 |
Patients frequently present with bothersome blepharoptosis, but in the absence of pharmacologic options, optometrists could historically do little to improve their appearance or functioning. However, late last year, the FDA accepted a promising New Drug Application that, if approved, may soon alter the landscape of ptosis care as we know it.
Etiology and Subtypes
Blepharoptosis is a common condition defined by either unilateral or bilateral eyelid drooping.1 It can affect individuals of all ages and is caused by weakness of the levator palpebrae superioris and Müller’s muscle, which are responsible for lifting the eyelid, or by a pathology of the nerves that cause innervation these muscles.1,2
Ptosis can be either acquired or congenital. The congenital form is the most common cause in children. It’s defined as ptosis present at birth or that develops by age one.1 Congenital blepharoptosis subtypes include blepharophimosis syndrome, congenital third cranial nerve (CN III) palsy, congenital Horner’s syndrome, and Marcus Gunn jaw-winking syndrome.3 Approximately 75% of congenital ptosis is unilateral, and leads to amblyopia in 20% of cases either due to occlusion of the pupil or by causing amblyogenic astigmatism in the affected eye.1,4
Acquired blepharoptosis can be divided into five subtypes:5
- Aponeurotic ptosis. This is the most common form of acquired ptosis.1 It occurs secondary to stretching or dehiscence of the levator aponeurosis, typically acquired with repetitive traction or involution of the tissue. These patients present with a reduced margin to reflex distance 1 (MRD1), a high upper eyelid crease, a near normal levator function (LF), and decreased palpebral fissure in downgaze.1
- Neurogenic ptosis. This form of blepharoptosis may result from CN III palsy or Horner’s syndrome.3
- Myogenic ptosis. Myogenic blepharoptosis can be found in myasthenia gravis (MG), chronic progressive external ophthalmoplegia, oculopharyngeal muscular dystrophy and myotonic dystrophy patients.3
- Mechanical ptosis. This can result from the presence of eyelid mass, such as neurofibroma or hemangioma or cicatrization secondary to inflammation or surgery.1
- Traumatic ptosis. Eyelid laceration with transection of the upper eyelid levators, or any disruption of the neural pathway can cause this type of acquired ptosis.3
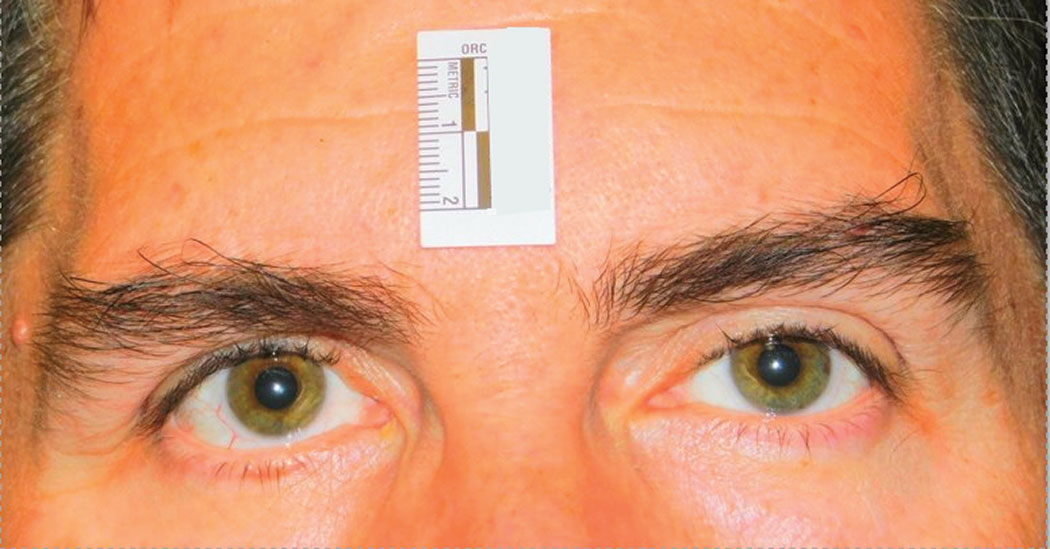 |
| This clinical study subject is seen five minutes after instillation of RVL-1201 for the treatment of ptosis. Click image to enlarge. |
Diagnosis
Identifying ptosis is critical for neurologic and visual function. Ptosis is present when the upper eyelid is lower than its normal anatomical position, typically 1mm to 2mm below the superior corneoscleral limbus.1,2 Evaluating the MRD1 can help determine the presence of ptosis, as well as its severity.3 A normal value for MRD1 is 3.5mm to 5.0mm.3 Levator function is also important and is a primary determinant of surgical technique. It is measured as the total excursion of the upper eyelid margin from maximum downgaze to maximum upgaze. A normal value is between 13mm Hg and 16mm Hg.1
Ptosis can foretell some potentially serious underlying conditions, such as Horner’s syndrome and CN III palsy.1 Research shows 20% of MG patients experience isolated ocular symptoms and 80% of patients who initially present with ocular MG develop systemic symptoms.1,2
Horner’s syndrome results from a disruption in the sympathetic nervous system pathway extending between the brain and the Müller’s muscle, affecting the eye and ipsilateral side of the face.3 While ptosis, miosis and anhydrosis are the classic Horner’s syndrome triad, these clinical signs may be subtle and are rarely all present.1
Cosmetic botulinum toxin type A injection patients may also present with ptosis complaints. Here, upper lid ptosis occurs when the toxin diffuses through the orbital septum and affects the levator muscle as it traverses the pre-periosteal plane or when the toxin tracks along tributaries of the superior ophthalmic vein.1 The side effects of this can persist for the whole duration of effect of treatment, but usually settle in three to four weeks.4
