 |
|
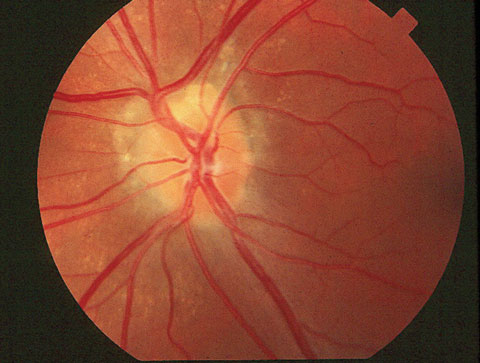
IOP reduction may be an effective way to treat progressive optic neuropathy and ocular hypertension. Photo: Joseph W. Sowka, OD. Click image to enlarge. |
A recent study looked at reducing intraocular pressure (IOP) as a potential therapy for patients with optic disc drusen (ODD), which are present in cases of glaucomatous optic neuropathy (GON).
This study retrospectively reviewed six patients with a history of both ocular hypertension and ODD. Progression of optic neuropathy was assessed through retinal nerve fiber thickness layer and visual field.
The researchers found that four out of six patients displayed progression of the condition in both eyes. The four that did were given IOP-lowering medications, and two of those four also had trabeculectomy surgery. Of the two who displayed no progression in either eye, one was given the same IOP-lowering medications, while the other was monitored off treatment.
Of the four patients who displayed progression, it was observed after the final IOP-lowering treatment that no further progression advanced. The researchers, based on this finding, believe that in the presence of both ocular hypertension and ODD, patients may benefit from treatment of ocular hypertension as a form of therapy, preventing further risk of progressive visual field or peripapillary retinal nerve fiber layer loss.
There is not much research on the coexistence of these conditions, but one study including 13 patients has concluded VF loss was more likely for those who display both ocular hypertension and ODD.
Researchers highlight that ODD and GON may share pathophysiological mechanisms, making IOP-related stresses a contributing factor in the progression of ODD. Furthermore, it is suspected that ODD result from impaired axonal transport and retinal ganglion cell metabolism. GON similarly displays increased mechanical stress, making retinal ganglion cells susceptible to damage, and impaired axonal transport at a given IOP. The researchers suggest impaired axonal transport and mechanical stress may be another mechanism shared by the two conditions, making pressure-dependent loss of retinal ganglion cells a result of shared mechanisms. Accordingly, both conditions may respond to the same IOP-lowering treatment.
Researchers caution that while ocular hypertension does present a substantial risk factor in developing GON, there is a portion of those with ocular hypertension who will never develop GON. As such, this study may have observed a similar phenomenon, with some patients displaying resistance to optic disc changes associated with ODD and GON, with IOP reduction having no discernible effect.
“Because IOP seems to be a risk factor, particularly in patients with ocular hypertension, it needs to be determined whether a potential shared mechanism between ODD and GON exists or whether a predominantly GON process is occurring and the definitive diagnosis is masked by the appearance of the optic disc”, researchers conclude. Despite this lack of understanding, treatment by IOP reduction may prove a reasonable therapy for patients with progressive optic neuropathy and ocular hypertension. When considering treatment, the researchers maintain that “although determining the origin of optic neuropathy in patients with ocular hypertension with ODD can be a challenge, we believe having a low threshold for initiating IOP-lowering treatment is warranted at this time.”
Kohli D, Chen JJ, Bhatti TM, et al. Optic disc drusen in patients with ocular hypertension: A case series and review of the literature. Journal of Neuro-Ophthalmology. 2022;00:1-6. |

