The word presbyopia comes from Greek roots meaning “old eye.” Past, current and—especially—future treatments for presbyopia aim to make that old eye young again.
Here’s a review of new corrective methods for presbyopia.
A New Look at Old Eyes
Ten years ago, the hot topic of presbyopia correction was scleral expansion bands. Scleral expansion bands have since fallen by the wayside, but new and revised methods of presbyopic correction have surfaced with the aim to help presbyopes toss away their readers.1
You’ve probably read all about currently-approved treatments for presbyopia, such as multifocal and accommodating IOLs, conductive keratoplasty and monovision LASIK.
So let’s look to the future. Right now, investigators are working on new accommodative IOLs, intracorneal implants, laser-induced multifocal corneal surgery, restoring flexibility to the crystalline lens, and maybe even a topical medicine.
Accommodative IOL

The Synchrony IOL accommodates by means of two separate optics.
• Synchrony IOL. Though not yet approved in the United States, the Synchrony Dual Optic Accommodating IOL (Abbott Medical Optics) is a single-piece, foldable, accommodating lens with two separate optics that are connected by a spring system. It’s designed to mimic the accommodating ability of the natural lens.
Two-year follow-up data in patients who had bilateral implantation found that both distance vision and reading speed actually increased at two years compared to one year post-op.
Specifically, best-corrected distance vision was 20/28 at one year and 20/23 at two years post-operatively.2 Reading speed was statistically significantly improved at two years, as was mean reading acuity (0.07 logMAR vs. 0.15 logMAR) and critical print size (0.28 logMAR vs. 0.48 logMAR).
Intracorneal Implants
• Flexivue Microlens.
The Flexivue Microlens (Presbia Coöperatief U.A.) is an intracorneal bifocal lens implant that is 3mm in diameter, less than 20μm thick, and made of a hydrophilic polymer. It is implanted in the nondominant eye, inserted into a pocket within the stroma created by a femtosecond laser. The central zone of the lens has no refractive power, while the periphery has a positive add for near vision. It is designed to correct between 2.50D and 3.50D of presbyopia, but can be removed if the patient’s prescription changes.
Investigators reported one-year results at the American Academy of Ophthalmology’s annual meeting in October.3 In 15 eyes, mean baseline near-vision acuity was 20/50. By the third month post-op—and for the remainder of the full year of follow-up—it improved to 20/25. In the implanted eye, mean uncorrected distance-vision acuity dropped from 20/20 at baseline to 20/40 during the first month, and then recovered to 20/30 at six months. All of the patients reported that their uncorrected near vision after the procedure was good or excellent, and 92% had stopped all use of reading glasses.
“Intracorneal lenses for the correction of presbyopia using a femtosecond laser seems to be a safe and effective method to correct presbyopia in patients aged between 45 to 55 years old—a target group that is considered too old for refractive laser surgery and too young for clear lens extraction,” investigators wrote.4

The tiny KAMRA inlay (pictured here next to a contact lens) creates a pin-hole effect to increase depth of field.
The Flexivue Microlens obtained the CE Mark in Europe, but is not approved in the U.S.
• KAMRA inlay. The KAMRA Corneal Inlay, formerly the AcuFocus Inlay (AcuFocus), is another implant approved in Europe that is currently being investigated in the U.S. The inlay is placed under a LASIK-type flap using a proprietary surgical device. It’s a donut-like 3.8mm implant with a 1.6mm central aperture that creates a pin-hole effect. The theory is that the small aperture setting increases the depth of field to bring objects both near and far into focus.
From results reported at three years post-op in 119 patients, the KAMRA inlay produced mean uncorrected distance vision of 20/20 and uncorrected near-vision of J1.5 A clinical trial of 504 patients is now under way in the U.S.
• Vue+ inlay. The Vue+ corneal implant, formerly called PresbyLens (ReVision Optics), recently completed Phase I of its FDA clinical trial. (It’s CE approved in Europe.) A multi-center study of the implant will evaluate 400 presbyopic subjects for a follow-up period of three years. All subjects are the target population for the implant: plano presbyopes between 45 and 65 years old.
