 In 2005, Medicare beneficiaries were permitted to upgrade from a conventional monofocal intraocular lens to a premium IOL (for presbyopia or astigmatism), as long as they request the additional products/services and are willing to pay all charges beyond those associated with standard cataract surgery. Now, rather than send a claim directly to Medicare for payment, optometrists and ophthalmologists must bill patients directly for these services and the non-covered component of the IOL itself.
In 2005, Medicare beneficiaries were permitted to upgrade from a conventional monofocal intraocular lens to a premium IOL (for presbyopia or astigmatism), as long as they request the additional products/services and are willing to pay all charges beyond those associated with standard cataract surgery. Now, rather than send a claim directly to Medicare for payment, optometrists and ophthalmologists must bill patients directly for these services and the non-covered component of the IOL itself.
Tests Before Cataract Surgery
When the only diagnosis is cataract(s), Medicare does not routinely cover testing other than one comprehensive eye examination and an A-scan or, if medically justified, a B-scan (for a dense cataract). Claims for additional tests are denied as not reasonable and necessary, unless there is an additional diagnosis and the medical necessity for the additional tests is fully documented.
Transfer of Care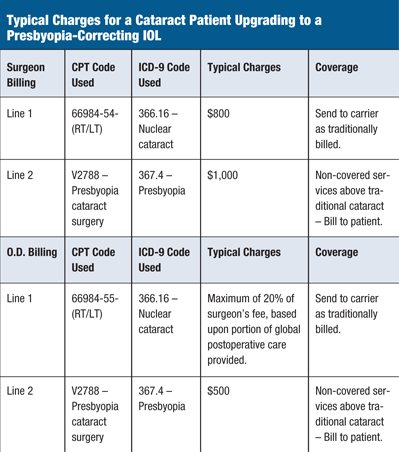
Document the transfer of care in the medical record. The agreement must be in the form of a letter or written as a notation in the discharge summary/hospital records or ambulatory surgical center records. The appropriate CPT-4 modifiers must be added to the surgical procedure code:
- -54 Surgical care only
- -55 Post-op management only
- -79 Unrelated procedure or service by the same physician during the postoperative period.
Pick the Right Surgical Code
CPT code 66984 is for the covered portion of the surgery and IOL. That part of the process should be billed in standard fashion. For the non-covered upgrade, code V2788 should be used to describe the upgrade to a premium IOL. Remember, the patient must always have the option of selecting a conventional monofocal IOL.
Please send your comments to CodingAbstract@gmail.com.

