 |
A 61-year-old female was referred for neurological evaluation because she reported seeing constant textured spots surrounded by a white halo in her vision. She had floaters in the past, but felt this was different. She also noted flashes of light for the past two years that were more prominent in the superior nasal field of both eyes. She denied a history of headaches, seizures or trauma.
Her past ocular history was significant for macular edema following cataract surgery in both eyes and a retinal tear in the left eye treated with laser retinopexy.
Upon examination, her best corrected vision was 20/40 OD and 20/60 OS. She had full fields to confrontation with finger counting and full motilities. Her pupils were equally round and reactive to light with no afferent pupillary defect. Intraocular pressure (IOP) was 19mm Hg OD and 20mm Hg OS.
A slit lamp examination of the right eye was remarkable for a few fine keratic precipitates inferiorly and trace cell in the anterior chamber. The left eye also had trace cell in the anterior chamber.
On dilated fundus exam, both eyes were positive for +1 cell in the vitreous, grade 1 optic nerve edema, retinal pigment epithelium (RPE) changes in the macula and extensive streaks and punctate depigmentation in the periphery (Figures 1 and 2).
OCT images of both eyes were also taken (Figures 3 and 4). Finally, fluorescein angiography (FA) was ordered at the visit (Figure 5). Our patient’s lab test results appeared to be normal.
Take the Retina Quiz
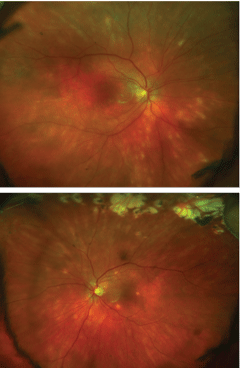 |
| Figs. 1 and 2. Above, these fundus images show a variety of signs including; optic nerve edema, changes to the RPE and extensive streaks and punctate depigmentation in the periphery. |
1. What is the late-stage FA finding seen on both eyes?
a. Staining from vasculitis.
b. Leakage from vasculitis.
c. Staining from optic nerve swelling.
d. Hypofluorescence from macular edema.
2. The patient is HLA-A29 (+); what is the most likely diagnosis?
a. Multiple evanescent white dot syndrome.
b. Serpiginous choroiditis.
c. Birdshot chorioretinitis.
d. Multifocal choroiditis.
3. What does the OCT reveal?
a. Outer retinal tubules.
b. Macular schisis.
c. Cystoid macular edema.
d. Choroidal neovascularization.
4. How should this patient be treated?
a. Anti-VEGF.
b. Antivirals.
c. Laser photocoagulation.
d. Steroid and immunosuppressives.
For answers, see below.
Diagnosis
Our patient had a history of chronic treatment with topical steroids and nonsteroidal anti-inflammatory drops for the past three years for presumably cystoid macular edema that developed as a complication of her cataract surgery. However, based on demographics, history, symptoms, clinical findings, imaging, normal blood lab results and HLA-A29 positivity, our patient actually has birdshot chorioretinitis (BSCR).BSCR is among a group of idiopathic multifocal inflammatory conditions involving the retina and the choroid that are known as the “white dot syndromes,” characterized by white dots in the fundus. These include acute posterior multifocal placoid pigment epitheliopathy, serpiginous choroiditis, multiple evanescent white dot syndrome, multifocal choroiditis and panuveitis, punctate inner choroidopathy and diffuse subretinal fibrosis.
The spectrum of conditions responsible for the “white dot syndromes” is broad; however, a careful history and detailed clinical examination can help narrow the differential diagnosis.
