 |
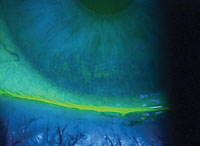
| An incomplete blink in a patient with dry eye. |
Efficacy outcomes, assessed at baseline and at four, 12 and 24 weeks, included an Ocular Surface Disease Index (OSDI) questionnaire, Schirmer’s test, tear break-up time, fluorescein and lissamine green staining, and corneal topographic indexes. Conjunctival impression cytologies were obtained and immuno-stained for inflammatory biomarkers. The results showed that the supplement treatment group had significantly improved dry eye symptoms. There was no progression of ocular surface inflammation, while inflammation worsened in the placebo group. Corneal irregularity, as measured by topographical indexes, was also maintained with supplement use, while surface irregularity progressed in the placebo group.
Understanding GLA
GLA is an omega-6 fatty acid (FA) found mostly in plant-based oils, such as borage seed oil, evening primrose oil and black currant seed oil. Omega-6 and omega-3 FAs are considered essential fatty acids (EFAs), which means they’re necessary for human health; however, our bodies don’t manufacture either of these fatty acids, so they must be ingested. A healthy diet contains a balance of omega-3 and omega-6 FAs.
Omega-3 fatty acids help reduce inflammation, whereas some omega-6 FAs promote it. Unfortunately, the typical American diet tends to favor the pro-inflammatory omega-6 variety, which is often found in animal fats and vegetable oils.
Notably, not all omega-6 fatty acids behave the same. Linoleic acid (LA) and arachidonic acid (AA) are typically considered less healthy because they promote inflammation. GLA, on the other hand, can reduce it, because much of the supplemental GLA is converted to an anti-inflammatory substance called dihomo-y-linolenic acid (DGLA).2 But to help promote the conversion of GLA to DGLA, the body must be nourished with certain nutrients, including magnesium, zinc, and vitamins C, B3 and B6.3
Fish Oil is Essential
Most ingested omega-6 fatty acids come from vegetable oils in the form of LA. The body converts LA to GLA and then to AA in a pro-inflammatory pathway. Without the presence of omega-3 fatty acids (ideally, from antioxidant-rich foods such as cold water fish or flaxseed), you can actually promote inflammation. You can achieve effective anti-inflammatory properties by maintaining a ratio of at least 1:1.
Clinical Research Concerning GLA + EPA/DHA
The clinical research related to ocular disease treatment and these EFAs is surprisingly abundant.
In 2011, researchers compared this combination to placebo and found statistical improvement in dry eye disease.4 Another study looked at the effects of a supplement involving LA, GLA and artificial tears on inflammatory markers in addition to typical dry eye testing. Interestingly, the results revealed statistically significant changes in symptoms (p<0.005), lissamine green staining (p<0.005) and ocular surface inflammation (p<0.05) in the study group, compared with controls as measured by human leucocyte antigen-DR (HLA-DR) expression reduction. There was no statistical improvement in TBUT or Schirmer’s testing.5
Research has also supported the benefits of GLA in the management of dry eye associated with contact lens use. In this study, the treatment group showed significant improvement in the specific symptom of “dryness” at three and six months (p<0.01) and also a significant improvement in overall lens comfort at six months (p<0.01). Tear meniscus height was increased in the treatment group at six months relative to baseline (p<0.01), although all other objective signs were unchanged.6
Patients with more advanced dry eye disease, such as Sjögren’s syndrome KCS, also seemed to benefit. GLA supplementation was shown to improve symptoms and corneal staining signs.7 More specific studies into post-refractive surgery (PRK) dry eye also showed statistical improvement in symptoms and signs, such as tear production clearance.8
Another study—once again, supporting the combination of GLA with EPA/DHA Omega-3 fatty acids—showed a statistical improvement in conjunctival inflammatory markers in dry eye patients after three months of use. The measurement for inflammation improvement was the reduction in conjunctival epithelium expression of the inflammatory marker HLA-DR. This study demonstrated that supplementation with omega-3 and omega-6 fatty acids can reduce expression of HLA-DR conjunctival inflammatory markers and may help improve DES symptoms.
