In attempting to treat wet age-related macular degeneration (AMD), are anti-vascular endothelial growth factor (VEGF) drugs drying the retina too much? Possibly so, according to a recent analysis of results from the Comparison of Age-related Macular Degeneration Treatment Trials (CATT).
 |
Both Avastin (bevacizumab, Genentech) and Lucentis (ranibizumab, Genentech) are equally effective at improving visual acuity in patients with choroidal neovascularization. But within two years of treatment, approximately one-fifth of patients in the CATT study developed geographic atrophy (GA), a cause of progressive visual loss often associated with the dry form of AMD.
The frequency of injections, whether monthly or as-needed, also appears to play a role in GA development.
Ranibizumab Raises Risk
To learn more about the risk of GA, the CATT researchers assessed 1,024 patients in a prospective cohort study to compare two-year treatment with either Avastin or Lucentis. The study patients had no signs of GA before treatment with either therapy—but, by two years, 127 patients developed GA.1
Perhaps more importantly, the type of medicine mattered. Specifically, the study found that patients who received Lucentis were 43% more likely to develop GA than those who received Avastin.
“The differences in the incidence of GA between the two medications could be because of differences in their effects on the retinal pigment epithelium and choroid, or because eyes treated with ranibizumab had more complete resolution of fluid,” the authors wrote.1
 |
|
|
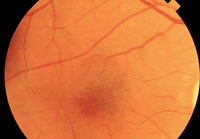
The CATT study confirmed what many clinicians already knew–Avastin is just as effective as Lucentis for the treatment of neovascular AMD, as seen in this patient.
|
Nevertheless, visual acuity was about the same for subjects in either treatment group at two years—but bear in mind that GA had not yet affected the fovea in any subjects. The authors add, “the development and progression of GA may become a more visually important event with longer follow-up of CATT study patients.”
The investigators also acknowledged that the two-year results from a similar study, the Alternative Treatments to Inhibit VEGF in Age-related Choroidal Neovascularization (IVAN) trial, did not show a difference between Lucentis and Avastin in the rates for developing GA (28% for Lucentis vs. 31.2% for Avastin).2 But, this disparity between the two studies is probably because treatment was initiated in the CATT study, unlike in the IVAN trial, as soon as disease activity was noticed.
PRN Better Than Monthly
Scheduling patients for monthly injections no longer appears to be the best approach for AMD patients if a treatment goal is to lower the incidence of geographic atrophy.
The CATT investigators found that monthly injections, regardless of the type of anti-VEGF medication, were associated with a 59% increase in risk of GA development compared with injections administered on an as-needed basis. This indicates that, “greater exposure to anti-VEGF medications may have a role in the development of this condition,” the researchers concluded.1
Another piece of evidence for the dosing risk factor: A group of patients who were switched from monthly injections in the first year of the study to an as-needed basis in the second year showed a decrease in the risk of GA development when they received either drug as-needed in year two. The GA rate in the first year was 12.7% compared to 7% in the second year. This 7% incidence rate was lower than the 8.8% incidence rate of GA in patients who received as-needed injections for both years, suggesting that the dosing regimen affects the incidence of GA in patients on anti-VEGF for wet AMD.1
“Although monthly injections may result in slightly better visual outcomes at two years, the increased risk of GA development may offset this benefit long term,” the investigators concluded.
How Dry is Too Dry?
Because anti-VEGF therapy is used to treat wet AMD, does excessive drying of the retina promote the development of GA? Looking into this, the CATT investigators used optical coherence tomography (OCT) to compare the relative incidence of residual fluid with the relative incidence of GA. They found that the higher the rate of residual fluid on OCT, the lower the rate of GA. “This has led some to speculate that excessive drying of the retina may promote the development of GA,” the authors wrote.
In other words, the dry form of AMD may still progress even though the wet form is suppressed, according to Mark Dunbar, OD, of Bascom Palmer Eye Institute in Miami.
“The reality is that some VEGF may be needed as part of the normal retinal physiology, so when it gets completely shut down—as happens with monthly injections of Lucentis, and to a lesser extent, monthly Avastin—dry AMD may continue to progress, and may in fact be slightly accelerated,” says Dr. Dunbar.
High-Risk Patients
Finally, another practical finding for optometrists is that patients with a worse baseline VA and the presence of GA in the fellow eye have the highest risk of developing GA in their remaining good eye. These high-risk patients should be sent to a retinal specialist who can provide injections on an as-needed basis.
This lower VA could indicate that more layers of the retina are involved or that a greater number of photoreceptors are damaged to begin with. Either way, this information helps us to be more proactive in the management of these patients and provide more realistic expectations.
1. Grunwald JE, Daniel E, Huang J, et al; CATT Research Group. Risk of geographic atrophy in the Age-related Macular Degeneration Treatment Trials. 2014 Jan;121(1):150-161.
2. Chakravarthy U, Harding SP, Rogers CA, et al; IVAN study investigators. Alternative treatments to inhibit VEGF in age-related choroidal neovascularisation: 2-year findings of the IVAN randomised controlled trial. Lancet. 2013 Oct 12;382(9900):1258-67.