Made of a proprietary hydrogel polymer, the Vue+ implant is 2mm in diameter, extremely thin and designed to fit beneath a corneal flap in the non-dominant eye. The implant is designed to steepen the central cornea. When the pupil constricts during an accommodative response, the inlay creates pseudo-accommodation to improve near and intermediate vision.
Results at six months post-op found that near vision improved to 20/25 or better in all the patients, with 86% percent seeing 20/20 or better, compared with a mean of 20/60 near vision at baseline. Mean uncorrected intermediate acuity was 20/25 at six months. There was a trade-off in distance vision, though, which decreased to 20/40 at worst. However, 72% of patients achieved 20/30 or better at distance.6
Multifocal Surgery
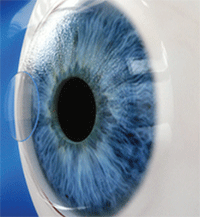
The Vue+ inlay steepens the central cornea for pseudo-accommodation.
• PresbyLASIK. This technique employs an excimer laser to create a multifocal ablation pattern on the cornea to correct the patient’s distance or near vision, depending on the approach.
In the center-distance approach (also called peripheral PresbyLASIK), the ablation pattern creates an aspheric cornea that is flatter in the center for good distance vision and steeper away from the center for good intermediate and near vision. Using this peripheral approach in 44 eyes (22 patients) with presbyopia and low to moderate hyperopia, investigators reported that the mean uncorrected distance vision was about 20/20 and the mean uncorrected near vision was about 20/25 at six months post-op.7
In the center-near approach (also called central PresbyLASIK), the ablation steepens the central cornea for good near vision and flattens the mid-peripheral cornea for clear intermediate and distance vision. Six-month post-op data from an early study found that 64% of patients achieved uncorrected distance vision of 20/20 or better and 72% of patients achieved uncorrected near vision of 20/40 or better. However, more than one-fourth of patients lost a maximum of two lines of best spectacle-corrected visual acuity.8
According to the reported results, both central and peripheral PresbyLASIK achieve adequate spectacle independence for both far and near. However, peripheral PresbyLASIK requires a neuroadaptation process, which may last as long as a year.9 Patient selection is also extremely important for either approach.
• IntraCor. The IntraCor procedure is similar to PresbyLASIK, but employs a femtosecond laser to remove tissue only in the stroma, leaving the corneal epithelium and Bowman’s membrane intact. Because no corneal incision is required, the IntraCor procedure maintains the structural integrity of the cornea, which promotes wound healing and greatly minimizes the risk of infection.
For this procedure, the femtosecond laser creates an intrastromal ablation, forming consecutive rings. These intrastromal ring cuts reshape the cornea and redistribute the biomechanical forces, which results in a change in corneal refraction.
Recent results of 25 patients (mean age of 56) showed improvement in near-vision acuity from about 20/100 at baseline to about 20/30 at two years post-op.10 Most patients had gained five to six lines of uncorrected near acuity on a standard chart relative to baseline, allowing them to read newspapers held at a normal distance without reading glasses. Intermediate vision was unchanged. However, the procedure does induce a degree of myopia for distance vision.

The IntraCor procedure employs a femto laser to reshape the stroma and improve near vision.
Softening the Lens
• Femtosecond lentotomy.
A corollary to the Helmholtz theory of accommodation is that presbyopia occurs due to the hardening of the lens. So, if the presbyopic lens could be softened or its flexibility improved, then accommodation would be restored.
This is the concept behind the use of femtosecond laser to make micro cuts inside the crystalline lens (lentotomy) to increase or even re-establish the flexibility of the lens, and eliminate presbyopia. (This assumes that the ciliary body and lens capsule stay functional in old age.)
A German laser company, Laser Zentrum Hannover, has developed a “steering wheel” cutting pattern to restore elasticity of the lens. Using a femtosecond laser, this pattern creates “gliding planes” in all directions, but leaves the lens capsule intact and the central field of view unaffected. So far, tests on enucleated pig eyes and human donor lenses have shown that femtosecond lentotomy did increase the flexibility of the crystalline lens.11
• Lens refilling. Replacement of the lens with an IOL is the standard treatment for cataract surgery. But, even an accommodating IOL is made of a harder material than the natural lens cortex. So, it only makes sense to replace the sclerotic lens with a malleable or even liquid material, such as a soft polymer, to restore accommodation. That’s the focus of several investigations. But a number of hurdles have to be overcome before this procedure can be called a success.
