 |
A long-standing patient is on the phone with your receptionist. She’s in a panic because her husband accidently got splashed in the eye with a chemical he uses for fertilizing his crops. He’s in severe pain and can barely open his eye. He’s currently in the shower with the water running over his eyes and face. She’s sure you and your staff will help her through this crisis. You hear your receptionist tell her to bring him into the office immediately.
Is this really the right suggestion? What response can she recommend they take before leaving? Should she ask any other questions? What can you do to prepare for this patient? In other words, are you and your staff prepared for such a phone call?
Types of Chemical Burns
An ocular chemical burn is considered a true ocular emergency. Whether by gas, liquid or solid, an acid or alkaline base can cause irreversible damage to the eye and adnexa if urgent action is not taken.
Alkali agents (pH of 10 or greater) such as ammonia (found in cleaning agents, fertilizers and refrigerants), lye (drain and oven cleaners, air bags), magnesium hydroxide (in firework sparklers, flares) and lime (in plaster, mortar, cement, white wash) are lipophilic and penetrate the corneal stroma through saponification of fatty acids in cellular membranes. Once stromal tissue is damaged, proteolytic enzymes are released that furthers tissue damage, also known as liquefactive necrosis.
|
|
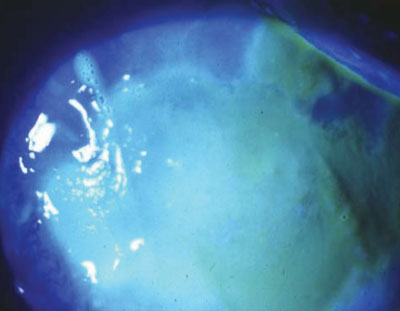
| This slit lamp image shows a patient who splashed bleach in her eye while cleaning. Photo: Bradley Sutton, OD |
|
Acid-based agents (pH of 4 or less) such as sulfuric acid (in car batteries), acetic acid (vinegar) and hydrochloric acid (swimming pool cleaners) are generally considered less harmful than alkali substances. Acids usually bind with tissue proteins, causing coagulation and stopping further penetration. One exception is hydrofluoric acid (found in refrigerants, fluorescent bulbs, glass polishing and mineral refining) where the fluoride ion can rapidly penetrate corneal tissue and cause severe, sight-threatening damage.
Irrigation
Certain substances can rapidly penetrate into the eye and cause irreversible intraocular damage in as little as five minutes. The first and most important step in management of an acute ocular chemical splash injury is copious irrigation. This, ideally, should begin wherever the injury took place. At home, the patient can perform this irrigation in the shower or using an outdoor hose, or at the workplace using a sink or designated eye wash station.
If irrigation begins immediately after the splash occurs, pH levels often normalize within 30 minutes of continuous irrigation (about one to three liters).
If delayed, irrigating volumes can sometimes exceed 20 liters before reaching physiologic pH levels. This is largely due to chemical deposition in ocular tissue that becomes more recalcitrant to irrigation. When triaging the patient over the phone, ask about the timing and severity of the burn.
Irrigation in the office or emergency room can be performed with either a Morgan lens or a standard nasal cannula that is positioned and sometimes taped to the bridge of the nose, to provide a similar steady flow to both eyes.
Evaluating Severity
Once the ocular surface pH is stable, perform a thorough case history and ocular examination to ascertain the extent and depth of injury. The most common symptoms are severe pain, photophobia, epiphora, blepharospasm and reduced vision. Slit-lamp exam should focus not only on the cornea, limbus and conjunctiva but external adnexa as well.
IOP readings are important too, as alkaline chemical burns may cause immediate, near-immediate or delayed rises in IOP.
