 |
A 71- year-old Hispanic male presented and reported decreased vision in his right eye for the past two months. He said he has difficulty reading fine print and seeing the TV.
His ocular history is significant for a traumatic injury to his left eye at a young age, which left him blind in this eye. He also underwent cataract surgery about seven years earlier in his right eye. His medical history is significant for hypertension, for which he takes lisinopril.
On examination, his visual acuity measured 20/100 in the right eye and was correctable to 20/50 on refraction. He had no light perception in his left eye. Confrontation visual fields were full to careful finger counting in the right eye.
 |
 |
|
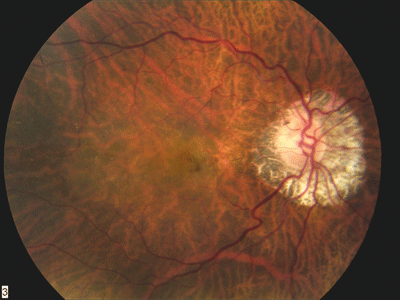
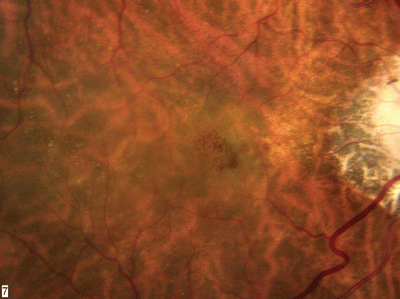
1, 2. The fundus photo of the right eye shows peripapillary atrophy and suspicious changes in the macula. |
 |
 |
|
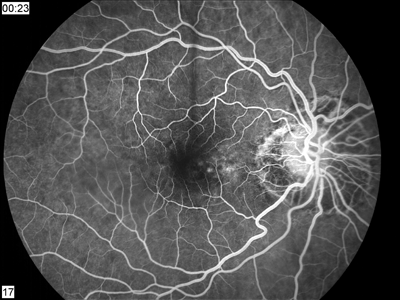
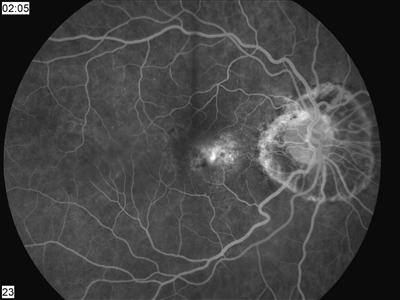
3, 4. The fluorescein angiogram shows an area of early hyperfluorescence that built in intensity with active leakage in the later frames. |
 |
|
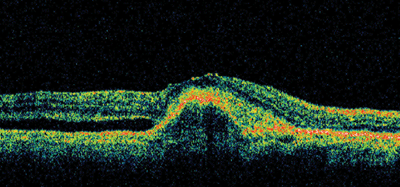
5. OCT of an oblique slice of the retina shows an obvious pigment epithelial detachment with an overlying neurosensory detachment inferiorly. |
1. Based on the fundus photos, which statement is likely true?
a. The patient has histoplasmosis.
b. The patient was highly myopic before cataract surgery.
c. The patient had a previous episode of malignant hypertension.
d. The patient had active toxoplasmosis at a young age.
2. What significant changes are seen in the macula?
a. Drusen.
b. Tear of the retinal pigment epithelium.
c. Subretinal hemorrhage.
d. All of the above.
3. What is the best interpretation of the fluorescein angiogram?
a. Serous detachment consistent with central serous retinopathy.
b. Retinal pigment epithelial detachment (PED).
c. Classic choroidal neovascular membrane.
d. Occult choroidal neovascularization (CNV) with some classic component.
4. What is the interpretation of the OCT?
a. PED with overlying neurosensory detachment.
b. Stage I macular hole.
c. Choroidal mass.
d. CNV.
