
A 38-year-old Asian female presented complaining of a pulsating sensation and puffiness in her left eye for the past two days. There was no associated blurred vision, pain, discharge, nausea, vomiting or headaches.
She was previously diagnosed with recurrent Posner-Schlossman syndrome (PSS), and she reported frequent episodes of elevated intraocular pressure and inflammation in her left eye since 1994.
The patient had completed a self-administered course of treatment using Betoptic (betaxolol, Alcon) and Pred Forte (prednisolone acetate 1%, Allergan) for this condition about two weeks prior to this visit.
She also reported an awareness of elevated IOP in the left eye and assumed that the condition had recurred. (Because of her many episodes of PSS, she usually can estimate her IOP within 2mm Hg.)
She believed this latest flare-up was related to an episode of recent stress: a death in the family. She also reported a correlation between flare-ups and exacerbated environmental allergies; she believed this episode was no different. She had instilled one drop of Betoptic and three drops of Pred Forte in the left eye within the last day.
A review of her records indicated that the patient has been treated for recurrent episodes of PSS since 1994. Since then, she has experienced six episodes per year on average. The longest period of remission was one year, and the shortest was about one month.
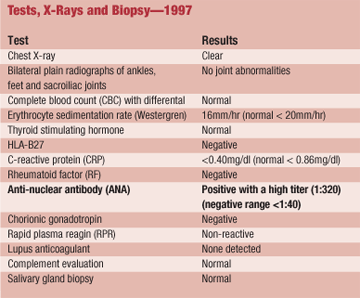
She had undergone a comprehensive blood work-up in 1997 (see Tests, X-Rays and Biopsy1997, below). All tests were negative or within normal limits, except for an elevated antinuclear antibody (ANA), 1:320.
She was subsequently referred to a rheumatologist to rule out an underlying systemic disease. The outcome of the rheumatology evaluation was inconclusive; however, her rheumatologist speculated that the elevated ANA could be related to a history of hyperthyroidism.
There was no history of injury, infection or surgery in the left eye.
Her medical history was positive for hyperthyroidism and hypercholesterolemia. Her primary-care physician opted not to treat the hyperthyroidism, since her last blood work-up showed normal thyroid function. The patient reported that she previously treated the condition with a Chinese medicine, which she believed helped resolve the condition. She also reported using Lipitor (atorvastatin calcium, Pfizer) q.d. for one month for her hypercholesterolemia, but subsequently self-discontinuing treatment. Lastly, the patient reported an adverse reaction (a psychotic episode) to Alphagan (brimonidine 0.2%, Allergan), which she had been prescribed previously. She also used Claritin OTC (loratadine, Schering-Plough) p.r.n. for frequent bouts of allergic rhinoconjunctivitis. Her family ocular and medical histories were non-contributory.
Diagnostic Data
Best-corrected distance acuity was 20/15-1 O.D. and 20/15 O.S. Pupils were equal in diameter in both light and dark illumination, with brisk direct and consensual pupillary responses. There was no relative afferent pupillary defect in either eye.
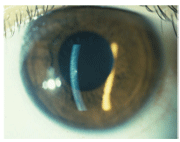
This patient presented with one fine keratic precipitate on the central corneal endothelium O.S. and two smaller ones at the 5 o"clock position.
Preliminary and gross external examinations were within normal limits. External biomicroscopy revealed open angles using the Van Herick technique. Two to three cells and minimal flare were visible in the anterior chamber of the left eye via high-magnification biomicroscopy.
One fine keratic precipitate (KP) was present on the central corneal endothelium in the left eye, and two smaller ones were noted at the 5 oclock position. There were no iris nodules or posterior synechiae. Biomicroscopy of the right eye was unremarkable.
IOP measured 16mm Hg O.D. and 27mm Hg O.S. by Goldmann tonometry. Gonioscopic evaluation at previous visits indicated bilateral open anterior chamber angles with normal angle pigmentation. Dilated fundus examination was unremarkable. Both optic nerves appeared pink, with cup-to-disc ratios of 0.40 x 0.40 O.D. and 0.55 x 0.50 O.S.
Diagnosis
I diagnosed PSS of the left eye.
Treatment and Follow-up
I initiated treatment in this eye with Pred Forte q.i.d. for four days, Betoptic b.i.d. and 200mg Aleve (naproxen, Bayer Health Care) p.o. b.i.d. Cycloplegia was unnecessary given the mild anterior chamber reaction. I instructed the patient to return after four days, at which time I would adjust the medical therapy as needed.
At the four-day follow-up visit, the patient believed that her IOP had normalized. Evaluation of the anterior chamber now revealed one cell per high-magnification field and a trace flare. The KPs observed at the first visit had decreased in density.
