
Youve heard the good news. Advances in lens design and material chemistry can combine to offer superb contact lens options for our presbyopic patients. Skeptical? Have you been offered promising new multifocal contact lenses in the past, only to find them disappointing?
Sometimes under-performance is the fault of the product, while other times, it is how we use the product. But, how do we know the difference? Heres how to meet the needs of the presbyopic patient most effectivelyand efficientlywith todays multifocal contact lenses.
Monovision or Multifocal?
First, try not to declare allegiance to either the monovision or multifocal fitting philosophy, as this type of thinking imposes unnecessary limits on problem-solving strategies. Sometimes, the best solution, especially with the more advanced presbyope, is to combine the two approaches.
Who wouldnt agree that it is better to have clear vision at all distances in each eye than to have clear vision at far in one eye and near in the other eye? With that in mind, it is reasonable to begin the fitting process by employing multifocal lens designs.
Understand Limitations
You may think that multifocal contact lenses require some give and take and that spectacle multifocal lenses provide perfect vision. Actually, every form of presbyopic correction requires some adaptation. The difference is that we have become accustomed to coaching our progressive spectacle lens patients to lower your eyes, not your head, when you want to read; we dont see these required behavioral changes as limitations. So, our task now is to arrive at the same level of comfort when coaching patients through the adaptation process with multifocal contact lenses. The first step: Set appropriate expectations.
1: Realistic Expectations
How do we let patients know what they can expect from multifocal contact lenses without being either discouraging or overzealous? The trick to establishing realistic expectations is to provide information about both the good and the less desirable characteristics of the lenses without emphasizing one more than the other. I find the sandwich approach helpful in striking the right balance. Introduce a positive statement about the lenses, then present the patient with the meat, or the challenging information, about multifocal lenses. Then, close with another positive statement. For example:
Positive Statement #1: I know youve enjoyed the freedom contact lenses have offered you. Im pleased to inform you that we have lens designs that allow you to continue to enjoy those benefits and provide you with clearer near vision.
The Challenge: Every form of bifocal correction requires some give and take. For example, glasses require you to look through a particular portion of the lens to see clearly at a given distance. Similarly, bifocal contact lenses require some adjustment. For example, you may find that you need to wear reading glasses over your contact lenses when reading in dim light. Also, some patients who wear these lenses notice glare around headlights while driving at night and find it more comfortable to wear glasses instead while taking a long night drive.
Positive Statement #2: But, having said that, I believe I can meet most of your daily visual needs with these lenses. Would you like my technician to come in and further discuss this option with you?
Also, make sure to let your patients know that fitting multifocal lenses is a process. Sometimes, the first pair of lenses fits well, but it is not unusual to need small adjustments to maximize lens performance.

2: The Value of a Good Refraction
Perform the pre-fitting spectacle refraction with the intention of providing clear vision at distance with the least amount of minus and clear vision at near with the lowest add power. Your goal should be to minimize the difference between the distance and near prescriptions. The greater the disparity between distance and near powers in a multifocal contact lens, the greater the likelihood that they will interfere with each other.
3: The Role of Ocular Dominance
There are conflicting opinions regarding the importance of ocular dominance in achieving success with presbyopic contact lenses.1 The most common method used to assess ocular dominance is the extended arms technique (figure 1). This method identifies what is referred to as sighting dominance. However, numerous studies have cast doubt on the importance of sighting dominance to success with presbyopic contact lens correction; these studies have not demonstrated a strong correlation between ocular dominance and monovision success rates.2,3
Sometimes, sensory dominance may play a more significant role.4 This can be determined by assessing a patients response to blur introduced in front of each eye independently under binocular conditions. (See Methods of Assessing Sensory Dominance.)
I assess ocular dominance because it serves as another tool that may help achieve success. Additionally, lens selection with designs such as the Frequency 55 and Proclear Multifocal (CooperVision) require that you determine which is the dominant eye.

4: Choosing Diagnostic Lenses
Youve laid the groundwork. Now, its time to choose the first pair of diagnostic lenses. Where do you start?
Base your brand selection on what you know about its performance. This information is gleaned from various sources, but perhaps the best teacher is experience. When new lenses are introduced into the marketplace, familiarize yourself with their design and rationale, and then try them. Begin with a straightforward case. Choose a patient with desirable ocular characteristics and reasonable expectations. Strive to fit at least five to 10 patients with each design so that you begin to understand the nuances of each design. This will help you employ them more judiciously in the future.
Once you decide on a brand, choose your first pair of lenses based on the manufacturers fitting guide. The manufacturer wants you to be successful with its lens, after all, and these guides are designed to help you do just that. They are a valuable resource but are often underutilized. Once you get comfortable with the lenses and begin to recognize their strengths and weaknesses, then you can start improvising.
Once the lenses are applied, escort the patient to the reception area. Allow the lenses to settle for at least 10 minutes.
This settling time is important for the patient in two ways. First, visionparticularly near visionwith multifocal contact lenses improves significantly after a few minutes. If you assess the patients corrected vision prematurely, you will underestimate the lenses true performance.
Second, while the lenses are settling, the patient can explore his or her visual world by looking out the window, reading a magazine or just observing the goings-on of your reception area.
6: Hows It Going?
Once the lenses have settled, call the patient back to the exam room. When you enter the room, immediately ask the patient: How are you doing with the lenses? An open-ended question allows patients to direct your focus to the area that needs attention and not simply answer Yes or No. For example, if the patient reports that her near vision is fine, but her distance is blurred, you can get right to work on her distance vision complaint.

