Many of this years presentations involving the retina deal with the debate between Avastin (bevacizumab) and Lucentis (ranibizumab), both by Genentech, Inc., in the treatment of age-related macular degeneration (AMD).
The possible use of Avastin in treating diabetic retinopathy and central or branch retinal vein occlusions also figures prominently in this years selection; but, some studies found that Avastin, when used in treatment of diabetic retinopathy, may play a role in causing a tractional retinal detachment (TRD).
Other research presented this year discusses the possibility of genetic predisposition to or against AMD. And, optical coherence tomography (OCT) is being tested in new environmentswith promising results.
Avastin or Lucentis for AMD?
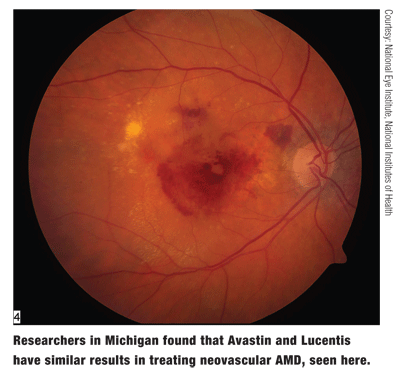 Its still a dead heat: Researchers found that the short-term results of treatment of neovascular AMD with Lucentis and Avastin are very similar.1813/B673 Researchers in
Its still a dead heat: Researchers found that the short-term results of treatment of neovascular AMD with Lucentis and Avastin are very similar.1813/B673 Researchers in
Whats next in this standoff? Researchers recommend a long-term study of both drugs effects. To this end, the National Eye Institute is funding an independently-conducted head-to-head study that will compare the drugs efficacy.
Other Uses for Avastin
But, will Avastin hold its spotlight beyond the treatment of AMD? Researchers in
Of the 28 eyes of 28 patients who had CNV due to ocular histoplasmosis syndrome, four eyes maintained current visual acuity, four eyes experienced decreased acuity, and 20 eyes experienced an increase in visual acuity by 0.38 LogMAR units.1458/B535
All of the 18 patients who had CNV due to pathologic myopia experienced an improvement in best-corrected visual acuityfrom 5.34/20 to 8.24/20 between injection and follow-up at three months.1451/B528 At nine months, 90% of patients presented with improvement of one to three Snellen lines. The other 10% showed stabilized acuity. No patients demonstrated significant ocular or systemic side effects.
Avastin has also been used to treat cases of macular edema secondary to branch retinal vein occlusion (BRVO)312/B365 as well as central retinal vein occlusions (CRVO).302/B355 It was also used preoperatively in cases of proliferative diabetic retinopathy.4031 Each study produced promising results, though the researchers, from Philadelphia, Miami and Santa Barbara respectively, indicate that further investigation is needed.
In the BRVO study, sixteen patients who had BRVO and underwent at least one intravitreal injection of Avastin were examined, with a follow-up period from four to 17 months.312/B365 The mean baseline visual acuity was 20/230 and improved to a mean acuity of 20/70 at one month. At final follow-up, the mean acuity was 20/50. Significant improvement in the central corneal thickness was also noted, and no systemic or ocular complications were seen.
In the CRVO study, the mean baseline visual acuity of the 44 patients presenting with CRVO was 17 letters.302/B355 At one month, it was 28; at three, it was 31; and at six, it decreased slightly to 26. By six months of follow-up, 5% of patients had lost three Snellen lines of visual acuity.
