 |
|
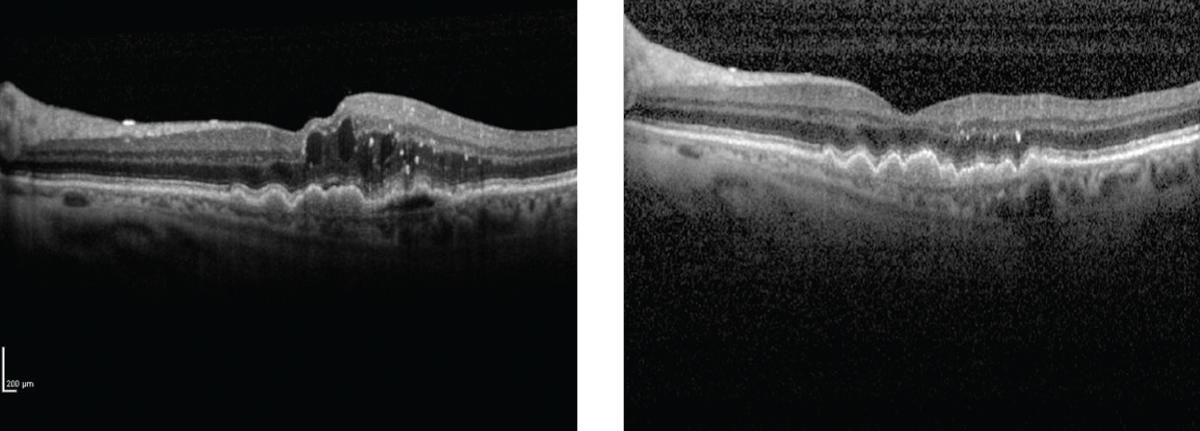
This study found that not every wet AMD patient needs multiple injections, as lack of continued therapy had no significant impact on outcomes. This photo shows a patient before and after treatment. Photo: Anat Loewenstein, MD. Click image to enlarge. |
Developing new injection schedules for patients receiving anti-VEGF agents is always on physicians’ minds due to the high costs of injections, the intense follow-up schedules, the psychological and physical impacts of these schedules and the threat of geographic atrophy. According to real-life analyses, treatment protocols and agent choices vary widely. More studies suggest that individualized treatment is best for wet AMD patients when taking into account treatment costs and scheduling. A new analysis published in Retina examined treatment-naïve wet AMD patients who received a single injection of ranibizumab/aflibercept and reported that a subset of these patients demonstrated resolution of choroidal neovascular membrane-associated exudation with a single injection that lasted more than two years.
The retrospective, observational study included 63 patients with wet AMD who achieved complete resolution of retinal exudation with a single injection. The researchers defined complete resolution as the total disappearance of intraretinal fluid, cysts and subretinal fluid, as well as a return to a retinal thickness <250µm on SD-OCT. Follow-up visits occurred on days one, seven and 30, postoperatively and then monthly. Patients had nine mandatory visits per year if the macula remained fluid-free.
The patients’ mean baseline and final-corrected distance VA was 20/160 and 20/45, respectively. They completed an average of 10.9 follow-up visits per year. They also noted that smaller choroidal neovascular membranes (<200µm), early presentation, better presenting corrected distance VA, subfoveal choroidal neovascular membranes, absence of blood/fibrosis and use of aflibercept (2mg) were factors associated with resolution after one injection.
Overall, the researchers said that a defined subset of patients receiving just one injection had “very good” visual and anatomical outcomes. These patients showed complete resolution of the neovascular membrane, and only seven required multiple injections after a treatment-free interval of at least 24 months. They noted no adverse events during follow-up.
Of the patients, 63% demonstrated a 15-letter gain and 47% were able to maintain a 10-letter gain at the end of follow-up (at least three years). “A lack of continued therapy didn’t adversely affect the final visual outcome,” the researchers noted. “The three patients who lost vision demonstrated macular atrophy on SD-OCT—probably a consequence of the natural progression of the disease. Overall, the gains noted in the first months after the injection were reduced by the end of the follow-up period; this reflects a continuing degenerative process in all probability, even if there’s no recurrence of the neovascular membrane.”
The researchers say these results are important, as real-life treatment often has different outcomes than clinical trials. “The purpose of the study is not to challenge established treatment protocols but to call for more flexibility in their execution in the real-life scenario and provide thought for future studies that look at larger numbers (modified PRN from baseline),” they explained. “The study underscores the fact that more than 10% of wet AMD may not need multiple injections. This can be vital in reducing costs in developing countries with rudimentary insurance systems or ‘copay’ systems and avoid procedure-related complications. Limited therapy might be an option in select patients without compromising on visual gain.”
Bilgic A, Kodjikian L, Mathis T, et al. Single injection response to antivascular endothelial growth factor agents in patients with wet age-related macular degeneration: incidence and characteristics. Retina. 2021;41:1901-10. |

