 |
|
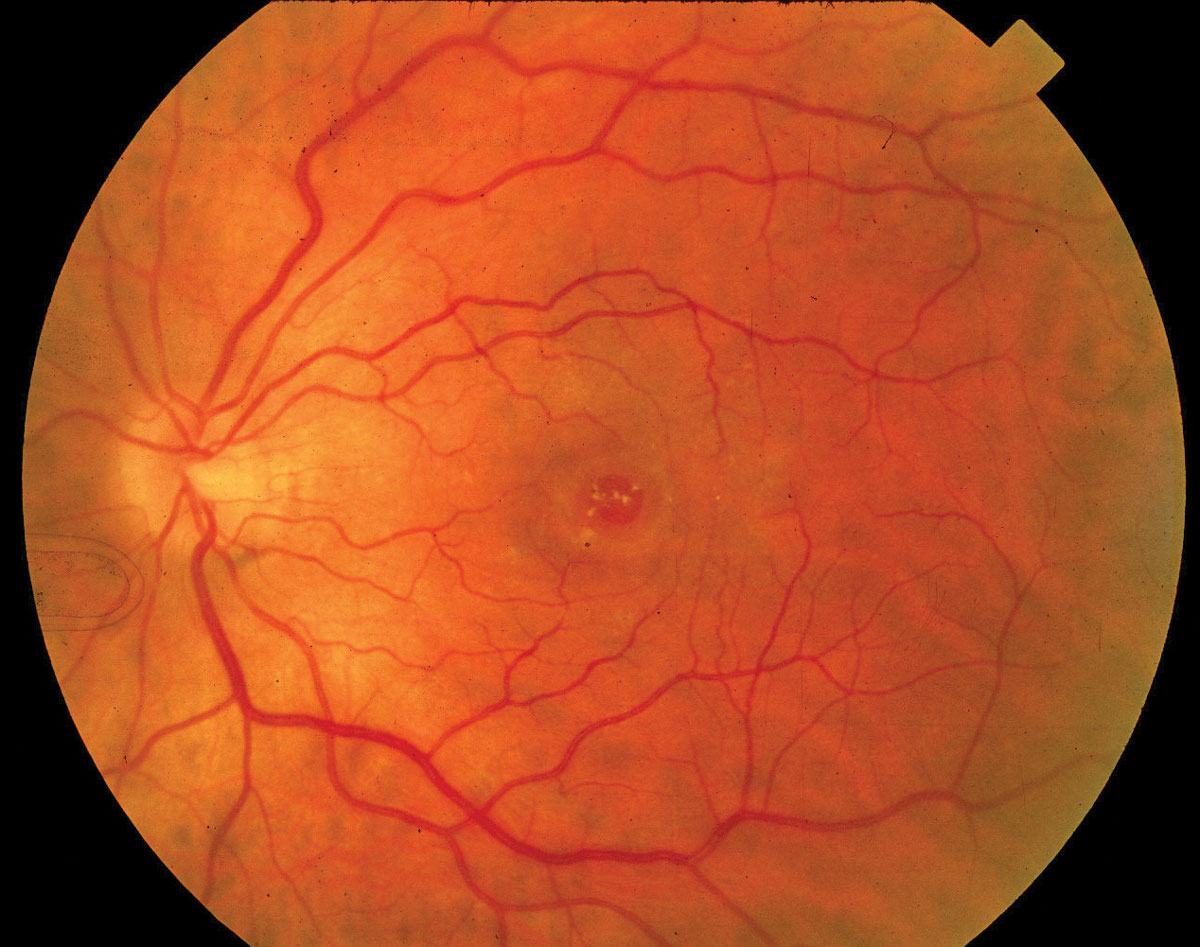
Patients with a full-thickness macular hole fare better after surgery if the procedure is initiated sooner after symptom onset. Photo: Diana Shechtman, OD. Click image to enlarge. |
For patients with an idiopathic full-thickness macular hole, surgery typically repairs the break and improves vision, but the relationship between outcome and symptom duration has remained unclear until now.
In a new meta-analysis of 940 eyes from 940 patients published in the Ophthalmology journal, researchers reviewed 20 years’ worth of findings from randomized control trials conducted between 2000 and 2020. Included were subjects with a full-thickness hole who underwent vitrectomy with gas tamponade. Recorded were the symptom duration, primary hole closure success or failure and postoperative best-corrected visual acuity (BCVA).
Most importantly, the researchers were able to conclude that symptom duration before macular hole surgery displayed a strong and consistent relationship with both poorer anatomical and visual outcomes after operation. Such outcomes included lower hole closure rates and lower final postoperative vision as well as lower BCVA improvement rates after surgery.
Actions that improved hole closure included ILM peeling, intraoperative use of ILM flaps and face-down positioning postoperatively. Vision also improved postoperatively with usage of long-acting gas as a tamponade.
Three characteristics included in the study were patients’ symptom duration, extent of visual acuity loss and the size of the hole, and all three were found to be interrelated. As such, a longer duration of symptoms before surgery was correlated with a larger macular hole size and a worse visual acuity preoperatively.
Rate of enlargement of the hole depended upon the size at presentation, with larger holes growing more slowly than smaller ones. Additionally, small holes were projected to worsen more than bigger holes, due to greater increase of size and visual decline before operation takes place.
The authors highlight the importance of the three components in which the length of time a macular hole has been present can be subdivided: (1) symptom duration at first presentation, (2) time spent in care pathways before a confirmed full-thickness macular hole diagnosis and evaluation by a vitreoretinal surgeon, and (3) the waiting period from diagnosis to surgery.
Because this study indicates that the duration of symptoms before surgery largely affects postoperative anatomical and visual outcomes, the authors urge “the development of prioritization care pathways for people with this condition, to ensure early suspicion (e.g., through increasing public awareness) and prompt diagnosis and treatment (e.g., with effective health care pathways that allow shortening the time between diagnosis and surgery).” Clinicians may want to keep in mind the researchers’ take-home point that, “based on the results of the current study, we advocate prompt referral and surgery for all primary macular holes, especially small ones, as the best means of achieving macular hole closure and good final functional results.”
Murphy DC, Al-Zubaidy M, Lois N, Scott N, Steel DH. The effect of macular hole duration on surgical outcomes: an individual participant data study of randomized controlled trials. Ophthalmology. 2022. [Epub ahead of print]. |

