 |
A 41-year-old white male welding student presented to the clinic for an emergency visit. He had been sharpening tungsten, a type of metal, in class that morning without wearing safety glasses when a fragment pierced his left eye. His vision was severely impacted, and he reported immense pain, which he described as a throbbing, aching sensation, and constant tearing.
The patient had type 2 diabetes, his medications and social history were not pertinent to the case and he had no known drug allergies.
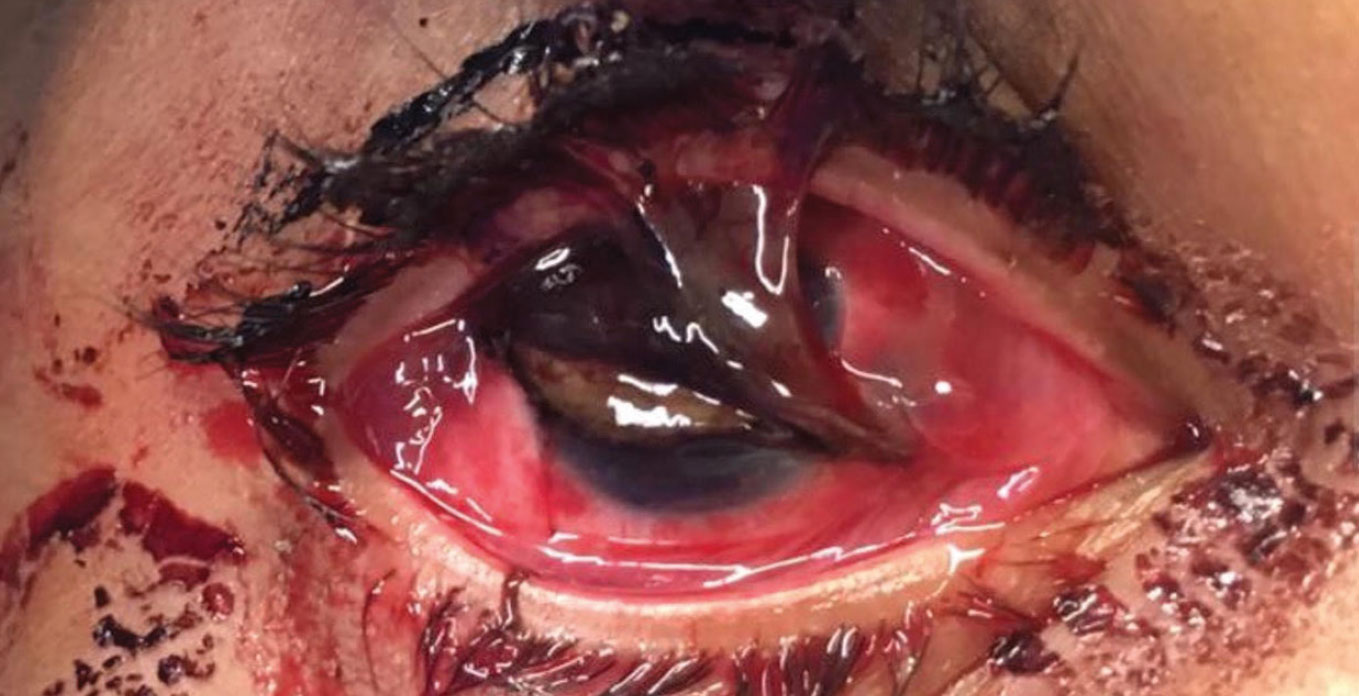 |
| A full-thickness corneal laceration with iris prolapse in a patient with a similar injury to the case described here. Photo: Brian Shafer, MD. Click image to enlarge. |
Case
The patient’s entering visual acuity was 20/150 with no improvement with pinhole in the left eye. Intraocular pressure was not evaluated. Upon slit lamp exam, a full-thickness corneal laceration was present nasally, extending from five to 10 o’clock with iris prolapse. Upon fundus exam, the posterior pole appeared normal with a limited view of the periphery. There were no signs of an obvious break, hole or tear.
The patient was diagnosed with an open globe secondary to a corneal laceration of the left eye, and urgent repair was recommended. The patient was informed that his visual prognosis would be guarded. Prednisolone acetate and moxifloxacin were initiated following surgery with instructions to take one drop of each eight times daily. The patient was to return to the clinic the following day.
At the one-day post-op exam, the patient presented with a visual acuity of 20/1250 with no improvement with pinhole in the left eye. Intraocular pressure was 12.3mm Hg. The corneal laceration was well apposed, with an overlying epithelial defect. Within the anterior chamber, a small hyphema was present and the pupil was dragged temporally with no apparent signs of entrapment within the wound.
At the two-week mark following globe repair, the patient’s visual acuity was 20/300 with a stable intraocular pressure, and the epithelial defect had healed. Upon dilation of the left eye, the optic nerve appeared well perfused with no clinical retinal nerve fiber layer defects. No breaks, holes or tears were observed within the periphery of the retina. Moxifloxacin was discontinued, with prednisolone acetate decreased to one drop four times daily. The patient was scheduled for a follow-up exam in another two weeks.
Four weeks post-open globe repair, the patient was 20/250 with his left eye and pinholed to 20/100. All findings of the anterior and posterior segments were stable with a macular OCT demonstrating normal macular contour. Prednisolone acetate was to be tapered by one drop each week. A four- to six-week follow-up was scheduled to continue monitoring healing, and the patient was asked to return to the clinic sooner if he noticed any changes in his signs or symptoms.