Finally, be sure to distinguish blepharoptosis from dermatochalasis.5 Although true ptosis correction often requires surgery to elevate the position of the upper eyelid margin, isolated dermatochalasis can be corrected by removal of excessive skin with or without fat debulking or redistribution.6 Importantly, correcting the ptosis alone may worsen the dermatochalasis as elevating the upper eyelid margin can increase the redundancy of the overlying skin. For this reason, some patients with both ptosis and dermatochalasis benefit from combined ptosis repair and upper lid blepharoplasty.6
Surgical Options
The primary surgical approaches for ptosis include Müller’s muscle-conjunctival resection, levator resection and the frontalis sling.1 Levator function, the degree of ptosis and the patient’s response to phenylephrine can help guide the surgeon select a surgical approach.1
Surgical ptosis correction can be performed at any age depending on the severity of the disease.3 However, if the patient has strabismus and blepharoptosis, the strabismus must be corrected first.3 A phenylephrine test can help determine if patients are good candidates for a conjunctivo-mullerectomy.1 As an alpha-adrenergic agonist, phenylephrine stimulates the sympathetically innervated Müller’s muscle when applied topically.3
Pharmaceutical Treatments
ODs can consider one of three medical treatments for ptosis: apraclonidine ophthalmic drops, botulinum toxin injection and oxymetazoline.
Apraclonidine is not an appropriate long-term treatment for blepharoptosis, as it may cause sensitivity with longer-term use, but since upper eyelid ptosis after cosmetic botulinum toxin is generally short-lived and may be responsive to apraclonidine ophthalmic drops, this treatment is appropriate in cases of inadvertent migration of botulinum toxin injection into the levator palpebrae superioris muscle.3,4
In addition to creating a need for ptosis treatment, botulinum toxin injection is also a plausible treatment itself. As a neuromuscular-blocking agent, botulinum toxins weaken targeted muscles by inhibiting the release of acetylcholine from the presynaptic terminal of the neuromuscular junction.4 As such, it can be a suitable option for the management of small eyelid margin asymmetries.5 Indeed, with mild or micro-ptosis, surgery is rarely indicated for functional purposes and, in some cases, surgery can lead to secondary aesthetic complications, such as contour asymmetry or crease abnormalities.6 In these cases, botulinum neurotoxin may be a desirable nonsurgical treatment option.6,7 However, note that treatment is dose-dependent and large doses may induce complications, such as lagopthalmos, exposure keratitis and inadvertent induction or worsening of ptosis.3
More recently, researchers have been looking into RVL-1201 (oxymetazoline 0.1%, Vertical Pharmaceuticals) for use in patients with acquired ptosis.3 Oxymetazoline is an ɑ1 and partial ɑ2 adrenergic agonist capable of contracting Müller’s muscle through direct transconjunctival contact of this sympathomimetic agent.3 In a Phase III study, the treatment was well tolerated and significantly improved the superior visual field, making this emerging therapy a potential nonsurgical treatment for upper eyelid ptosis.1,3
Optometrists are the first line of care for ptosis patients, yet we’ve had little opportunity to apply our deep understanding of the condition to approved treatments. Given the incidence of ptosis in the aging population, having an approved therapy—should it come to pass—will be a tremendous benefit in terms of providing comprehensive primary eye care.
| 1. Patel K, Carballo S, Thompson L. Ptosis. Dis Mon. 2017 Mar;63(3):74-79. 2. Pavone P, Cho SY, Praticò AD, et al. Ptosis in childhood: A clinical sign of several disorders: Case series reports and literature review. Medicine (Baltimore). 2018;97(36):e12124. 3. Alsuhaibani A, Burkat C, Plemel D. Blepharoptosis. Eyewiki. eyewiki.aao.org/Blepharoptosis. January 21, 2020. Accessed May 11, 2020. 4. Sudhakar, Q. Vu, O. Kosoko-Lasaki, M. Palmer. Upper eyelid ptosis revisited. Am J Clin Med. 2009;6(3):5-14. 5. Koka K, Patel B. Ptosis correction. www.ncbi.nlm.nih.gov/books/NBK539828/. StatPearls [Internet]. April 3, 2019. Accessed May 11, 2020. 6. Latting MW, Huggins AB, Marx DP, Giacometti JN. Clinical evaluation of blepharoptosis: distinguishing age-related ptosis from masquerade conditions. Semin Plast Surg. 2017;31(1):5-16. 7. Lim J, Hou J, Singa R, et al. Relative incidence of blepharoptosis subtypes in an oculoplastics practice at a tertiary care center. Orbit. 2013;32(4):231-4. |