While no “cookie-cutter” ap-proach to managing acute ocular chemical burns exists, more than one classification scheme is available to assist in formulating a prognosis and secondary treatment plan. One such scheme is the Roper-Hall classification method (Table 1).
| Table 1. Roper-Hall Classification Method for Ocular Chemical Burns | |||
| Grade | Prognosis | Cornea | Conjunctiva/Limbus |
| I | Good | Corneal epithelial damage | No limbal ischemia |
| II | Good | Corneal haze, iris details visible | <1/3 limbal ischemia |
| III | Guarded | Total epithelial loss, stromal haze, iris details obscured | 1/3 to 1/2 limbal ischemia |
| IV | Poor | Cornea opaque, iris and pupil obscured | >1/2 limbal ischemia |
Treatment Goals
The goal of treatment is to promote reepithelialization, while controlling inflammation and minimizing the adverse sequelae that often follow a chemical injury. Acute phase treatment often includes a broad-spectrum antibiotic, cycloplegic and anti-glaucoma therapy. Other treatment considerations are included in Table 2.
| Table 2. Treatment Considerations for Chemical Burns | |
| Grade I |
Prednisolone acetate 1% QID
Topical antbiotic ung (e.g., erythromycin) QHS to QID Preservative-free artificial tears PRN Consider cycloplegic for pain PRN |
| Grade II |
Topical antbiotic (e.g., fluoroquinolone) QID
Prednisolone acetate 1% Q1H while awake with rapid taper between days 10-14 Long-acting cycloplegic (i.e., atropine 1%) Oral pain medication PRN Oral doxycycline to reduce risk of corneal melting through MMP inhibition Oral vitamin C (1,000mg to 2,000mg) QID Sodium ascorbate drops (10%) Q1H while awake Preservative-free artificial tears PRN Debridement of necrotic tissue, using tissue adhesive as needed |
| Grade III |
Same as Grade II
Amniotic membrane application (e.g., Prokera)—best if used during the first two weeks of injury |
| Grade IV |
Same as Grades II & III
For significant necrosis, a tenonplasty can help re-establish limbal vascularity Stem cell transplantation Penetrating keratoplasty Keratoprosthesis |
If an eye shows elevated IOP, aqueous suppression is the first choice. Oral therapy is preferable, barring any contraindications, until reepithelialization occurs. For some chemical burns, reepithelialization may take 10 to 14 days. If it doesn’t occur within 21 days, the risk of permanent vision loss is significant. Consult a corneal specialist early in the management process so that the patient can undergo timely surgical treatment, should medical management prove insufficient.
|
|
10 Telephone Triage Tips for Chemical Splashes and Burns
1. Upon hearing of a chemical splash injury, make sure that the preliminary irrigation process begins on site before the patient seeks care. 2. If the chemical splash occurred outside of the workplace, remind the caller that the shower or an outdoor hose is an adequate option. 3. Attempt to determine time lapse between burn event and when irrigation started. 4. Attempt to determine the type of chemical that entered the eye(s). 5. Attempt to determine if the patient is wearing contact lenses. Irrigation should not stop in an effort to remove contact lenses. 6. Irrigation should take place for a minimum of 20 to 30 minutes before the patient is brought to the office or emergency room. 7. When the patient is ready to make the trip to the ER or office, remind them to bring the container that held the offending chemical. Important information may be obtained from the labeling. 8. If the injury occurred in the workplace, ask the patient to bring the MSDS (material safety data sheet) if available. 9. If the injury occurred where there is no or limited access to water for irrigation, refer them to the nearest emergency room or your office, whichever is closer. 10. Assist with dispatching emergency services as needed. |
Time is of the Essence
An ocular chemical burn can be devastating to the eye and to vision. Time is of the essence for this ocular emergency. Establish a practice-wide ocular injury protocol that includes chemical splashes to the eye. Telephone triage is vital in these cases, so make sure staff is properly trained on how to handle such calls. By doing so, you may make a tremendous difference in the lives of one or more of your patients.
2. Kuckelkorn R, Makropoulos W, Kottek A, Reim M. Retrospective study of severe alkali burns of the eyes. Klin Monbl Augenheilkd. 1993;203:397–402.
3. Fish R, Davidson RS. Management of ocular thermal and chemical injuries, including amniotic membrane therapy. Curr Opin Ophthalmol 2010, Jul;21(4):317–21
4. Herr RD, White GL, Bernhisel K, et al. Clinical comparison of ocular irrigation fluids following chemical injury. Am J Emerg Med 1991;9:228–31.
5. Cavanagh, HD. Contact Lenses in the Industrial Workplace: Are They Safe? The CLAO Journal, 1992, Jan:18(1):11.

