 |
Q: 68-year-old Asian female came in for a cataract evaluation, but her angles were so narrow by gonioscopy that I was afraid to dilate her. Do I send her out for a laser peripheral iridotomy first, and then dilate her to assess the cataract?
A: “Ideal care involves a dilated peripheral exam before cataract surgery,” says David Friedman, MD, PhD, professor of ophthalmology at the Wilmer Eye Institute and director of the Dana Center for Preventive Ophthalmology at Johns Hopkins University School of Medicine. But, this patient’s case is not an ideal situation. “It’s a difficult problem and one that requires some judgment. And you’ll get a lot of different responses from different doctors,” Dr. Friedman says.
In his opinion, “I think the risk of an acute attack is very low, even if the angles are closed.”
The question boils down to whether the patient appears ripe for cataract surgery.
• Cataract surgery is likely. “If you think this is a visually-significant cataract and surgery is imminent, it’s reasonable to refer to your cataract surgeon. Be sure to get a look at the nerve and macula through an undilated pupil before you refer, to alleviate any fundus concerns,” Dr. Friedman says.
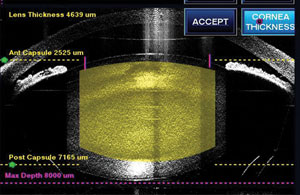 | |
| When dilating a cataract patient with narrow angles, such as this one, the risk of acute angle-closure attack is very low. |
The surgeon will dilate the eye at the time of surgery and take out the cataract. “The likelihood that the patient will have an acute angle-closure attack when dilated at the time of surgery is really low,” he says. “I even know some surgeons who will use dilation as a provocative test to see if an iridotomy is needed. I don’t personally do that but, because this is an area with limited evidence to support what we do, it’s a fairly reasonable approach.”
Furthermore, “once the cataract is out, there’s pretty much no risk of an acute attack. It would be incredibly unlikely,” Dr. Friedman says. Cataract surgery is essentially the cure for angle closure. “Taking out the lens will open the angle permanently in virtually anyone,” he says.
• Cataract surgery is not likely. “If the patient doesn’t have a visually significant cataract, and therefore surgery is unlikely in the near future, then I would refer the patient for an iridotomy and monitor for cataract over time,” Dr. Friedman says. “When you do an iridotomy, the angle opens up in about three-quarters of people. So it definitely does alter angle configuration in the majority of patients in whom it’s done.”
Again, this is the case in which the patient does not have visual symptoms. “I wouldn’t insist that the lens should come out just because there’s angle closure or residual angle closure after an iridotomy,” Dr. Friedman says. “I think that’s going a little too far, because there certainly are risks with cataract surgery—low risks, but risks all the same.”
Q: Does the consideration that the patient is Asian factor into the decision of whether to dilate?
A: No, says Dr. Friedman, who has researched the epidemiology of angle-closure glaucoma in Asian populations.
“While Asians may have a slightly higher rate of angle closure and angle-closure glaucoma, I still think the risk of acute attack with dilation is very, very small,” he says. Make gonioscopy part of your routine on all patients with shallow chambers, Asian or otherwise, and document your results clearly and carefully.