Discussion
Open-globe injuries are not particularly common, occurring in up to five of 100,000 people per year.1,2 Younger males between the ages of 10 and 30 tend to be the population most at risk.1,2 Worksite hazards can increase the chances of an open globe injury.2 The two most common mechanisms that lead to this type of injury include being struck by another individual or an object, followed by a sharp foreign body piercing the eye.1
Upon initial evaluation of these patients, a detailed history should be taken to figure out the nature of the incident and possible worker’s compensation paperwork. It is good to know what type of object injured the eye, what speed it was traveling and what environment the patient was in at the time of injury.2 The environment is essential to know to help predict the chances and nature of possible infection.2 If the patient reports the involvement of a sharp object, a fast-moving object or blunt force trauma, this should raise immediate suspicion.2
In all emergent cases, it is vital to establish a baseline visual acuity to denote damage acquired and determine possible visual recovery.2,3 With suspected open globes, the eye should be manipulated as little as possible with intraocular pressure measurement and eyelid eversion excluded from the work-up.2,3 This precaution decreases the risk of any intraocular material being expelled from the eye.2
Pupils should be tested to discern any irregularities that may be present.2,3 A peaked pupil is a strong indicator that the patient has undergone an open-globe injury due to the pupil being pulled toward the wound.2 A comprehensive slit lamp examination should be performed to look for any remnants of the inflicting foreign body and potential lacerations or penetration sites.2 If there is any question as to the depth of a wound, Seidel testing should be performed.2,3
The anterior chamber should be assessed for adequate depth, presence of hyphema, cells, flare or any vitreous material.2 With ocular trauma, evaluating the integrity and positioning of the lens becomes important due to the possibility of dislocation.2 With any possible ruptured globe, be sure to rule out hemorrhaging, retinal detachment and possible intraocular foreign bodies.2 If an exam is not obtainable at the slit lamp, non-contrast computed tomography is the imaging of choice for open globe injuries, especially in the case of metallic foreign body involvement.2,3
A Farewell From Dr. ManganHow time flies. After a 30-year career in medical optometry, I finally get to take a few minutes to reflect on my time as an author and board member for Review of Optometry. It’s hard to believe that it’s coming to a close. What a pleasure it has been to collaborate with so many amazing professionals. I’m honored to have served as a columnist for Review for six years. When we first discussed the topic of ocular urgencies and emergencies as a potential column idea, we felt that we might be able to find enough interesting cases to support such a column for maybe three years. I never imagined that the column would still be going strong all these years later, and I’m thrilled to announce that Alison Bozung, OD, a rising star from Bascom Palmer Eye Institute, will be taking over—and taking it to new heights. There are so many people to thank: First, Editor-in-Chief Jack Persico. Thank you for giving me the opportunity to take on this very important topic for Review. Your support over the years is so appreciated. I couldn’t have done it without you! Second, the amazing editorial staff I have had the pleasure of working with for so many years. You are the true artists behind the scenes that make the articles and case presentations come to life! Third, all of the amazing optometric physicians who have contributed to the column. You have made a tremendous impact in strengthening our ability to understand and manage ocular urgencies and emergencies as they present. Lastly, and most importantly, you, my colleagues who have shown that this is a topic that still resonates. Thank you for being loyal readers of my column and Review.
Signing off, Rich |
When a patient needs to be referred for an open-globe repair, it is crucial to educate them not to eat or drink anything prior to anesthesia, to prevent a delay in care.2,3 Placing a patch over the affected eye could be considered for protection prior to surgical intervention.3 Positioning of the patient to avoid bending and lifting is important as well to limit intraocular pressure elevation.2,3
One of the most devastating complications that can result from an open globe, besides potential vision loss, is endophthalmitis.2-4 Because the intraocular contents are exposed, the rate of endophthalmitis is around 6.8%.2,4 Patients at a higher risk for developing this complication include those who delayed seeking care, who had a lens capsule rupture during the time of injury or who had a wound inflicted with an unsanitary foreign body.3 Getting the wound repaired as soon as possible, preferably within 24 hours, and initiating prophylactic coverage with a broad-spectrum antibiotic is the best prevention.2
Following surgery, the patient should be advised to wear a protective shield while sleeping.2 Restrictions post-globe repair typically include limiting excessive movement such as exercise and extensive lifting, along with no swimming.2 These restrictions are put in place to prevent wound dehiscence and to decrease the chance of infection.2 The best preventative advice to offer is that proper eyewear protection is of the utmost importance to guard the precious gift of sight.
Dr. Walton graduated with honors from the Indiana University School of Optometry. She completed her residency at Vance Thompson Vision in Sioux Falls, SD, managing ocular disease, refractive cases and pre- and post-op ocular surgery. She currently works at Vance Thompson Vision in Omaha, NE. She has no financial interests to disclose.
Dr. Mangan is a board-certified consultative optometrist from Boulder, CO, and a fellow of the American Academy of Optometry. He is an assistant professor in the department of ophthalmology at the University of Colorado School of Medicine. His focus is on ocular disease and surgical comanagement. He has no financial interests to disclose.
1. Mir TA, Canner JK, Zafar S, et al. Characteristics of open globe injuries in the United States from 2006 to 2014. JAMA Ophthalmology. 2020;138(3):268-75. 2. Wang D, Deobhakta A. Open globe injury: assessment and preoperative management. AAO. August 2020. www.aao.org/eyenet/article/open-globe-injury. Accessed September 29, 2021. 3. Blair K, Alhadi SA, Czyz CN. Globe rupture. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2020. 4. Essex RW, Yi Q, Charles PG, et al. Post-traumatic endophthalmitis. Ophthalmology. 2004;111(11):2015-22. |

