
If the sky was the limit on your budget, your space and your ability, what diagnostic equipment would you want in your practice? How would it help your patients? How would it benefit your practice?
For this years 31st Annual Diagnostic Technology report, we posed these questions to several specialists in the fields of glaucoma, cornea and retina.
So, if youre building a specialty or referral practice, see what you think about the pieces of technology our panel members dream of.
Whats on Your Wish List?
What new diagnostic instruments have you bought recently?
I purchased the Z-View Aberrometer (Ophthonix) about two years ago, and it has been well worth it. It has allowed me to prescribe high-definition lenses and allowed me to stand apart from the average O.D. And, patients always comment that our practice is always on the cutting edge. New technology is a win-win for both our patients and our practice!
Tommy Lim, O.D.,
Cirrus OCT has not only dramatically increased diagnostic accuracy for retinal conditions and glaucoma, but it has also attracted referrals from other local optometrists and an ophthalmologist as well. I have no doubt that Cirrus, along with my Canon CR-DGi, will build a very positive reputation in the community through patient testimonials/referrals.
Len Ferguson, O.D.,
The HRT and pachymeter have improved the quality of care that I give patients, and they have benefited the practice by generating additional revenue. Also, the patients like the Wow! factor of the HRT images.
Marc Ullman, O.D.,
I recently purchased the Canon Fundus Camera for baseline photos and documentation/determination of progression of retinal pathology. Patient education has been enhanced, because patients understand the scope of care they are receivingI can emphasize that the eye exam covers more than just getting a pair of eyeglasses.
Stephen P. Byrnes, O.D.,
I recently bought a digital video slit lamp for patient education and better patient care. To be able to show the patient exactly what is wrong with their eye is absolutely fantasticespecially on the retina, if the patient has no symptoms. It adds that extra punch behind the diagnosis to hit home to the patient the necessity for proper follow-up care and compliance.
Jeffrey Tipton, O.D.,
Glaucoma
James L. Fanelli, O.D., who practices privately in
HRT-3 is ideal for analyzing optic nerve damage. Also, its retinal module is great at recognizing both progression and change in the retina over time, says Dr. Fanelli. And, HRT-3s TruTrack image alignment software allows the clinician to return to the exact same place on a patients retina at follow-up exams, which allows for precise detection of progression.
Jeff Miller, O.D., who is in private practice in
This machine [Visante OCT] is perfect for measuring the anterior chamber depth and angle, as well as central corneal thickness in glaucoma patients, says Dr. Miller. Also, Visante allows you to perform virtual gonioscopy, which is zero-touch and non-invasive.
Joseph P. Shovlin, O.D., of
Cornea
Everyone has a wish list, says Dr. Shovlin, who edits Reviews Cornea and Contact Lens Q+A and is the clinical editor of Review of Cornea and Contact Lenses. On mine are two things: A confocal microscope and anterior segment OCT imaging.
Dr. Shovlin admires the level of detail possible with a confocal microscope. It would help with the diagnosis of some dreaded corneal diseases, like fungal or protozoan infections. The imaging is just superb. For example, if you have a filamentous fungi infection, you can see the hyphae. If you have a patient with Acanthamoeba keratitis, you can actually see the cysts. It helps you gauge your treatment, because you can see whether youre driving these things deeper into the cornea with topical medication, or whether youre really impacting the way you want to treat these concernsin real time. Confocal microscopy provides a gauge of how youre doing, not just from an initial diagnostic perspective, but from a therapeutic routine perspective.
Christine Sindt, O.D., of
Like Dr. Shovlin, Dr. Sindt also ranks anterior segment OCT imaging high on her list. It takes such a high-resolution scan of the cornea that you can actually see individual layers of the cornea, like a cross-section, says Dr. Sindt. I can see any corneal thinning or edema, or even put a contact lens on the eye and see the saggital depth underneath the lens. The high resolution will be very helpful for contact lens fitting and
following disease progression.
