 |
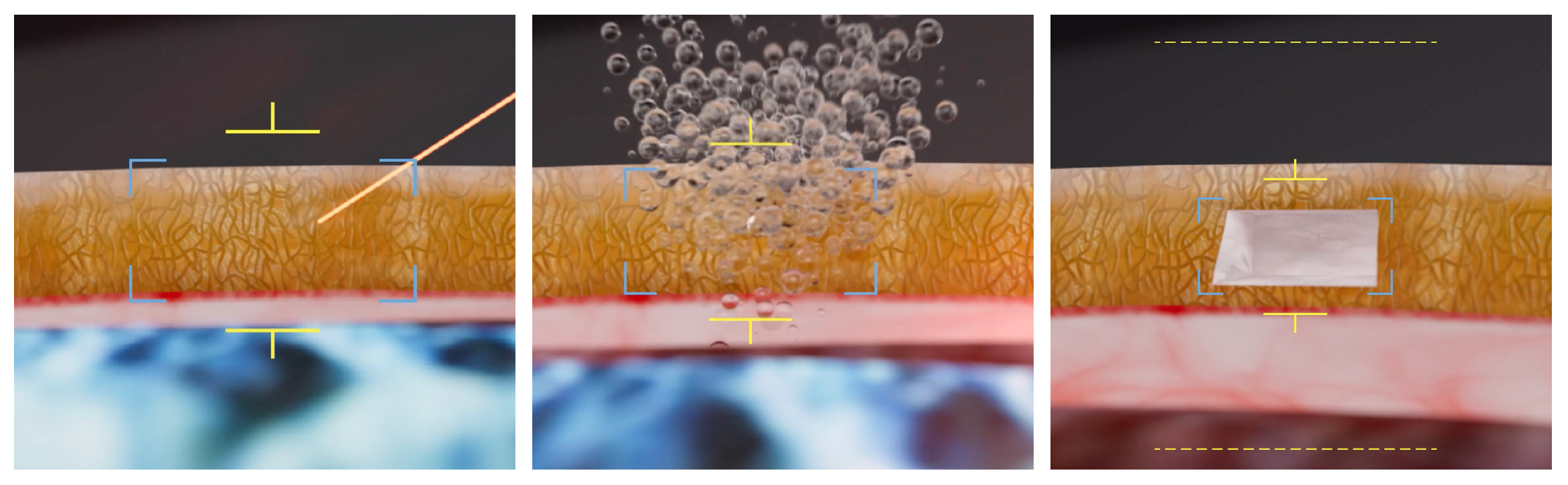
No serious adverse events came from FLIGHT, which could be an alternative to MIGS for patients with glaucoma. Photo: ViaLase. Click image to enlarge. |
As it stands, all MIGS glaucoma procedures are invasive to some degree, but are usually meant to piggyback on top of cataract surgery to minimize the added trauma. Can any glaucoma surgeries be truly noninvasive? One group of developers claims to be making headway. The results of a pilot study recently published in Ophthalmology Science describe a new procedure called femtosecond laser image-guided high-precision trabeculotomy (FLIGHT), which showed a favorable safety profile with no device-related serious adverse events after two years.
The procedure, developed by a company called ViaLase, is designed to noninvasively create a channel connecting the anterior chamber to Schlemm’s canal, bypassing aqueous humor outflow resistance. The company funded the study and all six authors are either consultants for or employees of ViaLase.
“A custom-engineered optical scanning system enables the delivery of tightly focused femtosecond laser pulses through the cornea and into the iridocorneal angle, thus permitting precise photodisruption of the trabecular meshwork,” the study authors wrote in their paper.
Eighteen eyes from 12 patients underwent the procedure, which created a single channel measuring 500μm wide by 200μm high through the trabecular meshwork and into Schlemm’s canal. According to the study authors, there were instances of minor blood reflux in 11 eyes immediately after surgery, which all resolved by day one post-op. Adverse events, intraocular pressure (IOP) and other parameters were evaluated out to 24 months.
In the 11 patients (17 eyes) who returned at 24 months, the researchers found no serious adverse events related to the laser treatment. Well-defined channels were clearly visible at 24 months by gonioscopy and AS-OCT, with no evidence of closure. At 24 months, mean IOP was reduced by 34.6% from 22.3mm Hg to 14.5mm Hg with an average of two hypotensive medications compared with 2.2 at baseline. Notably, 14 out of the 17 study eyes (82.3%) achieved 20% or greater reduction in IOP at 24 months when compared with baseline.
The researchers believe that the level of IOP reduction in the current study (34.6%) has the potential to be comparable with numerous trabecular meshwork outflow procedures.
“FLIGHT does not require opening the eye and only treats about 5° of the angle, which reduces the potential for harm to the eye,” they wrote in their paper. “The ability to noninvasively create a conduit between Schlemm’s canal and the anterior chamber, thus creating direct communication between the aqueous humor and the collector channels, is an advantage unique to FLIGHT technology,” they asserted.
The ability to perform FLIGHT in narrow angles is unknown. Narrower angles could make visualization of the trabecular meshwork more difficult, and there would be increased risk of iris incarceration following channel creation. The researchers suggest further investigation in these eyes is needed to assess these questions.
“Clinical studies are underway to further evaluate safety and to rigorously evaluate the efficacy of FLIGHT,” the team concluded in their paper. “Specifically, an appropriately powered, multicenter, randomized controlled study in a washed-out patient population of greater gender and racial diversity is necessary to understand the effects of femtosecond laser trabeculotomy.”
Nagy ZZ, Kranitz K, Ahmed IIK, et al. First-in-human safety study of femtosecond laser image guided trabeculotomy for glaucoma treatment: 24-month outcomes. Ophthalmol Sci. April 17, 2023. [Epub ahead of print]. |

