Hypertension is one of the most common chronic medical conditions that affects millions of Americans.1 It is a risk factor for premature cardiovascular, renal and cerebrovascular disease, and is responsible for up to seven million deaths a year.1,2 It is estimated that 1% to 2% of individuals with hypertension will present with acute and severe elevations in blood pressure termed “hypertensive crisis.”2 Hypertensive crisis is defined as a systolic blood pressure greater than 179mm Hg or a diastolic blood pressure greater than 109mm Hg.
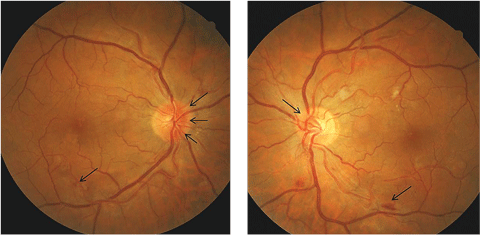 |
| Figs. 1a and 1b. These fundus photos display our patient’s disc edema (as shown with the black arrows) more prominent nasally and in the right eye than in the left. Click image to enlarge. |
Table 1. End Organ Damage in Arterial Hypertension1 | |
Vasculopathy • Endothelial dysfunction | Cerebrovascular Damage • Acute hypertensive encephalopathy |
| Heart Disease • Left ventricular hypertrophy | Nephropathy • Albuminuria |
| 1. Schmieder RE. End Organ Damage In Hypertension. Deutsches Ärzteblatt International. 2010;107(49):866-873. | |
This case report describes a patient who presented from the emergency department with bilateral disc edema with visual field loss secondary to uncontrolled blood pressure.
History
A 44-year-old white male was referred for a visual field deficit from the local emergency department, where he presented with complaints of visual disturbances, dizziness and a headache. His blood pressure was 195/139mm Hg. The patient was started on 10mg IV hydralazine to lower blood pressure over the course of several hours. CT scan of the brain showed an old, right basal ganglia lacunar infarct. The patient had a history of hypertension, but was noncompliant with his medication (due to cost).
Table 2. Clinical Findings | |
| Signs3 | Pathogenesis |
| Arteriolar narrowing/straightening | Due to vasospasm and increased vascular tone. |
| Copper or silver-wire arteriole changes | Results from intimal thickening, media-wall hyperplasia and hyaline degeneration of the arterioles. |
| Arteriovenous crossing changes | Thickened arterioles compress venules. |
| Exudates (Figure 2a) | Break in inner blood-retina barrier. |
| Hemorrhages (Figure 2b) | Break in inner blood-retina barrier. |
| Cotton wool spots (Figure 2b) | Ischemia of the nerve fiber layer due to the damaged retinal microvasculature. |
| Elsching spots | Infarction of segments of the choriocapillaris due to severe hypertension.4 |
| Siegrist streak | Linear RPE hyperplasia over infarcted choroidal arterioles.5 |
| Disc edema | Elevated intracranial pressure, obstruction of axoplasmic flow. |
| 1. Hayreh SS. Hypertensive fundus changes. In: Guyer DR, ed. Retina- Vitreous-Macula. Philadelphia: Sand- ers;1999:354-71. 2. Wong TY, Klein R, Klein BE, et al. Retinal microvascular abnormalities and their relationship with hypertension, cardiovascu- lar disease, and mortality. Surv Ophthalmol 2001;46:59-80. 3. Friedman NJ, Kaiser PK. Ophthalmology The Massachusetts Eye and Ear Infirmary. 3rd ed. 363. 2009. 4. Murphy RP, Lam LA, Chew EY. Hypertension. In: Ryan SJ, editor. Retina. 4th ed., vol. 2. Medical Retina. Philadelphia 2006. 5. Schmidt D, Loffler KU. Elschnig’s spots as a sign of severe hypertension. Ophthalmologica 1993;206:24-8. | |
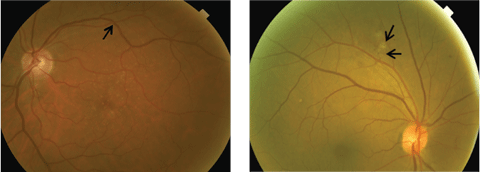 |
| Figs. 2a. and 2b. At left, this fundus image shows arteriovenous crossing changes along superior temporal arcades. At right, this fundus images shows hypertensive retinopathy with retinal hemorrhages and cotton-wool spots. Click image to enlarge. |
We discovered evidence of scattered blot hemorrhages with macular edema, narrowing of arterioles and increased arterial light reflex (Figure 1a). Dilated fundus examination of the left eye showed cup-to-disc ratio of 0.3 with blurred disc margins nasally as well. There was evidence of scattered cotton-wool spots, blot and flame hemorrhages, macular edema, narrowing of arterioles and increased arterial light reflex (Figure 1b).