Dr. Shovlin notes that anterior segment OCT could facilitate exams of post-LASIK patients. You could examine the residual bed thickness. Also, you could look at infections to see how deep they are in the cornea, he says. For ophthalmology, its ideal for a practice that does phakic intraocular lensesyou can look at the anatomical considerations, such as the crystalline rise, when determining where to place the lens.
Dr. Sindt uses an aberrometer in her practice, as well. They are very useful when dealing with complaints of blur, or changes in vision with different pupil sizes, or even creating a differential diagnosis regarding visual symptoms. Aberrometry allows you to see the source of the optical distortion; you can decide if its purely corneal or maybe involving the lens or a cataract.
SD-OCT Makes the Call
History
A 71-year-old white male presented for a three-month follow-up examination after being previously diagnosed with dry age-related macular degeneration (AMD) O.U.
The patients best-corrected visual acuity measured 20/40 O.D. and 20/25 O.S. His anterior segment evaluation was unremarkable. The dilated fundus examination was significant for macular drusen formation O.U.
We diagnosed the patient with vitreomacular traction (VMT) O.S., associated with his dry intermediate AMD O.U.
Treatment and Follow-Up
The patient was asked to continue taking his AREDS formula supplements, and to return to the clinic in three months for follow-up.
Retina
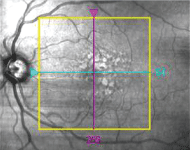
A fundus image of the patient"s left eye. Note the drusen--and note that the vitreous detachment is not visible.
Diagnostic Data
We further analyzed the macular degeneration using spectral-domain optical coherence tomography (SD-OCT). The analysis revealed modulations in the RPE associated with the soft drusen.
Coincidentally, an area of partial vitreous detachment with continuous adherence to the macula was also noted O.S. This was previously undetectable on the fundus exam.
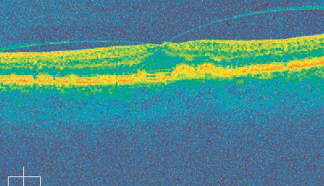
An SD-OCT image of the same eye. Note both the drusen formation and the vistreous detachment.
Diagnosis
Diana L. Shechtman, O.D., of
I have always preferred the use of OCT for retinal imaging over other technologies, she says. OCT is easy for both the clinician and the patient to use, and it is efficient and accurate.
Dr. Shechtman has been especially impressed with the new Cirrus HD-OCT (Carl Zeiss Meditech). Spectral domain provides excellent high-resolution imagery, up to 5m, and fast acquisition speed, up to 27,000 A-scans per second. High resolution and faster acquisition time may allow
you to pick up on subtle defects that may have been overlooked (See SD-OCT Makes the Call).
Dr. Miller agrees with Dr. Shechtmans appreciation for Cirrus HD-OCT. Cirrus HD-OCT is a total upgrade from Stratus OCT (Carl Zeiss Meditech), which relies on time-domain technology, Dr. Miller says. You are able to image each layer of the retina, examine individual tissue layer maps, and obtain advanced visualization with 3-D volume rendering.
Also, a Cirrus scan is much more accurate than a Stratus scan, because Cirrus does not draw upon extrapolated retinal data to fill in the blanksall its data is real.
Dr. Miller also likes Cirrus Auto Patient Recall software, which allows clinicians to precisely reproduce imagery from previous visits and accurately track progression at follow-ups.
In addition to OCT, Dr. Shechtman likes to use ForseePHP for predicting and detecting progression of intermediate AMD to wet AMD.
With the PHP, you are able to detect new onset of visual field defects (associated with wet AMD) prior to noticeable symptoms, she says. Because of this, the PHP may allow you to intervene promptly at an earlier stage of the disease.
While Dr. Shechtman uses some of the latest ophthalmic equipment, she believes that no single piece of technology can ultimately replace clinical experience and skills.
You cannot completely rely on diagnostic technology in your practice, she says. Any data that you generate with your imaging devices should be only part of the patients complete comprehensive eye exam.
When it comes to creating a specialty practice, remember that the equipment you useand the skill you bring to the diagnosisdirectly influences your patient care. (For more on new and upcoming diagnostic technology, see our Technology Survey.)