Our patient was in her sixth decade of life when the symptoms began (two years before being referred to us) and had developed a bilateral and chronic process where inflammation is mostly limited to the posterior segment. In addition, she had negative lab results, which helped rule out infectious, autoimmune and neoplastic etiologies. She did have a positive HLA-A29, a haplotype that 85% to 95% of affected BSCR patients carry.1
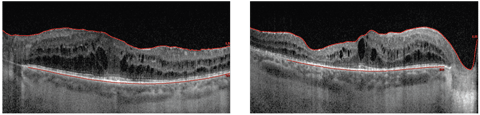 |
| Figs. 3 and 4. Above, do the patient’s OCT images help identify a diagnosis? |
Discussion
The hallmark of the disease is the presence of multiple hypopigmented, cream-colored, irregularly shaped choroidal lesions, often clustered around the optic disc; optic nerve edema; retinal vasculitis; and vitritis with no snow banking.1 A mild anterior uveitis may be present with minimal to no keratic precipitates. It is usually seen in middle-aged Caucasian females 30 to 70 years old. It is bilateral, idiopathic and has an insidious onset. BSCR represents 6% to 8% of all posterior uveitis.2 The pathogenesis of inflammation occurs independently but simultaneously in the choroid and the retina. The pathophysiology is poorly understood. Only two histological reports have been published indicating that the hypopigmented choroidal lesions represent nodules of lymphocyte aggregation and that retinal involvement is characterized by an exudative vasculopathy involving both small capillaries and large retinal vessels.3Symptoms of floaters and flashes were consistent with birdshot lesions located, primarily, in the nasal peripapillary choroid, but also beyond the vascular arcades up to the midperiphery. Early-stage birdshot chorioretinitis (when “birdshot” lesions are not yet present) can only be diagnosed or confirmed by using indocyanine green angiography (ICG), which reveals evenly distributed occult choroidal hypofluorescent dark dots.4 Decreased visual acuity in these patients is attributed to macular edema. However, nyctalopia and color vision deficiencies may precede decreased visual acuity and the onset of classic depigmented spots in the fundus by several years.
Management and Treatment
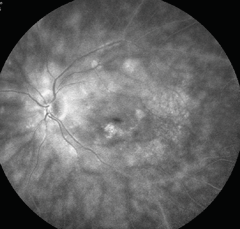 |
| Fig. 5. What can this fluorescein angiography image, combined with our patient’s medical history, tell you? |
The creamy-light colored lesions will fade over time and be replaced by diffuse pigmentary loss. FA can provide panoramic information on retinal inflammation and is useful to assess complications and treatment response of cystoid macular edema, retinal vasculitis and optic nerve edema. ICGA is more sensitive than FA and detects choroidal inflammation in early stages of the disease.4 OCT helps to monitor macular edema, retinal thickness and atrophy. Visual outcome is dependent on visual acuity at the onset of the treatment; early intervention and targeted treatment may improve a patient’s outcome.5
Because of the chronic nature of this disease, patients with BSCR are usually treated with a combination of oral steroids (prednisone 40mg to 60mg) and a second-line immunosuppressive agent.1 These include T-cell inhibitors, antimetabolites and biologics (anti-TNF). Once the disease is under control, the steroid may be stopped. However, most patients will need to maintain use of one of the second-line immunosuppressive agents indefinitely. There’s no accepted optimal treatment protocol, and switching between agents can be useful. Planned therapy is at least four to five years.
Localized ocular immunosuppressive therapy in the form of a steroid implant may also control inflammation. Examples of these medications include Ozurdex (dexamethasone, Allergan) and Retisert (fluocinolone acetonide, Bausch + Lomb).6
Our patient was first treated with oral prednisone 40mg, then started on CellCept (mycophenolic acid, Genentech)- 1g twice daily with oral prednisone taper. Given the unsuccessful resolution of her macular edema, the patient was started on tacrolimus 1mg twice daily and given Ozurdex injection in both eyes, which helped stabilize edema for only a month. The patient was then switched from tacrolimus to cyclosporine 150mg a day, but continued having persistent macular edema with further vision loss. She was then treated with Retisert in both eyes, which resolved her macular edema for the past six months. Unfortunately, she developed steroid-induced glaucoma and will likely need a glaucoma drainage device.
Dr. Gomez is an optometric resident at the Bascom Palmer Eye Institute in Miami.
|
1. Shah K, Levinson R, Yu F, et al. Birdshot chorioretinopathy. Surv Ophthalmol. 2005;50:519-41. 2. Levinson R, Brezin A, Rothova A, et al. Research criteria for the diagnosis of birdshot chorioretinopathy: results of an international consensus conference. Am J Ophthalmic. 2006;141:185-7. 3. Shao E, Menezo V, Taylor S. Birdshot chorioretinopathy. Curr Opin Ophthalmol. 2014;25:488-94. 4. Papadia M, Herbort C. Indocyanine green angiography (ICGA) is essential for the early diagnosis of birdshot chorioretinopathy. Klin Monbl Augenheilkd. 2012;229(4):348-52 5. Rothova A, Berendschott T, Probst K, et al. Birdshot chorioretinopathy: long term manifestation and visual prognosis. |
Retina Quiz Answers:
1) b; 2) c; 3) c; 4) d.