Diagnosis
Based on these findings, the patient was diagnosed with bilateral disc edema secondary to hypertensive crisis. He was referred back to his primary care provider for blood pressure control and was asked to return in one week for Humphrey 24-2 visual fields. A referral to a retina specialist was recommended due to presence of macular edema. However, the patient declined due to lack of insurance.
At the one-week visit, his visual acuities improved to 20/25-2 OD and 20/20-2 OS. His blood pressure measured 120/80mm Hg. A 24-2 visual field showed right homonymous hemianopia (Figure 3a).
It was unclear if the visual field defect was new or secondary to the pre-existing basal ganglia infarct.
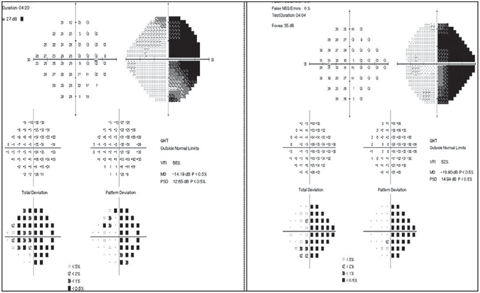 |
| Fig. 3a. 24-2 Humphrey visual field revealed right homonymous hemianopia.Click image to enlarge. |
The patient was asked to return in three weeks to repeat the visual field test and dilated fundus examination. The patient reported an improvement in the vision in his left eye. His visual acuities improved to 20/25+1 OD and 20/20-2 OS. Visual fields showed improvement in the field defect in the right eye with a stable defect in the left (Figure 3b). A dilated fundus examination showed improvement in hemorrhages and cotton-wool spots.
He was advised to continue seeing his primary care provider to maintain control of his blood pressure. We asked him to return in six weeks for a follow-up. He was also referred for a low vision consult due to visual field defects.
Discussion
Chronic and acute hypertension are established risk factors for cardiovascular, cerebrovascular, renal disease, organ damage and significant morbidity.1 According to researchers, patients with a systolic blood pressure greater than 179mm Hg or a diastolic blood pressure greater than 109mm Hg are considered to have a “hypertensive crisis.” The term “malignant hypertension” has been removed from national and international blood pressure control guidelines and the status is best referred to as a hypertensive crisis.1
Hypertensive crises can be further classified as either “hypertensive emergency” or “hypertensive urgency.”2,3 Hypertensive emergency is characterized by severe elevations in blood pressure with acute end-organ damage.3 Hypertensive urgency does not have associated end-organ damage.4
Major end-organ damage can include aortic aneurysm, myocardial infarction, stroke and renal failure (Table 1).
Ocular Complications and Pathogenesis
Retinopathy is the most common sign of hypertension in the eye. The Beaver Dam Eye Study estimated that 10.7% of hypertensive patients older than age 40 have hypertensive retinopathy and, over a five-year follow-up period, 6% of those who had normal retinal exams developed hypertensive retinopathy. A 2001 study suggested a more recent, three-grade classification of hypertensive retinopathy.8,9 In this approach, “mild” hypertensive retinopathy includes generalized and focal arteriolar narrowing, arteriovenous nicking and arteriolar wall opacification. “Moderate” includes mild retinopathy signs plus flame or blot hemorrhages, cotton-wool spots, hard exudates or microaneurysms. “Severe” hypertensive retinopathy includes the signs of moderate retinopathy associated with optic disc swelling.
Table 2 illustrates possible clinical findings in patients with hypertensive retinopathy and their pathogenesis. The patient described in this case report had narrowing of arteries, hemorrhages, cotton-wool spots and bilateral disc edema. The disruption of blood-retinal barrier with degeneration of vascular smooth muscle and endothelial cell necrosis results in blood and exudation in the retina.7,8 Hypertensive choroidopathy can occur in cases of moderate and severe hypertensive retinopathy.
Management
More than 65 million Americans have hypertension, and half of those don’t have it under control.9 Patients with hypertensive retinopathy need to be properly counseled on the underlying condition. Patients with blood pressure of 180/110mm Hg or higher should be referred to the local emergency department.
