 A 29-year-old female presented complaining of a large, painless lump in her left upper eyelid that developed rapidly over several days and has been present for the past three weeks. Though painless now, she experienced moderate pain while the lesion developed. This growth occurred several times previously, though not to this extent, and it resolved quickly without any intervention, she said. This time, she purchased an over-the-counter product and used it as directed on the box without any relief.
A 29-year-old female presented complaining of a large, painless lump in her left upper eyelid that developed rapidly over several days and has been present for the past three weeks. Though painless now, she experienced moderate pain while the lesion developed. This growth occurred several times previously, though not to this extent, and it resolved quickly without any intervention, she said. This time, she purchased an over-the-counter product and used it as directed on the box without any relief.
Best-corrected visual acuity was 20/15 O.U. The remainder of her examination was normal, except for biomicroscopically visible crusting around the eyelashes, blocked meibomian glands and a grossly visible hard focal lump in her left upper eyelid. Based upon appearance and history, she developed a chalazion secondary to chronic blepharitis.
There are several treatment options available for this patient, and virtually every doctor has a preferred approach to managing chalazia. In this months column, we examine the science behind each approach.
 Background
Background
Chalazion is a common inflammatory condition of the eyelid. There are two patterns of granulomatous inflammation representing the spectrum of changes in the clinical course of this condition. There may be mixed-cell granulomas consisting of neutrophils, lymphocytes, plasma cells, macrophages, giant cells and granulation tissue. Additionally, there may be suppurating granulomas characterized by epithelioid cell granulomas with numerous neutrophils in a proteinaceous background. The cells involved in these lesions are steroid sensitive.1,2
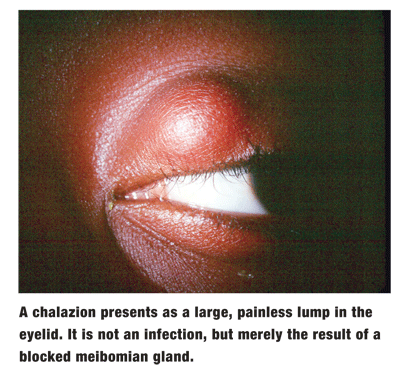
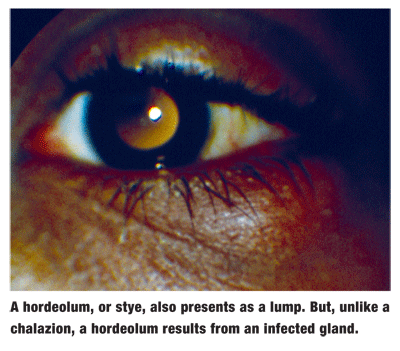 A chalazion is typically caused by blockage of the meibomian glands and chronic lipogranulomatous inflammation. It can affect patients of any age, race and gender. Common complaints are poor cosmesis, local irritation and, in cases of large lesions, mechanical ptosis and corneal astigmatism.3 In contrast to a hordeolum (commonly referred to by patients as a stye), which is painful and represents an infected gland, a chalazion is not the result of an infection.
A chalazion is typically caused by blockage of the meibomian glands and chronic lipogranulomatous inflammation. It can affect patients of any age, race and gender. Common complaints are poor cosmesis, local irritation and, in cases of large lesions, mechanical ptosis and corneal astigmatism.3 In contrast to a hordeolum (commonly referred to by patients as a stye), which is painful and represents an infected gland, a chalazion is not the result of an infection.
Therapeutic Options
The most common approach to the management of chalazia involves conservative therapy. The treatment modalities may include lid scrubs (using baby shampoo or commercially prepared scrubs), hot compresses with or without digital massage, topical antibiotic solutions and ointments, combination antibiotic/steroid solutions and ointments, and oral antibiotics.4-6
The effectiveness of conservative therapy is debatable, however. In a small series involving 37 patients, simple lid hygiene resulted in clinical chalazia cure in 80% of cases.6 But, a smaller case series involving six patients with seven chalazia managed with hot compresses and lid hygiene found only a 43% cure rate.5 In yet another small series involving 12 patients receiving hot compresses, lid hygiene and antibiotic ointment q.i.d., there was a cure rate of 58%.4
So, while conservative therapy does have success, it clearly does not work for every patient. Furthermore, there appears to be no standard as to what constitutes conservative therapy. But, it is non-invasive and exceedingly safe.
Because the inflammatory cells comprising chalazia are sensitive to steroids, intralesional steroid injection has been long considered a management option.2-10 It involves the injection of 0.1ml to 0.3ml of triamcinolone acetonide (5mg/ml to 40mg/ml) through the conjunctiva.3,4,7 Like conservative therapy, intralesional steroid injection lacks set guidelines with respect to the optimal amount and concentration of steroid to be used.
