 It affects the lower lids only and is secondary to changes in lid anatomy due to aging.1,2 The anatomical changes include disinsertion of the lower lid retractors, laxity of the medial and lateral canthal tendons, and atrophy of the orbicularis muscle.1 One study found no difference in muscle fiber type in histological sections of patients with involutional ectropion vs. normal patients.3 Onset is gradual, and the first sign is typically punctal eversion.2 This causes the patient to complain of epiphora, which occurs when tears cannot reach the lower puncta. As the ectropion progresses, the long-term exposure and inflammation of the palpebral conjunctiva causes thickening of the tarsus, leading to worsening of the ectropion, lagophthalmos, exposure keratopathy and ultimately corneal ulceration.2
Congenital ectropion, which is due to a shortage of skin in the eyelids.1,2 This form of ectropion is most commonly associated with Down syndrome, but is also seen in blepharophimosis syndrome, or it can be idiopathic.1,2 Both upper and lower eyelids can be affectedboth lids in Down syndrome and mainly lower lids in blepharophimosis syndrome and idiopathic cases.1
Paralytic ectropion, which results from loss of orbicularis muscle tone secondary to stroke, Bells palsy, facial nerve trauma or in association with a central nervous system neoplasm.1,2 The ectropion is usually most severe medially, due to the area of the insertion of the orbicularis muscle.2
Cicatricial ectropion, which is due to a vertical shortening of the lid skin and orbicularis muscle secondary to skin diseases, scarring from trauma, burns or surgery, or acute allergic skin reactions.1,2 Onset can be gradual or sudden depending upon the etiology.2
Mechanical ectropion, which results when a mass lesion (tumor, conjunctival cyst, edema and/or scar tissue) pulls on the lower lid, displacing it from the globe.1,2
Treatment depends upon the etiology and severity of the patients signs and symptoms. In patients with mild corneal involvement, artificial tears and careful follow-up evaluations are sufficient.1,2 Surgery is recommended in severe cases of patient discomfort or corneal involvement.1,2 Skin grafts are recommended for patients with congenital ectropion.2 For patients with involutional ectropion, surgery to repair the laxity of the lids is recommended.2
Patients with a temporary paralytic ectropion should be monitored until the facial palsy resolves. If the palsy is permanent, surgery is almost always necessary.2 Management of cicatricial and mechanical ectropion involves treating the underlying cause.2
1. Vallabhanath P, Carter SR. Ectropion and entropion. Curr Opin Ophthalmol 2000 Oct;11(5):345-51.
2. Robinson FO, Collin JR. Ectropion. In: Yanoff M, Duker JS. Ophthalmology.
3. Manners RM, Weller RO. Histochemical staining of orbicularis oculi muscle in ectropion and entropion. Eye 1994;8(Pt 3):332-5.

