A 61-year-old Hispanic female, presented to our primary care clinic with a chief complaint of right eye floaters that had degraded her vision during the previous four days.
The patient reported seeing flashes that had subsided in the same eye three months earlier.
Testing eventually confirmed a horseshoe retinal tear that required emergency intervention. Fortunately, laser treatment was arranged—but only after initial work-ups and treatment failed to address her most serious problem.
Our patient’s case showcases one of many different types of retinal tears that you may encounter in practice. Although some patients require an urgent response, others may need prophylactic therapy, monitoring or some other approach.
Here, we discuss many aspects of these complex cases.
Discussion
A retinal detachment is a separation of the neurosensory retina from the retinal pigment epithelium (RPE). The two classifications of retinal detachment, which differ based on underlying etiologies, include tractional/exudative (also known as serous) and hegmatogenous retinal detachment (RRD).
RRD is the most common type of RD. The detachment requires a full-thickness retinal break, vitreous traction and the passage of fluid through the break. The pathogenesis of an RRD may be variable but an acute posterior vitreous detachment (PVD) is commonly the cause.
A total of 67% of patients older than 65 years of age develop a PVD, but most experience no adverse sequelae.1 During a PVD, traction at a site of firm vitreoretinal adhesion may lead to the development of a retinal break. The incidence of retinal breaks is highest during the sixth and seventh decade of life, when PVDs are more prevalent.2 Up to 15% of patients presenting with acute PVDs have concomitant retinal breaks.3-5 Any retinal break can allow passage of liquefied vitreous to gain access into the subretinal space, culminating in an RRD.
Diagnosis
Her ocular history was unremarkable. Her systemic history was positive for hypercholesterolemia, which was controlled with diet and exercise. She was not taking any systemic medications.
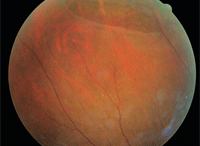
1. A large tear was evident in the
superior retina of the patient’s right eye.
We determined that her best-corrected visual acuity was 20/20, O.D. and O.S. Preliminary testing was unremarkable. Her blood pressure measured 130/80mm Hg at 9:13 a.m. Examination of the anterior segment was unremarkable. Intraocular pressure (IOP) was measured via Goldmann applanation tonometry at 16mm Hg O.D. and O.S.
Dilated fundus examination of the right eye revealed a posterior vitreal detachment, associated with Schaeffer’s sign and an inferior vitreal hemorrhage. A large retinal tear was evident in the superior retina of the right eye (figure 1). Scattered atrophic retinal holes were also observed throughout the periphery.
The left eye revealed moderate syneresis and a second PVD. The periphery of the left eye showed areas of lattice degeneration in both the superior and inferior aspects, including scattered pigmented retinal holes throughout. A retinal tear was noted adjacent to the area of the superior lattice.
We made a STAT referral to a retinal specialist, who lasered both the large retinal tear in the superior periphery of the right eye and the small retinal tear adjacent to the lattice superiorly of the left eye (figures 2 and 3). The lattice inferior area in the left eye and few retinal holes throughout left eye were also treated by the laser.
Symptomatic Treatment
Referring our patient for immediate treatment was a critical step in safeguarding her vision. About 30% of symptomatic, untreated retinal breaks result in an RRD.6-8
Therapy of retinal breaks started in 1920, when Gonin’s work led to the recognition that a retinal break was the cause of an RRD and that treatment of the RRD would require the sealing of such breaks.9 In 1950, with the advent of the xenon laser, prophylactic treatment of all retinal breaks was recommended to prevent an RRD.10,11
Since then, several studies have evaluated the natural progression of retinal breaks. It has been documented that the overall clinical picture, including the type of break and symptomatology, are critical prognostic indicators for the development of RRD.
Variable accompanying signs, symptoms, risk factors and break types need to be considered to make the proper recommendation (see tables 1-3).
The American Optometric Association (AOA) guidelines recommend referral for symptomatic retinal breaks for prophylactic laser treatment in many cases.12 The guidelines are based on the increased likelihood of progression toward an RRD. This protocol is linked to prospective clinical studies that evaluated the natural history of retinal breaks, overall risk factors toward the progression of an RRD, type of retinal break present, as well as guidelines for retinal break treatment developed by the American Academy of Ophthalmology.
Despite this protocol, however, controversy persists.
Asymptomatic retinal breaks have shown insignificant conversion to the development of an RRD.13-15 The prevalence of retinal breaks in the general population is about 6%, contrasted with 0.1% for RRD.16,17 Therefore, most asymptomatic retinal breaks are commonly managed by continuous monitoring unless the patient has additional findings or symptoms that may indicate an increased risk of developing an RRD.
Follow-up
During a two-week follow up examination of our patient, she complained of photopsia in the right eye. Anterior segment evaluation revealed trace cells in the anterior chambers of both eyes. IOPs measured via Goldmann applanation tonometry was 12mm Hg and 11mm Hg, O.D. and O.S., respectively.