For example, in a study of nine rhesus monkeys whose lenses were refilled with silicone polymer, the maximum accommodative amplitude of the surgically treated eyes was only about 40% (6.30D).12 After 37 weeks of follow-up, the accommodative amplitude decreased to almost zero in three monkeys. Yet, in two other monkeys, the accommodative amplitude remained stable at about 4.00D during the follow-up period. (An accommodative amplitude of approximately 3.00D to 4.00D in presbyopic human eyes would be sufficient for reading purposes, the investigators wrote.) Additional hurdles to overcome include defining the exact type of polymer to be used, the correct amount to be used, and halting rapidly developing posterior capsule opacification.
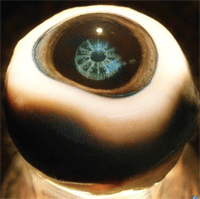
A femto laser cut this “steering wheel” pattern into the lens to restore flexibility.
Last but not least is a recent patent for a topical drop to prevent presbyopia. The drop would contain a chelating agent, such as picolinic acid, that would inhibit the growth of epithelial cells in the crystalline lens.13 (The lens grows throughout life.)
So, who knows? One day these surgical approaches may fall by the wayside, and you’ll stop presbyopia with a drop.
Thanks to Jerry Legerton, O.D., M.S., M.B.A., of San Diego, Calif., for his help with this article.
1. Mathews S. Scleral expansion surgery does not restore accommodation in human presbyopia. Ophthalmology. 1999 May;106(5):873-7.
2. Bohórquez V, Alarcon R. Long-term reading performance in patients with bilateral dual-optic accommodating intraocular lenses. J Cataract Refract Surg. 2010 Nov;36(11):1880-6.
3. Pallikaris IG. Intracorneal lenses for the treatment of presbyopia using femtosecond laser: visual outcomes and safety. Abstract PA101. Paper presented at the American Academy of Ophthalmology Annual Meeting; October 17, 2010; Chicago, Ill.

4. Pallikaris I, Limnopoulou A, Kymionis G, et al. Intracorneal lenses for the treatment of presbyopia using femtosecond laser: visual outcomes and safety. 2010 Sep. Acta Ophthalmologica. [Epub ahead of print]
5. Durrie D. Patient experience with Acufocus intracorneal inlay 3 years after surgery. Abstract PA102. Paper presented at the American Academy of Ophthalmology Annual Meeting; October 17, 2010; Chicago, Ill.
6. Lin DT, Holland SP, Barragan E, Mehin ME. Early experience with a presbyopic corneal inlay. Paper presented at American Society of Cataract and Refractive Surgery Symposium and Congress. April 3-8, 2009; San Francisco, Calif.
7. Pinelli R, Ortiz D, Simonetto A, et al. Correction of presbyopia in hyperopia with a center-distance, paracentral-near technique using the Technolas 217z platform. J Refract Surg. 2008 May;24(5):494-500.
8. Alió JL, Chaubard JJ, Caliz A, et al. Correction of presbyopia by technovision central multifocal LASIK (presbyLASIK). J Refract Surg. 2006 May;22(5):453-60.
9. Alió JL, Amparo F, Ortiz D, Moreno L. Corneal multifocality with excimer laser for presbyopia correction. Curr Opin Ophthalmol. 2009 Jul;20(4):264-71.
10. Holzer M. Two-year follow-up of IntraCOR femtosecond laser treatments. Abstract PA100. Paper presented at the American Academy of Ophthalmology Annual Meeting; October 17, 2010; Chicago, Ill.
11. Schumacher S, Oberheide U, Fromm M, et al. Femtosecond laser induced flexibility change of human donor lenses. Vision Res. 2009 Jul;49(14):1853-9.
12. Koopmans SA, Terwee T, Glasser A, et al. Accommodative lens refilling in rhesus monkeys. Invest Ophthalmol Vis Sci. 2006 Jul;47(7):2976-84.
13. Ravi N, Hamilton PD. Treatment of presbyopia with alpha-picolinic acid and its analogs. Available at:
www.freepatentsonline.com/20100113535.pdf (accessed December 8, 2010.)