5. What is the most likely diagnosis for this patient?
a. Occult CNV with some classic component.
b. Classic CNV.
c. Idiopathic central serous chorioretinopathy (ICSC).
d. Stage I macular hole.
6. How should this patient be treated?
a. Vitrectomy, membrane peel and injection of gas.
b. Photodynamic therapy (PDT) with Kenalog injection.
c. Macugen.
d. Intravitreal Avastin.
For answers, see bottom of page.
Discussion
The changes seen in the macula represent subretinal hemorrhage, most likely from a choroidal neovascular membrane. The fluorescein angiogram shows an area of early hyperfluorescence that builds in intensity with active leakage in the later frames; this is consistent with CNV. The complete boundaries of the membrane are not clearly defined, so this represents an occult CNV with some classic component to the membrane.
OCT also provides useful diagnostic information. On an oblique slice of the retina, we see an obvious PED with an overlying neursensory detachment inferiorly. The denser, higher reflective area on the superior side above the PED probably represents the CNV.
Given the peripapillary atrophy and appearance of the posterior pole, our patient probably was highly myopic before he underwent cataract surgery. When questioned, he admitted that he was very nearsighted as a child and that after cataract surgery, he no longer needed to wear thick glasses.
Could the high amount of myopia have anything to do with his present condition? There is no easy answer to this question. CNV associated with age-related macular degeneration (AMD) is more common in our patients age group, but there are no drusen anywhere in his retina. So, its unlikely that his condition is due to AMD. We might then assume that it is due to myopic degeneration, but CNV associated with myopic degeneration tends to be smaller than what we see here.
We dont really know the origin of this patients CNV. The important question, however, is how to treat it. Photodynamic therapy (PDT) is a reasonable option, but the results have not been promising for occult CNV.1
Anti-VEGF (vascular endothelial growth factor) therapies currently offer the best hope for treating these patients. Macugen (pegaptanib sodium, Pfizer) is the only anti-VEGF therapy that has been FDA approved for treating all types of CNV. Studies have shown it to be more successful than PDT, but patients still seem to lose vision over time.2
Lucentis (ranibizumab, Genentech), a future anti-VEGF treatment, has generated much excitement (though it is not currently FDA approved). In early clinical trials, visual acuity improved in patients treated with Lucentis but deteriorated in patients in the control group, the company says.
Avastin (bevacizumab, Genentech) was the first anti-VEGF drug to be FDA approved for the treatment of metastatic colorectal cancer. Because Lucentis is derived from Avastin and has shown great promise in early clinical trials, investigators have begun studying the off-label use of Avastin for treating CNV via intravenous and intravitreal injections.3
The results so far have been very encouraging. For example, in one study of 81 eyes (79 patients), mean visual acuity improved from 20/200 to 20/125 four weeks after injection and to 20/80 at eight weeks3
Because our patient has only one seeing eye, we elected to treat him with intravitreal Avastin. We believed that this agent offered the best chance of effectively treating the CNV and restoring the patients vision.
One month later, our patients uncorrected visual acuity improved to 20/30, the subretinal hemorrhage was resolved, and the PED was flattened. Our patient received a second injection and instructions to return in one month.
1. Photodynamic therapy of subfoveal choroidal neovascularization in age-related macular degeneration with verteporfin: one-year results of 2 randomized clinical trialsTAP report. Treatment of age-related macular degeneration with photodynamic therapy (TAP) Study Group. Arch Ophthalmol 1999 Oct;117(10):1329-45.
2. Gragoudas ES, Adamis AP, Cunningham ET Jr, et al. Pegaptanib for neovascular age-related macular degeneration. N Engl J Med 2004 Dec 30;351(27):2805-16.
3. Avery RL, Pieramici DJ, Rabena MD, et al. Intravitreal bevacizumab (Avastin) for neovascular age-related macular degeneration. Ophthalmology 2006 Mar;113(3):363-72.
Answers: 1)b; 2)c; 3)d; 4)a; 5)a; 6)d.

