
History
A 73-year-old white male presented for a routine eye examination without visual or ocular complaints. His ocular history was remarkable for age-related macular degeneration (AMD). Systemic history was noncontributory.
Diagnostic Data
His best-corrected acuity was 20/40 O.D. and 20/30 O.S. at distance and near. External examination was normal, and there was no evidence of afferent pupillary defect.
Anterior segment findings demonstrated cataract, open angles and normal corneas. IOP measured 13mm Hg in both eyes.
The pertinent fundus findings, along with the corresponding visual fields, are demonstrated in the photograph, though the pallor of the temporal disc O.S. may not be apparent.
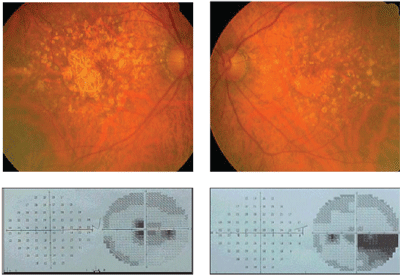 |
| Dilated fundus photography demonstrated this appearance, O.D. (left) and O.S. (right). Pallor of the temporal disc in the left eye may not be apparent. |
Your Diagnosis
How would you approach this case? Does this patient require additional tests? What is your diagnosis?
How would you manage this patient? What is the likely prognosis?
Thanks to Jason M. Savochka, O.D., of Kremer Laser Eye Surgery Center in Cherry Hill, N.J., for contributing this case.
Discussion
Additional testing might include central threshold visual field testing, color vision testing, fluorescein angiography, carotid auscultation, carotid duplex ultrasonography and neuroimaging.
The macular diagnosis in this case is central areolar choroidal degeneration (CACD), a variant of dry AMD. CACD usually affects patients in the fifth decade and consists of circumscribed atrophy of the choriocapillaris, photoreceptors and retinal pigment epithelium.1 CACD is responsible for the visual field defect in the patients right eye. The defect in the left eye is due to a combination of the maculopathy and an old non-arteritic ischemic optic neuropathy (NAION). The marked pallor of the disc indicates infarct.
What makes this case interesting is that the vision loss caused by the NAION went unnoticed because the maculopathy had already compromised the central acuity.
NAION is often found in patients who have hypertension and is often produced by emboli or atherosclerotic disease.2 Management involves treating the underlying systemic disease, so this patient was worked up for diabetes, hypertension, hypercoagulable state, infection, inflammation, dyslipidemia, and cardiac and carotid disease. The tests showed that the patient had systemic hypertension that required intervention. He was managed hemodynamically with aspirin.
1. Nagasaka K, Horiguchi M, Shimada Y, Yuzawa M. Multifocal electroretinograms in cases of central areolar choroidal dystrophy. Invest Ophthalmol Vis Sci 2003 Apr;44(4):1673-9.
2. Kim SK, Volpe NJ, Stoltz RA. Contemporaneous retinal and optic nerve infarcts, choroidal non-perfusion, and Hollenhorst plaque: Are these all embolic events? J Neuroophthalmol 2006 Jun;26(2):113-6.