The patients IOP measured 14mm Hg O.D. and 16mm Hg O.S. I instructed her to taper the Pred Forte in the following manner: one drop t.i.d. for four days, one drop b.i.d. for four days, one drop q.d. for four days, and then one drop every other day for four days. I also instructed her to continue the Aleve p.o. b.i.d. and discontinue the Betoptic.
One week later, her IOP measured 13mm Hg O.D. and 12mm Hg O.S. There were no cells or flare in the left anterior chamber, and all the endothelial KPs had resolved.
I told the patient that she could resume her use of Restasis b.i.d. O.U. for her dry eyes. I also suggested that she schedule a consultation with an allergist to try to decrease the frequency of her allergic bouts.
We discussed possible preventive measures, such as low-dose steroids or nonsteroidal anti-inflammatory drugs (NSAIDs), but she is reluctant to take any medications. So, we stressed the importance of returning for an annual eye exam, or returning as needed if symptoms develop.
Discussion
In 1948, Adolph Posner, M.D., and Abraham Schlossman, M.D., first reported on their observations of a recurrent, unilateral anterior uveitis associated with a spike in IOP that lasted from a few hours to several weeks.1 This condition has since been referred to as Posner-Schlossman syndrome, or glaucomatocyclitic crisis.
PSS is diagnosed by the presentation of episodic, often unilateral spikes in IOP associated with low-grade non-granulomatous anterior uveitis.1-11
The period of remission is generally characterized by normal IOP, outflow facility, optic nerve appearance and visual fields.1-13 The latter two clinical features are not absolute hallmarks of PSS, though; patients experiencing recurrent PSS attacks for 10 years or more have 2.8 times greater risk of optic nerve damage.9
PSS is a self-limiting condition that lasts a few weeks to a month. During the acute and remission phases of PSS, anterior chamber angles are typically open with normal pigmentary density and no associated synechiae.2-5,8,10
The IOP spike associated with PSS is primarily due to a decrease in outflow facility, although some research demonstrates that increased aqueous formation may also be involved.12
When diagnosing PSS, you must rule out other conditions that could cause unilateral or bilateral uveitis. These include Fuchs heterochromic iridocyclitis, acute angle-closure glaucoma, pigmentary glaucoma, herpes simplex virus, trabeculitis (which has been suggested as a possible cause of PSS), neovascular glaucoma and secondary angle-closure glaucoma due to peripheral anterior synechiae.2-4,8,10
The exact etiology of PSS is still unknown. But, associations with allergies, cytomegalovirus, herpes simplex virus, an autonomic imbalance and stress-induced attacks have been reported.5,8,10,14-18 One study found elevated prostaglandin E levels in the aqueous humor of patients during the active phase of PSS and normal concentrations during the remission phases; these levels correlated positively with IOP.19 In another case, the patient reported a correlation between flare-ups and monthly stressas did the patient who presented here.10
Reports show that PSS accounts for about 4% of anterior uveitis cases.20 The condition is most prevalent between the second and fifth decades of life, and it is more common in males.8 A positive diagnosis is usually based on both history and clinical appearance.
No systemic associations have been linked with the condition, although recent reports suggest an association with the human leukocyte antigen (HLA) Bw54.2-5 Human leukocyte antigens are a genetically determined series of antigens present on human white blood cells (leukocytes) and tissues. There are three major genetically controlled groups: HLA-A, HLA-B and HLA-DR.
HLA-B surface antigens are encoded by more than 30 detectable alleles on locus B of the HLA complex, the most polymorphic of all the HLA specificities. They are involved in the cellular immune reactivity of cytolytic T lymphocytes. Several of these antigens (e.g., HLA-B27, -B7, -B8) are strongly associated with a predisposition to rheumatoid and other autoimmune disorders. So, any suspicion of underlying systemic disease warrants a blood work-up to rule out coexisting systemic conditions.
Treatment of PSS includes topical steroids to decrease the inflammation and ocular hypotensive agents, such as topical beta-blockers, topical alpha-agonists, topical or oral carbonic anhydrase inhibitors, and hyperosmotic agents.2-5,8,10,11
Cycloplegic agents are generally reserved for more severe symptomatic anterior chamber reactions.5 Prostaglandin analogues and pilocarpine are contraindicated, as these may exacerbate the inflammatory reaction.