Dilated fundus examination revealed a horseshoe tear in the inferior aspect of the mid-periphery of the right eye, approximately 180° away from the previous laser surgery (the superior retinal tear). The laser scars from the treatment two weeks earlier appeared stable. Management included a STAT referral back to the retinal surgeon, who treated our patient in the area surrounding the horseshoe tear with a laser treatment in the right eye.
A retinal flap tear, also known as a horseshoe or U-shaped tear, commonly occurs in association with a PVD formation. This type of tear develops when the posterior hyaloid membrane continues to adhere to the retina as the PVD attempts to separate more anteriorly, creating a U-shaped or horseshoe tear with a triangular appearance.
Typically, the apex of the tear points towards the posterior pole and the flap points toward the vitreous base, which still adheres to the vitreous. Most flap tears are found just anterior to the equator of the globe, commonly in the superotemporal quadrant. Because of the associated vitreoretinal traction, flap tears are more likely to lead to RRDs.
Flap tears are the most common type of breaks in RRD patients.19
Additional Retinal Breaks
Besides the horseshoe tear that was affecting her, you may also see retinal holes. The sizes of these red, round, and full-thickness retinal defects range from pinpoint to 1.5 disc in diameter. Below are descriptions of two types you might find:
• Atropic retinal holes. The underlying cause of these defects is a poorly functioning choriocapillaris that no longer gives adequate circulation to the retinal layers above the hole. This chronic thinning and decompensation of the chorioretinal blood supply has a domino-like effect on the overlying neurosensory retina, resulting in thinning. Atrophic holes may be found in isolation, within areas of lattice degeneration, (LD) or adjacent to LD (18% to 42%).5

Isolated retinal holes are often localized at the posterior aspect of the vitreous base, posing the lowest propensity for RRDs. When localized within the lattice, they are associated with a very low incidence of retinal detachment. Fewer than 1% of cases of lattice degeneration with holes progress to RRD.15 When they are localized adjacent to LD, there is a slightly higher incidence of RRD because of increased vitreoretinal traction. Overall, atrophic retinal holes are seldom linked as an etiology of RRD. Management typically includes monitoring twice a year or once a year, depending on associated clinical presentation.
• Operculated retinal holes. These holes have the same clinical appearance as atrophic retinal holes. But operculated holes also have an overlying free-floating plug of retinal tissue (operculum) that adheres to the posterior hyaloid of the vitreous. Unlike the pathogenesis of an atrophic retinal hole, the operculated retinal hole results from increased focal vitreoretinal traction. Avulsion of the retinal tissue moving in a forward direction results in the free-floating operculum. The operculum, which can be seen as a whitish disc-shaped floater, remains attached to the posterior hyaloid membrane overlying the retinal hole.
With time, the operculum contracts and deteriorates because of loss of retinal blood supply. In many cases, it is observed to be smaller than the underlying retinal defect. The development of an operculated retinal hole will most likely be a sudden event, rather than a progressive process occurring during the formation of a PVD. In addition, vitreoretinal tufts commonly precede the operculated retinal hole.
Patients may be symptomatic in the initial phase of an operculated retinal hole development, but become asymptomatic once the operculum is fully formed and traction is released. The absence of vitreoretinal traction after the operculum becomes free floating translates into a very low risk for the development of a RRD. No treatment is necessary.12
If there is persistent vitreoretinal traction, an operculated retinal hole can lead to an RRD. However, fewer than 1% of asymptomatic operculated retinal holes develop into RDs.7 Treatment is considered for fresh operculated holes that are large and superiorly located, or for cases associated with ominous signs, such as a vitreous hemorrhage.12
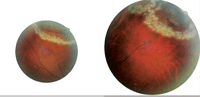
2, 3. A retinal specialist lasered both the large retinal tear in the superior periphery of the right eye and the small retinal tear adjacent to the lattice superiorly of the left eye.
Second Follow-up
Our patient’s case illustrated how much care must be taken to ensure that RD is managed effectively. When returning for a second follow-up visit two weeks after her laser treatments, she complained of increased flashes and floaters again. Dilated examination of the left eye revealed vitreal traction on the inferior aspect of her lattice degeneration.
After this visit, she received peripheral laser treatment, 360° in both eyes, as a precautionary measure.
