 |
A 31-year-old Caucasian male presented for follow-up after being diagnosed with preseptal cellulitis in his left eye. He claims compliance with his treatment regimen (Bactrim DS BID PO), but feels that his left eyelid has become more swollen and tender. His vision has remained unchanged.
Exam Findings
Entrance BCVA was 20/20 in each eye. While extraocular movements were full in both eyes, the patient reported a pulling sensation in his left eye when looking superior temporal. The left eye appeared slightly proptotic. Retropulsion assessment was inconclusive. Confrontation fields and pupil testing were unremarkable. Dilated funduscopic exam noted no apparent pathology of the posterior pole. Cup-to-disc ratios were 0.3 OU.
Despite having been treated with oral antibiotics, his condition appeared to be worsening. Could it be antibiotic resistance? Does the pulling sensation suggest early orbital cellulitis?
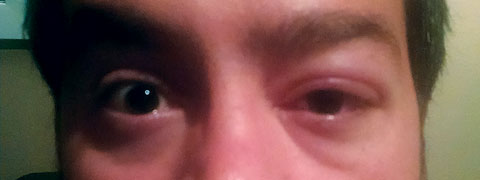 |
| This 31-year-old patient provided poor history for his swollen and tender left eyelid. |
Infection Investigation
Preseptal cellulitis refers to the infectious involvement of the eyelid and periorbital soft tissue anterior to the orbital septum. Conversely, orbital cellulitis is the infectious involvement of tissue posterior to the orbital septum, including the fat and muscle within the bony orbit. The distinction is important because a delay in diagnosing orbital cellulitis may be associated with visual and life-threatening sequelae.
Anatomically, the orbital septum is a thin, fibrous, multi-laminated membrane made up of connective tissue that acts as the anterior boundary of the orbit. It extends from the orbital rim to the lids and contains orbital fat.1 Certain blood vessels and nerves pass through the septum from the orbital cavity to the face and scalp. Venous drainage of the paranasal sinuses and the mid region of the face occur primarily via the orbital veins, which communicate directly with the cavernous sinus. If the cavernous sinus becomes infected, it may adversely affect structures within the sinus (i.e., oculomotor nerve, trochlear nerve, abducens nerve and branches of the trigeminal nerve, internal carotid artery), and extend posteriorly to the pituitary gland and surrounding meninges, and that can be life-threatening.2
When to Opt for Surgery
|
When confronted with a patient who has lid and periorbital soft tissue erythema and swelling, a detailed case history is warranted. One of the more common causes of preseptal cellulitis is extension from a paranasal sinusitis.3,4 These patients may report an acute or chronic history of sinus congestion and headache. Other sources of soft tissue infections include skin infections, lid infections (e.g., chalazia, hordeola), dacyrocystitis, trauma (e.g., orbital fracture, foreign body) and insect bites. Preseptal and orbital cellulitis may also be iatrogenic from recent lid, sinus, dental or maxillofacial surgery.5
A complete and thorough eye examination should include visual acuity assessment, pupil testing, confrontation fields, extraocular motility assessment, tonometry, slit-lamp biomicroscopy and direct and indirect ophthalmoscopy. In distinct contrast to preseptal cellulitis, eyes with posterior septal involvement may show proptosis, limitation in motility, resistance to retropulsion, orbital pain, an afferent pupillary defect, optic nerve head edema and venous engorgement. A decrease in vision should also raise suspicion for post-septal extension.
Initial treatment of preseptal cellulitis in adults usually consists of empirically prescribed oral antibiotics based on any predisposing risk factors. This is assuming the patient will be compliant. If the adult patient reports a history of acute or chronic sinusitis, then oral antibiotics geared towards Staph and Strep (pneumoniae and pyogenes) species, as well as H. influenza and M. catarrhalis is warranted. In focal trauma, suspect Staph aureus.2
Treatment
Antibiotics of choice for preseptal cellulitis include amoxicillin-clavulanate, cefuroxime, gatifloxacin, moxifloxacin and levofloxacin. Patients who report a history of resistant infections will require a more detailed case history to determine which antibiotic is warranted and whether the oral or IV route of administration is most appropriate. Patients who fail to respond or demonstrate clinical worsening while on oral antibiotics should be promptly transitioned to intravenous antibiotics as the possibility of a resistant strain exists. In the case of an immunocompromised patient, also consider a fungal etiology (i.e., mucormycosis or aspergillus).