Few studies have been done into the prophylactic management of PSS. Medical therapy using ocular hypotensive agents between attacks may be considered; however, since the prognosis is generally good without the drops, the risks such as hypotony between attacks and the side effects of the medications, have to be carefully weighed. Filtration surgery has been suggested as a method of prophylaxis; however, reports vary regarding its efficacy in reducing flare-ups.9,21 Some reports advocate the use of topical and/or systemic NSAIDs, but there is no evidence that such treatment prolongs remission periods.2-5,8,10
Careful monitoring of any change in the patients visual fields, retinal nerve fiber layer and optic nerve is essential, especially given the high risk of optic nerve damage associated with recurrent attacks and a possible association of PSS with primary open-angle glaucoma (although no well-controlled clinical studies have investigated this association).9,22
A unilateral (or, in rare instances, bilateral) episodic spike in IOP accompanied by a low-grade non-granulomatous uveitis that is out of proportion to the spike in IOP should alert you to a differential diagnosis of PSS. Make certain to exclude other conditions that mimic this condition.
The goal of treatment is to control the inflammation and reduce IOP. Frequent follow-up and proper patient education on signs, symptoms and recurrences are essential to manage the condition effectively and promptly.
Dr. Pate is an associate clinical professor at the University of Houston College of Optometry. Dr. Raghunandan is an assistant professor at Michigan College of Optometry.
1. Posner A, Schlossman A. Syndrome of unilateral recurrent attacks of glaucoma with cyclitic symptoms. Arch Ophthalmol 1948 Apr;39(4):517-35.
3. Kunimoto DY, Kanitkar KD, Makar MS, eds. The Wills Eye Manual: Office and Emergency Room Diagnosis and Treatment of Eye Diseases, 4th ed.
4.
5. Oakman JH. Posner-Schlossman Syndrome, June 2006. Available at: www.emedicine.com/ oph/topic137.htm. (Accessed 22 Oct 2004).
6. Shiuey Y. 34-year-old man with a dull ache around his left eye. Dig J Opthalmol. Available at: www.djo.harvard.edu/ print.php?url=/physicians/gr/310&print=1. (Accessed Oct 2004).
7. Scott SS, Kevin NW. Posner-Schlossman Syndrome, American Uveitis Society. Available at: www.uveitissociety. org/pages/diseases/pss.html (Accessed Feb 2003).
8. Geurds AM,
9. Jap A, Sivakumar M, Chee SP. Is Posner-Schlossman syndrome benign? Ophthalmology 2001 May;108(5):913-8.
10. Harrington JR. Posner-Schlossman syndrome: a case report. J Am Optom Assoc 1999 Nov;70(11):715-23.
11. Malinovsky VE. Glaucomatocyclitic crisis. J Am Optom Assoc 1983 Dec;54(12):1069-70.
12. Nagataki S, Mishima S. Aqueous humor dynamics in glaucomatocyclitic crisis. Invest Ophthalmol 1976 May;15(5):365-70.
13. Darchuk V, Sampaolesi J, Mato L, et al. Optic nerve head behavior in Posner-Schlossman syndrome. Int Ophthalmol 2001;23(4):373-9.
14. Raitta C, Vannas A. Glaucomatocyclitic crisis. Arch Ophthalmol 1977 Apr;95(4):608-12.
15. Knox DL. Glaucomatocyclitic crisis and systemic disease: peptic ulcer, other gastrointestinal disorders, allergy and stress. Trans Am Ophthalmol Soc 1988;86:473-95.
16. Bloch-Michel E, Dussaix E, Cerqueti P, Patarin D. Possible role of cytomegalovirus infection in the etiology of the Posner-Schlossman syndrome. Int Ophthalmol 1987 Dec;11(2):95-6.
17. Teoh SB, Thean L, Koay E. Cytomegalovirus in aetiology of Posner-Schlossman syndrome: evidence from quantitative polymerase chain reaction. Eye 2005 Dec;19(12):1338-40.
18. Yamamoto S, Pavan-Langston D, Tada R, et al. Possible role of herpes simplex virus in the origin of Posner-Schlossman syndrome. Am J Ophthalmol 1995 Jun;119(6):796-8.
19. Masuda K, Izawa Y, Mishima S. Prostaglandins and glaucomatocyclitic crisis. Jpn J Ophthalmol 1975;19:368-75.
20. Simmons CA, Mathews D. Prevalence of uveitis: a retrospective study. J Am Optom Assoc 1993 Jun;64(6):386-9.
21. Dinakaran S, Kayarkar V. Trabeculectomy in the management of Posner-Schlossman Syndrome. Ophthalmic Surg Lasers 2002 Aug;33(4):321-2.
22. Kass MA, Becker B, Kolker AE. Glaucomatocyclitic crisis and primary open-angle glaucoma. Am J Ophthalmol 1973 Apr;75(4):668-73.

