 A 42-year-old Hispanic female presented with significant blur at near. She said that her distance vision was mildly blurry as well. Her last eye exam was more than five years ago. She said that her previous eye doctor had noted the presence of “something unusual” in her right eye at a previous examination. Her medical history was unremarkable, and she did not take any medications.
A 42-year-old Hispanic female presented with significant blur at near. She said that her distance vision was mildly blurry as well. Her last eye exam was more than five years ago. She said that her previous eye doctor had noted the presence of “something unusual” in her right eye at a previous examination. Her medical history was unremarkable, and she did not take any medications.
Her best-corrected visual acuity measured 20/20 O.S., with a slight astigmatic correction. Confrontation visual fields were marginally depressed in her right eye, but full to careful finger counting in her left eye. Pupils were equally round and reactive, with a 1+ afferent defect in her right eye. Ocular motility testing was normal in both eyes. The anterior segment examination of both eyes was unremarkable. Her intraocular pressure measured 14mm Hg O.U.
Dilated fundus exam of her right eye revealed a clear vitreous as well as the obvious changes seen in figure 1. We ordered an optical coherence tomography scan (figure 2).
In her left eye, she had a small cup with good rim coloration and perfusion. Additionally, the vessels, macula and periphery were normal.
2. An SD-OCT scan through the macula and over the lesion in our patient’s right eye. What does it reveal?
Take the Retina Quiz
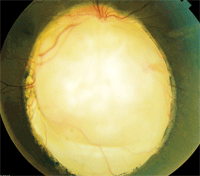
1. Our patient’s right eye exhibits a prominent white lesion.

1. Based upon this information, what would you predict the visual acuity in her right eye to measure?
a. 20/20 to 20/25.
b. 20/50 to 20/200.
c. Around 20/400.
d. Hand motion to light perception only.
2. What is the etiology?
a. Congenital.
b. Infectious.
c. Inflammatory.
d. Traumatic.
3. How would you describe the OCT findings over the lesion?
a. Normal.
b. Retinal thickening.
c. Absent.
d. Cystoid macular edema (CME).
4. What is the correct diagnosis?
a. Retinochoroidal coloboma involving the optic nerve.
b. Retinochoroidal calcification.
c. Toxoplasmosis chorioretinal scar.
d. Amelanotic choroidal melanoma.
5. What ocular complication is she at highest risk for?
a. Glaucoma.
b. Retinal detachment.
c. Metastasis.
d. Eye rot.
For answers, see below.
Discussion
Our patient has a large retinochoroidal coloboma with optic nerve involvement. It appears as a large, white staphylomatous depression; only the sclera is visible, because the retina, retinal pigment epithelium (RPE) and choroid are absent.
On clinical observation, the staphylomatous depression is difficult to appreciate. But, on Heidelberg Spectralis 3-D OCT (Heidelberg Engineering), the defect is seen very clearly. The OCT cross-sectional scan of the retina adjacent to the coloboma is normal; however, as the scan moves over the coloboma, the retina and RPE anatomy can be seen diving into the colobomatous depression.
A coloboma is a congenital defect that results from a failure of an embryonic fissure to close during the fifth week of development.1 It can affect multiple layers of the eye, including the iris, lens, optic nerve, RPE and choroid. Retinochoroidal colobomas most often occur inferiorly (in rare instances, they may be present in other locations of the retina). They may be isolated or involve all or parts of the optic nerve, as seen in our patient. Also, retinochoroidal colobomas may present either unilaterally or bilaterally.
The visual prognosis is dependent upon the coloboma’s extent and location. If there is no macular involvement, the patient’s visual acuity may be as good as 20/20 or 20/25. But, severe cases may result in microphthalmia.1 Retinal detachment, likely secondary to vitreoretinal traction along the edges of the coloboma, has been reported in up to 40% of affected patients.1-3 Choroidal neovascularization has also been reported.3 Due to an absence of the retinal layers, an absolute visual field defect will be present in a location consistent with the coloboma. In this case, our patient had a dense superior altitudinal defect.
There are several chromosomal syndromes associated with colobomas.4 The most notable is CHARGE syndrome (colobomas, heart defects, choanal atresia, retardation of growth and ear abnormalities), which should be suspected in the presence of bilateral colobomas.4
Other than the retinochoroidal coloboma with optic nerve involvement, our patient’s ocular health was normal. Given the dramatic appearance of this lesion, it is understandable that she drew a lot of attention from other doctors who were examining her. We explained the risk of retinal detachment to her and made her aware of the signs and symptoms. We gave her a prescription for glasses to minimize the blur and asked her to return for follow-up in one year.
Retina Quiz Answers: 1) a; 2) a; 3) c; 4) a; 5) b.
1. Onwochei BC, Simon JW, Bateman JB, et al. Ocular colobomata. Surv Ophthalmol. 2000 Nov-Dec;45(3):175-94.
2. Gallemore RP, McCuen BW. Silicone Oil in Vitreoretinal Surgery. In Ryan SJ (ed.). Retina, vol. III––Surgical Retina, 4th ed. St. Louis: Mosby, 2006; 2111-234.
3. Leff SR, Britton WA Jr, Brown GC, et al. Retinochoroidal coloboma associated with subretinal neovascularization. Retina. 1985 Summer-Fall;5(3):154-6.
4. Russell-Eggitt IM, Blake KD, Taylor DS, Wyse RK. The eye in the CHARGE association. Br J Ophthalmol. 1990 Jul;74(7):421-6.