Among patients with proliferative diabetic retinopathy, the preoperative use of 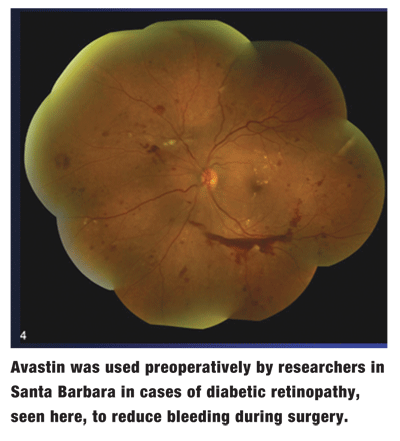 Avastin in 57 eyes of 52 patients prior to vitrectomy rapidly slowed diabetic neovascularization, which resulted in less bleeding during surgical removal of fibrovascular proliferations.4031 Postoperatively, 14 eyes demonstrated recurrent vitreous hemorrhage, one eye demonstrated retinal detachment, and one patient developed a tractional rhegmatogenous retinal detachment.
Avastin in 57 eyes of 52 patients prior to vitrectomy rapidly slowed diabetic neovascularization, which resulted in less bleeding during surgical removal of fibrovascular proliferations.4031 Postoperatively, 14 eyes demonstrated recurrent vitreous hemorrhage, one eye demonstrated retinal detachment, and one patient developed a tractional rhegmatogenous retinal detachment.
Researchers note the benefit of Avastin preoperatively, but note that further study is needed to determine if these postoperative side effects result from the Avastin.
Side Effects of Avastin
Other researchers noted negative side effects in the use of Avastin, as well. Researchers in Mexico studied cases of tractional retinal detachment after injection of Avastin for treatment of proliferative diabetic retinopathy,1412/B468 while researchers in six western countries organized a joint retrospective to study this side effect.1411/B467 These studies demonstrate the learning curve present with any new drughow best to use it therapeutically.
The cases studied in Mexico each required pars plana vitrectomy, removal of epiretinal fibrovascular membranes, photocoagulation and insertion of a silicone tamponade.1412/B468 Researchers warn that tractional retinal detachments may occur a short time after intravitreal injection of Avastin in patients with proliferative diabetic retinopathy.
The joint retrospective, in reviewing a wide variety of cases, found that tractional retinal detachments are rare in patients who have been treated for proliferative diabetic retinopathy with Avastin prior to surgery, occurring at a rate of 4.7%.1411/B467 Researchers note that a longer time span between injection and vitrectomy, patient history and improperly-managed diabetes mellitus may also impact the likelihood of a tractional retinal detachment.
Genetic Factors Aid AMD
Also presented this year are findings about genetic factors that can predispose a patient to AMD or impact the treatment of a patients case of AMD. Understanding the genetic factors to a disease such as AMD will aid the eye-care practitioner in identifying warning signs, not to mention that it will aid in disease management and treatment.
Researchers in
A variant of a gene that increases risk of AMD among whites was found by researchers in Maryland.3653 In testing the relation between CHF on chromosome 1q32 and the HtrA1 protein, they found that the proteins location varied widely and that it didnt interact with the CFH as expected. But, they did find that white patients with AMD presented with a higher incidence of a specific HtrA1 variant.
Also, the presence, absence or location of the CFH genotype affects how a patient with AMD reacts to treatment with Avastin, found researchers in St. Louis.5103/B251 Specifically, researchers examined patients with AMD for the TT genotype, the TC genotype and the CC genotype. While those with the TT and the TC genotypes of CFH demonstrated improvement of visual acuity (20/215 to 20/100 and 20/185 to 20/150, respectively), those with the CC genotype of CFH experienced a decrease in visual acuity upon treatment with Avastin: from 20/180 to 20/190.
Researchers suggest that determining patients CFH genotype prior to treatment could allow the managing practitioner to tailor their treatment in cases of exudative AMD.