Finally, there is also research supporting the benefits of GLA in meibomian gland dysfunction. In this study, patients were divided into three groups; the first received supplement containing GLA, the second lid hygiene and the third received both. Statistically significant improvement in symptoms occurred in all groups. After 180-day therapy, group one showed significant reduction in secretion turbidity (p=0.02) and meibomian gland obstruction (p=0.0001), whereas group two had significant reduction in eyelid edema (p=0.02), corneal staining (p=0.01), secretion turbidity (p=0.01) and meibomian gland obstruction (p=0.0001). Group three had significant reduction in eyelid edema (p=0.003), foam collection in the tear meniscus (p=0.02), corneal staining (p=0.02), secretion turbidity (p=0.0001) and meibomian gland obstruction (p=0.0001).
The importance of maintaining significant levels of omega-3 essential fatty acids in the body cannot be emphasized enough. The clinical benefit of GLA is well-supported as a proper supplement to promote DGLA formation and anti-inflammatory effects. GLA may well be a valuable component to ocular surface disease health, perhaps similar to what we’ve seen in macular disease research related to lutein, xeaxanthin and mesoxeaxanthin carotenoids.
Disclosures: Paul M. Karpecki has received compensation in the form of research grants, consulting fees, advisory board participation or speaker honoraria from the following companies: Akorn, Alcon, Allergan, AMO, Bausch + Lomb, MacuHealth, OcuSoft, PRN, Science Based Health and ZeaVision.
1. Sheppard JD Jr, Singh R, McClellan AJ, et al. Long-term supplementation with n-6 and n-3 PUFAs improves moderate-to-severe keratoconjunctivitis sicca: A randomized double-blind clinical trial. Cornea 2013;32:1297-1304.
2. Pacht ER, DeMichele SJ, Nelson JL, et al. Enteral nutrition with eicosapentaenoic acid, gamma-linolenic acid, and antioxidants reduces alveolar inflammatory mediators and protein influx in patients with acute respiratory distress syndrome. Crit Care Med. 2003 Feb;31(2):491-500.
3. Horrobin DF. Loss of delta-6-desaturase activity as a key factor in aging. Med Hypotheses. 1981 Sep;7(9):1211-20.
4. Creuzot-Garcher C, Baudouin C, Labetoulle M, et al. Efficacy assessment of Nutrilarm, a per os omega-3 and omega-6 polyunsaturated essential fatty acid dietary formulation versus placebo in patients with bilateral treated moderate dry eye syndrome. J Fr Ophtalmol. 2011;34:448-455.
5. Barabino S, Rolando M, Camicione P, et al. Systemic linoleic and gamma-linolenic acid therapy in dry eye syndrome with an inflammatory component. Cornea 22:97-102, 2003.
6. Kokke KH, Morris JA, Lawrenson JG. Oral omega-6 essential fatty acid treatment in contact lens associated dry eye. Contact Lens & Anterior Eye 31:141-6, 2008.
7. Aragona P, Bucolo C, Spinella R, et al. Systemic omega-6 essential fatty acid treatment and PGE1 tear content in Sjögren’s syndrome patients. Investigative Ophthalmology and Visual Science 46:4474-9, 2005.
8. Macri A, Giuffrida S, Amico V, et al. The effect of LA and GLA on tear production, tear clearance and on the ocular surface after PRK surgery. Graefes Arch Clin Exp Ophthalmol. 241:561-6, 2003.
9. Brignole-Baudouin F, Baudouin C, Aragona P, et al. A multicentre, double-masked, randomized, controlled trial assessing the effect of oral supplementation of omega-3 and omega-6 fatty acids on a conjunctival inflammatory marker in dry eye patients. Acta Ophthalmologica 89:e591-7, 2007.
10. Pinna A, Piccinini P, Carta F. Effect of oral linoleic and gamma-linolenic acid on meibomian gland dysfunction. Cornea 26:260-4, 2007.

