When a “new layer” of the cornea was reported last month, it made headlines in the scientific and lay press. Some even went so far as to say that ophthalmic textbooks will need to be rewritten.

But, what is its significance—if any—for primary eye care?
At issue: Researchers in the UK have described a newly discovered and very thin layer of the cornea.1 It has been dubbed “Dua’s layer” after its main discoverer, Harminder S. Dua, MD, PhD, professor of ophthalmology and visual sciences at the University of Nottingham. It’s a tough, well-defined, acellular lining only about 10μm to 15μm thick, sandwiched between the corneal stroma and Descemet’s membrane (DM).
“In the operation of deep anterior lamellar keratoplasty (DALK), surgeons were observing ‘things’ that they could not make sense of,” Dr. Dua says. After performing various lamellar corneal surgeries—corneal transplants, in particular—Dr. Dua hypothesized that another layer of the cornea might exist to cause these phenomena. To confirm this, he and his colleagues simulated corneal transplants by injecting air into corneal grafts to carefully separate the distinct layers of the cornea. Then, they closely examined the layers using electron microscopy.
They found that the separation of layers that yielded the strongest tissue was not between the stroma and the DM, as believed. Rather, the ideal separation was between the deep stroma and this unrecognized layer.
“Thus far, all surgeons thought that they were separating the DM from the stroma in the operation of DALK. We have proved that this is not so, but that this new layer offers the plane of cleavage in most cases,” Dr. Dua says. “And, because this layer is so tough, it keeps the eye much stronger than it would have been if only DM was left behind. Knowledge of this layer will now enable surgeons to understand the operation better and make it safer with improved patient outcomes.”
For instance, graft tissue composed specifically of endothelium, DM and Dua’s layer could be used in endothelial keratoplasty. This may allow a better and more easily performed method of this procedure, with fewer grafts wasted due to tears in the DM, Dr. Dua says.
Also, the discovery of this layer may have implications in such conditions as descemetocele (protrusion of Descemet’s membrane through the cornea) and acute corneal hydrops in keratoconus (edema due to spontaneous rupture in Descemet’s membrane—and possibly Dua’s layer).
Incidentally, Dr. Dua may not have been the first to report this layer. A paper published in 1991 by Perry Binder, MD, describes a network of fibers located at the interface of the posterior stroma and DM, although it was not identified as a distinct corneal layer.2 When contacted for his perspective,
Dr. Binder, who is currently a clinical professor of ophthalmology at Gavin Herbert Eye Institute, University of California–Irvine, declined to comment for this story.
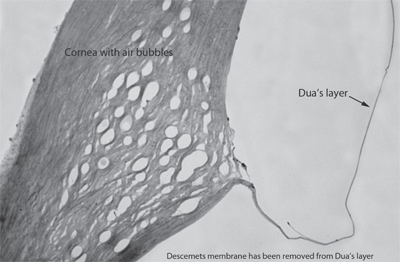
To find Dua’s layer, researchers injected air into corneal grafts to carefully separate the layers of the cornea, then inspected the layers under an electron microscope. Photo: Harminder S. Dua, MD, PhD
For now, Dr. Dua and his team will be putting the layer to the test—literally. “The bursting pressure of this layer is around 700mm to 900mm Hg,” he says. “We are currently building a [more] sensitive pressure gauge and should have more accurate figures in the not too distant future. When the layer bursts, it does so with a pretty loud popping sound … suggesting its strength.”
Dr. Dua suggests that this is an important discovery, with wide-ranging implications. But he denies a quote in the lay press attributed to him: “This is a major discovery that will mean that ophthalmology textbooks will literally need to be re-written.”
But will optometry textbooks need to be re-written? No need to stop the presses just yet, it seems.
“As Dr. Dua mentions, knowledge of the existence of this layer may help with our understanding of why certain keratoconus patients develop corneal hydrops and why certain patients with descemetoceles don’t experience a rupture,” says John Pole, OD, MS, professor at Michigan College of Optometry, Ferris State University. “In the fall, when I teach my students corneal anatomy and physiology, I will mention that there is a suggestion of a new corneal layer and that its importance seems to be related to the new corneal transplantation procedures. [But] its impact on primary care at this time will be small.”
1. Dua HS, Faraj LA, Said DG, Gray T, Lowe J. Human corneal anatomy redefined: a novel pre-Descemet’s layer (Dua’s layer). Ophthalmology. 2013 May 25. [Epub ahead of print]
2. Binder PS, Rock ME, Schmidt KC, Anderson JA. High-voltage electron microscopy of normal human cornea. Invest Ophthalmol Vis Sci. 1991 Jul;32(8):2234-43.