New Uses for OCT
Many presentations and posters this year discuss the progression and evolution 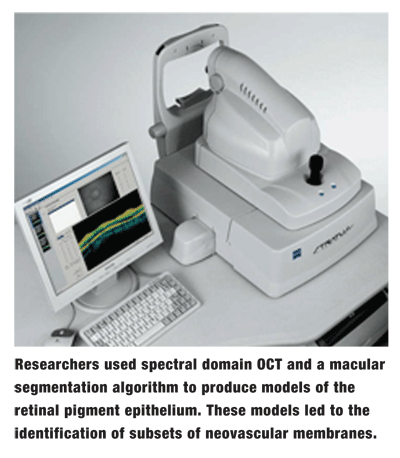 of this technology, and the potential of spectral domain optical coherence tomographyespecially in a retina practice. Researchers presented results of studies that required modification or new uses of the optical coherence tomograph (OCT). Its modification into a system that could examine infants eyes safely and easily,2585/B662 as well as its success in three-dimensional modeling of choroidal neovascularization,1456/B533 suggest that the OCT will become an increasingly useful tool in observation, diagnosis and management of retinal conditions.
of this technology, and the potential of spectral domain optical coherence tomographyespecially in a retina practice. Researchers presented results of studies that required modification or new uses of the optical coherence tomograph (OCT). Its modification into a system that could examine infants eyes safely and easily,2585/B662 as well as its success in three-dimensional modeling of choroidal neovascularization,1456/B533 suggest that the OCT will become an increasingly useful tool in observation, diagnosis and management of retinal conditions.
An OCT-3 was modified with a custom-built stage and infant carrier to allow for comfort, safety and ease of use in examining the eyes of anesthetized infants.2585/B662 No complications were reported regarding positional changes, oxygen saturation or temperature stability. All the patients maculae were successfully imaged; one patients diagnosis of X-linked retinoschisis was confirmed by OCT evaluation.
Spectral domain OCT was used in conjunction with a macular segmentation algorithm to produce a model of patients retinal pigment epithelia, which were then compared to fundus photos and fluorescein angiograms.1456/B533 These models allowed researchers to identify distinct subsets of choroidal neovascular membranes.
Dr. Dunbar is Director of Optometric Services and Optometry Residency Supervisor at Bascom Palmer Eye Institute in
302/B355. Gaitan JR, Gregori NZ, Rosenfeld PJ, et al. Intravitreal bevacizumab (Avastin) for macular edema secondary to central vein occlusions.
312/B365. Badala F, Brown G, Brown M, et al. Intravitreal bevacizumab (Avastin) treatment of macular edema associated with branch retinal vein occlusion.
1411/B467. Maia M, Flynn HW, Saravaia M, et al. Development or progression of tractional retinal detachment after intravitreal bevacizumab (Avastin) in severe proliferative diabetic retinopathy.
1412/B468. Alvarez-Verduzco O, Torres-Sorjano M, Reyna-Castelan E, et al. Tractional retinal detachment after intravitreal injection of bevacizumab in proliferative diabetic retinopathy.
1451/B528. Zucca I, Orru F, Vinci M, et al. Bevacizumab (Avastin) intravitreal injection in patients with choroidal neovascularization associated with pathologic myopia.
1456/B533. Lujan BJ, Gregori G, Rosenfeld PJ, et al. Three-dimensional modeling of choroidal neovascularization using spectral domain optical coherence tomography.
1458/B535. Schadlu R, Sheybana A, Shah GK, et al. Intravitreal bevacizumab for the treatment of choroidal neovascularization in ocular histoplasmosis syndrome.
1813/B673.
2585/B662. Rich RM, Berrocal A, Parel J, et al. The Bascom Palmer Eye Institute pediatric OCT dystemour initial experience.
3653. Bojanowski CM, Tuo J, Ross RJ, et al. Variants within HTRA1 and LOC387715 independent of CFH are associated with an increased risk of age-related macular degeneration in a caucasian population.
3654. Khatibi NH, S.Teymoorian S, Memarzadeh M, et al. The association of complement factor H polymorphism (CFH), elongation of very long chain fatty acids-like 4 (ELOVL4) and Apolipoprotein E (ApoE) in age-related macular degeneration (AMD).
4031. Avery RL, Pieramici D, Rabena M, et al. Intravitreal bevacizumab (Avastin) in the surgical treatment of proliferative diabetic retinopathy.