The success rates of this management modality, however, typically have been found higher than those of conservative therapy. One study saw a 94% cure rate following intralesional injection of triamcinolone; conservative therapy only demonstrated a 58% cure rate.4 A separate study achieved an 80% success rate after two injections.8 Intralesional injection in another study had a success rate of 90%, though two injections were often necessary.10 Yet another study had a cure rate of 90% with steroid injection combined with conservative therapy vs. a 43% cure rate using conservative therapy only.5
While intralesional injection of triamcinolone is generally considered a safe procedure, significant complications can occur. Skin depigmentation is a common occurrence following intralesional injection in dark-skinned patients.4,8,10 Also, accidental globe perforation is a possibility, and micro embolization by steroid particles can potentially result in retinal and choroidal infarction with subsequent permanent vision loss.11
Finally, surgical incision and curettage remain an option. The lesion is surgically removed, typically through a palpebral conjunctival approach, with the use of scalpel and chalazion clamp following injection of anesthetic. The surgeon may cauterize the wound immediately following excision, but again, it is a matter of preference, and it does not appear to reduce rates of recurrence.12
Cure rates following surgical excision are between 90% and 100%, though more than one surgery may be necessary.7,8 Surgical excision is the recommended procedure for lesions that are large (more than 11mm in diameter) and chronic (more than eight months in duration).2
But, while highly successful, surgical excision also has potential complications. The procedure is longer and more expensive than intralesional steroid injection. If the excision goes through the dermis, scarring is possible. And, inadvertent globe perforation may occur during chalazion excision.13 Still, surgical excision remains an option if conservative therapy or intralesional injection fail.
In the case presented here, conservative therapy seemed the best course of action since the patient had very dark skin, making her prone to depigmentation with steroid injection. Also, she was afraid of surgery. So, we directed her to apply lid scrubs and an antibiotic steroid ointment to her lid margins twice daily to combat her blepharitis and very hot compresses four times daily combined with vigorous digital massage to reduce the chalazion.
After two weeks of sporadic compliance, she returned with the chalazion greatly reduced (but still present). However, the lesion bothered her much less, and she elected no further treatment.
Drs. Sowka and Kabat are full-time faculty members at Nova Southeastern University College of Optometry.
1. Dhaliwal U, Arora VK, Singh N, et al. Cytopathology of chalazia. Diagn Cytopathol 2004 Aug;31(2):118-22.
2. Dhaliwal U, Bhatia A. A rationale for therapeutic decision-making in chalazia. Orbit 2005 Dec;24(4):227-30.
3. Ben Simon GJ, Huang L, Nakra T, et al. Intralesional triamcinolone acetonide injection for primary and recurrent chalazia: is it really effective? Ophthalmology 2005 May;112(5):913-7.
4. Chung CF, Lai JS, Li PS. Subcutaneous extralesional triamcinolone acetonide injection versus conservative management in the treatment of chalazion.
5. Garrett GW, Gillespie ME, Mannix BC. Adrenocorticosteroid injection vs. conservative therapy in the treatment of chalazia. Ann Ophthalmol 1988 May;20(5):196-8.
6. Perry HD, Serniuk RA. Conservative treatment of chalazia. Ophthalmology 1980 Mar;87(3):218-21.
7. Mustafa TA, Oriafage IH. Three methods of treatment of chalazia in children. Saudi Med J 2001 Nov;22(11):968-72.
8. Ahmad S, Baig MA, Khan MA, et al. Intralesional corticosteroid injection vs surgical treatment of chalazia in pigmented patients. J Coll Physicians Surg Pak 2006 Jan;16(1):42-4.
9. Kaimbo WA, Kaimbo D, Nkidiaka MC. Intralesional corticosteroid injection in the treatment of chalazion. J Fr Ophtalmol 2004 Feb;27(2):149-53.
10. Ho SY, Lai JS. Subcutaneous steroid injection as treatment for chalazion: prospective case series.
11. Thomas EL, Laborde RP. Retinal and choroidal vascular occlusion following intralesional corticosteroid injection of a chalazion. Ophthalmology 1986 Mar;93(3):405-7.
12. Sendrowski DP, Maher JF. Thermal cautery after chalazion surgery and its effect on recurrence rates. Optom Vis Sci 2000 Nov;77(11):605-7.
13. Shiramizu KM, Kreiger AE, McCannel CA. Severe visual loss caused by ocular perforation during chalazion removal. Am J Ophthalmol 2004 Jan;137(1):204-5.

