Starting July 1, optometrists can participate in a new physician quality reporting initiative that offers a 1.5% Medicare bonus payment for those health-care providers who report specific measures designed to improve patient care.
This new program, known as the Physician Quality Reporting Initiative (PQRI), is being administered by the Centers for Medicare and Medicaid Services (CMS). Participation is voluntary for Medicare providers, including O.D.s, says optometrist David Cockrell, AOA board of trustees liaison to the AOA Advocacy Group.
The initiative establishes a financial incentive for eligible physicians to participate in a voluntary quality-reporting program. The objectives: to help CMS assess the quality of care provided for key illnesses and clinical conditions that affect Medicare beneficiaries and to support clinicians in providing appropriate treatment of the conditions identified, according to CMS.
Eligible professionals who successfully report a designated set of quality measures on claims for dates of service from July 1 to December 31 may earn a bonus payment of the 1.5% of total allowed charges for covered Medicare physician fee schedule services.
There are 74 measureseight of which pertain to eye careincluded in the 2007 PQRI. These quality-control measures involve primary open-angle glaucoma, age-related macular degeneration, cataract and diabetic retinopathy. (See table.)
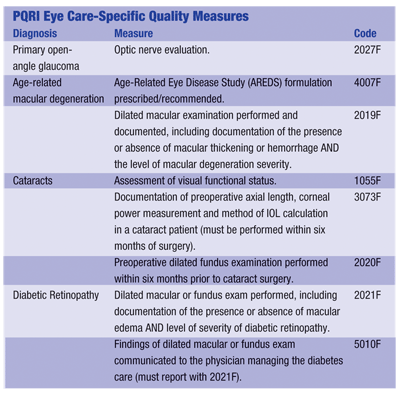
When a doctor diagnoses one of these conditions, he or she must fill in the procedure code on the Medicare form and write in a special code underneath the procedure code, Dr. Cockrell says.
Practitioners must report the designated services on claims using CPT Level II Codes, the performance measurement code set. These special codes tell the Medicare reviewer how the diagnosis was made.
The billing is still the same; an additional code is just added. It is very simple, Dr. Cockrell says.
Optometrists report the quality codes on the CMS 1500 form or the 837-P electronic formthe same claim forms for reporting the payment codes. Optometrists will need to modify their billing to add the listed CPTII codes on all claims or electronic billing systems. O.D.s do not need to use electronic medical records to participate. Quality reporting can be done using the current 1500 billing form and by amending the new category II codes.
To qualify for the 1.5% bonus, an optometrist must achieve 80% reporting on three measures for each patient who has the diagnosis relevant to the quality measure. If an optometrist reports on four or more measures, only three measures must achieve the 80% reporting standard.
The 1.5% bonus is based on the total allowed charges from July 1, 2007 through Dec. 31, 2007. The bonus payment will be made in a lump sum in mid-2008.
For more information, go the CMS Web site at www.cms.hhs.gov/PQRI, or the AOA Web site at www.aoa.org/X7506.xml.

