 |
Q:
A 45-year-old female in good health presents with subepithelial infiltrates and a red eye. It looks like simple epidemic keratoconjunctivitis. However, the patient is lethargic with labored breathing. Do I just assume that her eye infection is causing her to feel bad?
A:
“When this patient presented to me, I suspected something else was going on,” says Carlton Edwards, OD, in private practice in Douglasville, GA. Both eyes had been red for only three days, yet there were corneal infiltrates noted in both eyes, says Dr. Edwards. “It didn’t add up, so I made an immediate referral to her internist, which led to hospital admission.”
An obvious ocular condition in conjunction with non-specific systemic complaints should catch your attention, as a potentially life-threatening condition could be at work, says Joseph Shovlin, OD, a practitioner at Northeastern Eye Institute in Scranton, PA, and president of the American Academy of Optometry. “Always gauge the general health of your patient and respond to any symptoms that appear sinister or unexpected,” says Dr. Shovlin. Although patients are often very uncomfortable with adenovirus infection, severe malaise or a feeling that they are very ill are out of the norm, Dr. Shovlin explains. “If these symptoms occur, it’s imperative that clinicians evaluate the patient for additional systemic ailments.”
Corneal signs, including infiltrates, can certainly be a manifestation of an underlying systemic disease, such as the nummular infiltrates found in Lyme disease and numerous corneal findings of the herpes family of infections, says Dr. Shovlin. He says to monitor patients for any unusual symptoms and follow closely when indicated. “As my mentor once said, ‘When all else fails, re-examine,’” says Dr. Shovlin.
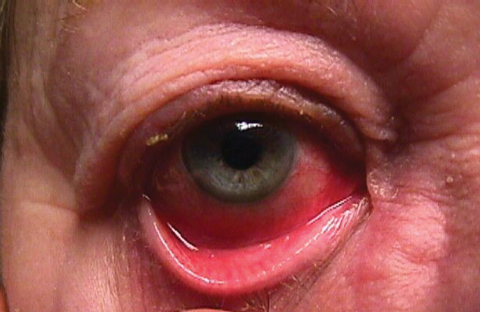 |
| An ill eye, along with non-specific systemic complaints, could signal a serious systemic condition is afoot. |
Back to Square One
To unravel the mystery of your patient’s illness, Dr. Shovlin says to start by asking them for all the facts. “A detailed history is always a great place to start,” says Dr. Shovlin. Ask about timing, onset and the exact symptoms, he says, as well as severity and frequency.
Investigate the Infiltrate
Next, see what the corneal disruption might suggest. Infiltrates— aggregates of white blood cells—have multiple causes, says Dr. Shovlin. He explains that the number, location and level of corneal involvement may provide some clues as to the etiology. “The central cornea and the periphery have key anatomical and physiological differences, and mitotic rates and corneal nerve density differ greatly,” he explains. A careful history, along with patient symptoms and a detailed examination of the cornea and adnexa, are essential in differentiating a sterile from an infectious process.
“Remember that, histologically, all infections have infiltration with, or occasionally without, overlying defects or frank ulceration,” he says. “In this case, the patient presents with diffuse subepithelial infiltrates that may signal a viral cause. Generally, infiltrates in adenovirus disease present the second week and, if vision is affected significantly, topical steroid drops such as loteprednol etabonate are indicated.”
It just so happens that in this case, the viral cause wasn’t located in the eye. Rather, it was located in the heart. Dr. Edwards spoke to the patient’s internist a week later, and “the workup confirmed a systemic viral infection, which led to premature ventricular contractions. The cardiomyopathy that ensued could have taken the patient’s life if it had been ignored,” says Dr. Edwards.
As medical professionals, optometrists are responsible for the health of their patients in every area, across organ systems. The ocular system is often a window into the rest of the body. When practitioners remain vigilant and suspicious, they have the best opportunity to save the life of their patients.