When you encounter purulent discharge (i.e., dacyrocystitis, draining lid lesions, etc.), perform culture and sensitivity testing. Attempts to isolate the causative organism through blood cultures or nasal swab may provide conflicting information and is generally not recommended in preseptal cases.
A critical component in the evaluation of a declining preseptal cellulitis or orbital cellulitis is radiographic imaging. Both computed tomography (CT) scans and magnetic resonance imaging (MRI) allow for confirmation of disease extension into the orbit, concurrent sinusitis, as well as orbital or periosteal abscess.6,7 Contrast dyes help differentiate inflammation from abscess in involved orbital tissue. While MRI provides more detailed information, MRI services may not be readily available at all hours, hindering the clinician’s ability to render appropriately prompt therapy. If radiographic imaging confirms post-septal extension on the infection, start the patient on intravenous antibiotics promptly. If culture and sensitivity results are not readily available, empiric treatment is geared towards the most common causative organisms, Staphylococcus and Streptococcus.
Local hospitalists and specialists in infectious disease will likely have a clear understanding of local trends in antimicrobial susceptibility. Additionally, most hospitals track and maintain infection trends in the form of an antibiogram, which can aid in designing a treatment plan. If local community-acquired MRSA infection rates are high, consider ancillary treatment with IV vancomycin.
Follow Up
Our patient was a relatively poor historian. Given this, he reported no history of sinusitis, injury or previous surgery. He also reported no allergies. Based on his assurance that he was compliant with his oral Bactrim DS (sulfamethoxazole and trimethoprim, Roche), a lengthy discussion ensued regarding the need for imaging and consideration of IV antibiotics, as I could not rule out MRSA or similar resistant strain. He was being seen in a remote clinic, so daily monitoring at our clinic was not an option. Instead, we referred him to a co-management center nearby. After a same-day consult, the ophthalmologist decided to add second-line oral antibiotic therapy—Augmentin (amoxicillin and clavulanate, GlaxoSmithKline) 500mg/125mg TID, pending a CT scan of the sinuses and orbit. If the CT scan were to suggest impending or post-septal involvement, IV cefuroxime 1.5g q8h +/- 1g vancomycin Q12h would likely be ordered. Our patient was educated on the importance of compliance with his oral antibiotics, CT imaging and follow-up appointments.
CT imaging (coronal and axial views) of the sinuses and orbits were performed with and without contrast dye. Findings were consistent with a preseptal cellulitis, absent of sinusitis. No post-septal extension was seen. The patient was followed daily for the first three days. Shortly after second-line therapy was initiated, the lid edema and erythema improved and, within two weeks, resolved.
Orbital cellulitis is a true medical emergency. In an era when bacterial resistance is on the rise, even preseptal cellulitis cases warrant close monitoring, especially in patients with predisposing risk factors. Preseptal cases can progress to orbital cellulitis in short order. Knowing the risk factors for orbital cellulitis, as well as the most common causative organisms for such an infection, will put you in a strong position to appropriately care for your patient.
|
1. Koornneef L. Orbital septa: anatomy and function. Ophthalmology. 1979;86(5):876-80. 2. Howe L., Jones N., Guidelines for the management of periorbital cellulitis/abcess. Clin. Otolaryngol. 2004:29;725-8. 3. Jones D, Steinkuller P, Strategies for the initial management of acute preseptal and orbital cellulitis. Trans. Am. Ophthalmol. Soc. 1988;86:94–108. 4. Oxford L, McClay J. Complications of acute sinusitis in children. Otolaryngol. Head Neck Surg. 2005;133:32–7. 5. Cox N, Knowles M, et al. Pre-septal cellulitis and facial erysipelas due to Moraxella species. Clin. Exp. Dermatol. 1994;19:321–3. 6. Eustis H, Mafee M, Walton C, Mondonca J. MR imaging and CT of orbital infections and complications in acute rhinosinusitis. Radiol. Clin. North Am. 1998;36(6):1165–83. 7. Towbin R, Han B, Kaufman R, Burke M. Postseptal cellulitis: CT in the diagnosis and management. Radiology. 1986;158:735–7. |