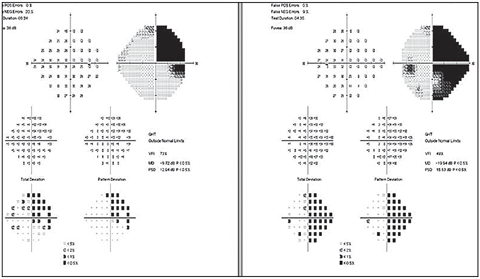 |
| Fig. 3b. Visual field three weeks after initial visit. Visual field in the right eye had improved, but the left remained unchanged. Click image to enlarge. |
It is yet unknown if patients can progress from hypertensive urgency to hypertensive emergency.3,10 The latter requires immediate blood pressure control in an inpatient setting, whereas blood pressure elevation in hypertensive urgency can be reduced more slowly, and inpatient treatment is not necessarily required.15 In hypertensive emergency, blood pressure is titrated by 10% to 25% within the first four hours of intravenous therapy. The goal is to decrease the diastolic blood pressure to between 100mm Hg and 110mm Hg.3
Mild hypertensive retinopathy will typically regress over six to 12 months with strict control of blood pressure under the care of a primary care practitioner. Poor control of blood pressure will delay the regression of retinopathy. A series of case studies show progressive reduction in retinal hemorrhages, exudates, cotton-wool spots and macular star in patients with persistent retinopathy secondary to hypertensive crises with intravitreal bevacizumab injection.12,13
As primary eye care physicians, optometrists may be the first to see hypertensive changes in patients who are undiagnosed with this condition. Routinely checking blood pressure in the optometric practice will assist the clinician to make an appropriate diagnosis and referral in a timely manner.
Dr. Kaur is on staff at Louis Stokes VA Medical Center in Cleveland, Ohio.
|
1. Hajjar I, Kotchen T. Trends in prevalence, awareness, treatment, and control of hypertension in the United States, 1998-2000. JAMA. 2003;290:199-206. 2. Marik P, Varon J. Hypertensive Crisis: Challenges and Management. CHEST. 2007;131:1949-62. 3. Chobanian A, Bakris G, Black H. The seventh report of the joint national committee on prevention, detection, evaluation and treatment of high blood pressure: the JNC 7 report. JAMA 2003; 289: 2560-2572. 4. Rodriguez M, Kumar S, De Caro M. Hypertensive crisis. Cardio Rev. 2010;18: 102-7. 5. Houston M. Hypertensive emergencies and urgencies: pathophysiology and clinical aspects. Am Heart J. 1986;83:131-6. 6. Martin J, Higashiama E, Garcia E, et al. Hypertensive crisis profile. Prevalence and clinical presentation. Arq Bras Cardiol. 2004;83:131-6. 7. Klein R, Klein B, Moss S. The relation of systemic hypertension to changes in the retinal vasculature: the Beaver Dam Eye Study. Trans Am Ophthalmol Soc. 1997;95:329-48. 8. Wong T, McIntosh R. Systemic associations of retinal microvascular signs: a review of recent population-based studies. Ophthal Physiol Opt 2005;25:195–204. 9. Hayreh S. Hypertensive fundus changes. In: Guyer DR, ed. Retina- Vitreous-Macula. Philadelphia: Sanders;1999:354-71. 10. Wong T, Klein R, Klein B, et al. Retinal microvascular abnormalities and their relationship with hypertension, cardiovascular disease, and mortality. Surv Ophthalmol. 2001;46:59-80. 11. CDC. Vital signs: prevalence, treatment, and control of hypertension. United States, 1999-2002 and 2005-2008. MMWR 2011;60(4):103–8. 12. Bender S, Fong M, Heitz S, et al. Characteristics and management of patients presenting to the emergency department with hypertensive urgency. J Clin Hypertens 2006;8:12-8. 13. Bock KD. Regression of retinal vessel changes by anti-hypertensive therapy. Hypertension 1984;6:158-62. 14. Salman AG. Intravitreal bevacizumab in persistent retinopathy secondary to malignant hypertension. Saudi J Ophthalmol. 2013;27:25-9. 15. Al-Halafi AM. Tremendous result of bevacizumab in malignant hypertensive retinopathy. Oman Journal of Ophthalmology. 2015;8:61-3. |