7: A Real World Environment
 When assessing patients vision performance with these lenses, do so under conditions that are similar to what they will experience on a day-to-day basis. This means having them read the acuity chart under binocular conditions with the room lights up. Most of us are binocular creatures. Assessment of vision with multifocal contact lenses under binocular conditions is not only more natural, but the lenses perform better.
When assessing patients vision performance with these lenses, do so under conditions that are similar to what they will experience on a day-to-day basis. This means having them read the acuity chart under binocular conditions with the room lights up. Most of us are binocular creatures. Assessment of vision with multifocal contact lenses under binocular conditions is not only more natural, but the lenses perform better.
Keep the room lights up to normalize pupil size, since it dictates what information enters the eye with the simultaneous vision designs that make up many of todays gas permeable (GP) multifocal lenses and virtually all soft multifocal contact lenses.
If the room lights wash out the contrast on the acuity chart, turn off the overhead light and bring your instrument stand light out in front of the patient. Place it to the side so that it lightly illuminates the patients face (figure 2).
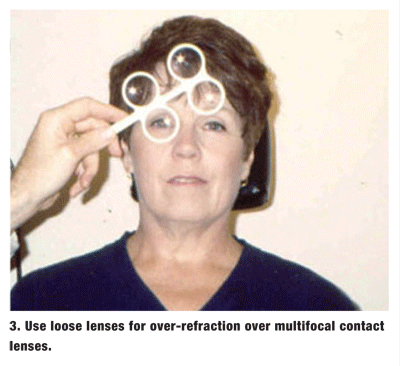 If the patient has a visual complaint, put the phoropter aside and perform an over-refraction utilizing loose lenses (figure 3). Or, if the patient has no complaints and can see well enough to drive safely, dont change anything immediately. Encourage the patient to wear the lenses regularly and return in a week for follow-up.
If the patient has a visual complaint, put the phoropter aside and perform an over-refraction utilizing loose lenses (figure 3). Or, if the patient has no complaints and can see well enough to drive safely, dont change anything immediately. Encourage the patient to wear the lenses regularly and return in a week for follow-up.
8: Time to Troubleshoot
If the patient returns with a visual complaint, dont lose heart. Remember, multifocal contact lens fitting is a process.
Begin by assessing binocular vision both at distance and near. To troubleshoot, proceed to monocular acuity assessment at distance and near. This way, you can identify an eye that may not be performing as expected at a given distance. Demonstrate changes over the contact lenses with loose lenses; a change of 0.25D can make a significant difference in visual performance.
In most cases, a change of no more than 0.50D, or occasionally 0.75D, should be expected. If your over-refraction indicates that a greater change is needed, the contact lens power is most likely wrong, or you probably need to change to a different lens design.
Solving distance vision complaints usually involves maximizing vision in the dominant eye. But first, assess monocular acuity to ensure that the non-dominant eye is providing the expected level of acuity at distance.
Then, look at the dominant eye. If the contact lens has a low add, modify the distance prescription. This usually means adding minus, but some hyperopes may need more plus in the distance Rx.
 If the contact lens has a high add, reducing it is usually the most effective method of improving distance vision. Remember, the lowest add is no add. A single-vision lens on the dominant eye is sometimes the solution, especially when dealing with low distance refractive errors.
If the contact lens has a high add, reducing it is usually the most effective method of improving distance vision. Remember, the lowest add is no add. A single-vision lens on the dominant eye is sometimes the solution, especially when dealing with low distance refractive errors.
If distance vision complaints persist, and the acuity of the non-dominant eye is less than 20/40 at distance, employ the above strategies with the non-dominant eye.
Solving near vision complaints, on the other hand, usually involves maximizing vision in the non-dominant eye. Confirm that the lens on the dominant eye is providing the expected level of acuity at near before proceeding.
Problem solving strategies at near are precisely the inverse of what is employed to resolve distance vision complaints. Increase plus in the distance prescription, or increase add power. These strategies can be employed with either eye, but generally begin with the non-dominant eye when troubleshooting near vision complaints.
Also, keep in mind that some lens designs provide additional problem-solving strategies. For example, if a patient fit with the Proclear Multifocal lens (CooperVision) wears a D lens on the dominant eye and an N lens on the non-dominant eye but complains of distance blur, this patient may perform better with a D lens on each eye.
Finding the Right Balance
The key to success with multifocal contact lenses is to find the right balance between distance and near vision. Any time a change is made to enhance the vision of one, the impact must be assessed at the other.
The proper balance may differ from patient to patient. A night duty security officer may be willing to give up a little near vision to achieve clear distance vision while on duty, while a librarian may be willing to give up a little distance vision in order to see comfortably through the work day.
Be supportive as you interact with the newly presbyopic contact lens patient. A little more hand-holding is often required as you work through the multifocal fitting process. Remember: It is a process. Remind the patient of this if you feel discouragement creeping in.
Patience, perseverance and a methodical problem-solving strategy will guide you to success with todays ever-improving multifocal contact lens designs.
Dr. Quinn is in group practice in
1. Quinn T. The role of ocular dominance in presbyopic contact lens correction. Contact Lens Spect 2007 Jan;134:48-9.
2. Shor C, Landsman L, Erickson P. Ocular dominance and the interocular suppression of blur in monovision. Am J Optom Physiol Opt 1987 Oct; 64(10):723-30.
3. Erickson P, McGill EC. Role of visual acuity, stereoacuity, and ocular dominance in monovison patient success. Optom Vis Sci 1992 Oct;69(10):761-4.
4. Robboy MW, Cox IG, Erickson P. Effects of sighting and sensory dominance on monovsion hight and low contrast visual acuity. CLAO J 1990 Oct-Dec; 16(4):299-301.