Variable Management Options
Recommendations for the management of retinal breaks are clearly varied. Some retinal breaks are exclusively treated, such as a symptomatic flap tears, and other retinal breaks merely requires yearly follow up visits, such as atrophic retinal holes.7,20
The literature does not provide enough consensus to guide management of an asymptomatic flap tear. But, at least 50% of untreated symptomatic retinal horseshoe or flap tears accompanied by persistent vitreoretinal traction will cause a clinical RD, unless the patient is treated.19-21 Thus, urgent treatment of these tears is crucial. Prompt creation of a chorioretinal adhesion around these symptomatic tears reduces the chances of RD to less than 5%.21 Even an asymptomatic horseshoe tear can result in RRD. Approximately 5% progress to retinal detachment, making the timely diagnosis of this condition extremely important.18
In 1974, Byer reported in his series of retinal breaks that not a single asymptomatic retinal break progressed to a clinical RRD.20 Sixty percent of these retinal breaks were identified as asymptomatic flap tears. Yet, other studies have shown that asymptomatic retinal breaks (such as asymptomatic flap tears) can lead to RRD.2,18

The lack of agreement in the literature adds to the challenge of management guidelines of certain retinal breaks. AOA recommendations can help manage variable presentations.12 In the presence of a retinal break, multiple risk factors are associated with greater propensity toward the development of a RRD. All signs and symptoms should be taken into account, depending on the presenting clinical picture and associated risk factors. Although most asymptomatic, uncomplicated retinal breaks are simply monitored, consider referrals for patients presenting with predisposing risk factors.13,14,22 For example, a patient with a history of retinal detachment has a 10% risk of detachment in the other eye in the presence of a retinal break.2,23,24
Early Detection, Timely Referrals
Early detection and timely referrals of retinal breaks are critical. Treatment of retinal breaks with laser photocoagulation may be
necessary to prevent the development of RRDs. The decision to treat is anecdotal, depending on the type of break and the overall clinical picture, as well as risk factors. A good case history, careful dilated eye examination, with perhaps scleral depression, are critical to make the proper recommendations to our patients.

1. Foos RY, Wheeler NC. Vitreoretinal junction: Synchysis senilis and posterior vitreous detachment. PVD. Ophthlamol 1982;89(12):1502-12.
2. Combs JL, Welch RB. Retinal breaks without detachment: natural history, management, and long-term follow-up. Trans Am Ophthalmol 1982;80:64-97.
3. Lindner K. The prevention of spontaneous retinal detachment. Arch Ophthalmol 1934;11:148.
4. Jaffe NS. Complications of acute posterior vitreous detachment. Arch Ophthalmol 1968:79(5):568-71.
5. Tasman WS. Peripheral Retinal Lesions. In: Ophthalmology, 2nd edition. Yanoff M (ed.). Philadelphia: Mosby; 2004.
6. Colyear BH, Pischel DK. Preventive treatment of retinal detachment by means of light coagulation. Pac Coast Oto Ophthalmol Soc 1960;40:193-215.
7. Davis MD. The natural history of retinal breaks without detachment. Trans Am Ophthalmol Soc. 1973;71:343-72.
8. Shea M, Davis MD, Kamel I. Retinal breaks without detachment, treated & untreated. Mod Prol Ophthalmol. 1974;12: 97-102.
9. Gonin J. La thermoponction oblitιrante des dιchirures rιtiniennes dans le dιcollement de la rιtine. Ann Oculist. 1931;168:1-29.
10. Meyer-Schwickerath G. Indications & limitations of light coagulation. Trans Am Acad Ophthalmol Otolagyngol. 1959;62:725-38.
11. Guerry D, Wiesinger H: Experiences with light coagulation of fundus lesions. Trans Am Ophthalmol Soc 1959;57:109-25.
12. American Optometric Association. Optometric clinical practice guidelines. Care of the patient with retinal detachment and related peripheral vitreoretinal disease. Available at: www.aoa.org/documents/CPG-13.pdf (Accessed August 29, 2010).
13. Davis MD. Natural history of retinal breaks without detachment. Arch Ophthalmol 1974;92(3):183-94.
14. Neumann E, Hyams S. Conservative management of RB. Br J Ophthalmol. 1972;56(6):482-6.
15. Byer NE. What happens to untreated asymptomatic RD, and are they affected by PVD? Ophthalmol 1998;105(6):1045-50.
16. Haimann MH, Burton TC, Brown CK. Epidemiology of retinal detachment. Arch Ophthalmol. 1982;100(2):289-92.
17. Wilkes SR, Beard CM, Kurland LT, et al. The incidence of retinal detachment in Rochester, Minnesota, 1970-1978. Am J Ophthalmol. 1982;94(5):670-3.
18. Wilkinson CP. Evidence-based analysis of prophylactic treatment of asymptomatic retinal breaks and lattice degeneration. Ophthalmology 2000;107(1):12-5.
19. Tielsch JM, Legro MW, Cassard SD, et al. Risk factors for retinal detachment after cataract surgery. A population-based case-control study. Ophthalmology 1996;103(10):1537-45.
20. Byer NE. Prognosis of asymptomatic retinal breaks. Arch Ophthalmol. 1974;92(3):208-10.
21. Rowe JA, Erie JC, Baratz KH, et al. Retinal detachment in Olmsted County, Minnesota, 1976 through 1995. Ophthalmology 1999;106(1):154-9.
22. Coffee RE, Westfall AC, Davis GH, et al. Symptomatic posterior vitreous detachment and the incidence of delayed retinal breaks: case series and meta-analysis. Am J Ophthalmol 2007;144(3):409-13.
23. Byer NE. The natural history of asymptomatic retinal breaks. Ophthalmology 1982;89(9):1033-9.
24. Delaney WV, Oates RP. Retinal Detachment in the second eye. Arch Ophthalmol. 1978;96(4):629-34.

