
I have a patient who has herpes zoster. Is there anything new to prevent or treat this painful condition?
In May, the FDA approved a new vaccine, Zostavax (live attenuated zoster vaccine, Merck) to prevent herpes zoster (shingles). The vaccine is approved for adults ages 60 and older who have had chickenpox but have not yet had shingles.
Nearly 1 million Americans develop herpes zoster each year, primarily those ages 50 and older, according to the Varicella Zoster Virus (VZV) Research Foundation.
The vaccine isnt a home run, because it doesnt prevent herpes zoster in 100% of cases and its effectiveness lessens with increasing age, says Louis R. Gary, chairman of the board of VZV Research Foundation. But it is a solid double, he says, because it reduces the chance of developing herpes zoster or, in patients who do develop shingles, it reduces the severity.
Specifically, the Shingles Prevention Study, which enrolled more than 38,000 adults ages 60 and older, found that Zostavax:1
Reduced the incidence of herpes zoster by 51.3%.
Reduced the severity of herpes zoster by 61.1%.
Reduced the incidence of post-herpetic neuralgia by 66.5%.
Unlike other vaccines that prevent infection, Zostavax is administered to people who have already been infected in the form of childhood chickenpox. The purpose of this vaccine is to boost their immunity to prevent it from coming back as shingles, says Stephen Tyring, M.D., professor of dermatology at the University of Texas Health Sciences Center at Houston. Dr. Tyring was one of the clinical investigators of the vaccine.
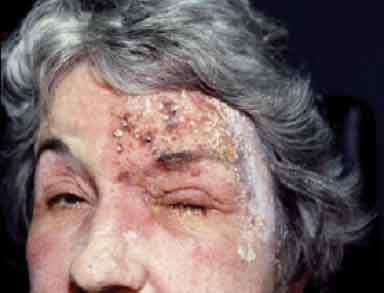 |
| This patients herpes zoster was first mistakenly treated as poison ivy. |
Because the vaccine is not yet covered by most insurance plans, patients must pay for it outright (cost: $220). But the cost and pain involved in a subcutaneous injection is much less than the cost and pain involved in treating shingles, Dr. Tyring says. The pain of shingles is terribly severe and can go on for months and sometimes years. In the case of [herpes zoster] ophthalmicus, it can result in blindness. The pain of a shot is mild and over almost instantaneously, he says.
On October 25, the Centers for Disease Control and Prevention is scheduled to consider recommending the vaccine and will review Medicare coverage for it.
Refer interested and appropriate patients to a knowledgeable general practitioner or dermatologist for the vaccine.
For treatment, would you start the patient on acyclovir and manage the patient yourself or comanage with a dermatologist?
Send the patient to a dermatologist for at least one visit, in case the patient should develop complications down the road. Unless the patient has painful post-herpetic neuralgia, you can manage the rest of herpes zoster treatment, says optometrist Randall Thomas, of Concord, N.C.
For treatment, there are other options besides generic acyclovir tablets, which involve a more onerous regimen for the patient: 800mg five times a day for a week, Dr. Thomas says. The two other oral antivirals, Valtrex (valacyclovir, GlaxoSmithKline) and Famvir (famciclovir, Novartis), are administered three times a day at 1,000mg and 500mg respectively, and are equally effective as acyclovir. So if a person has a drug plan, Ill prescribe Valtrex or Famvir because these drugs only have to be taken three times a day. But if finances are a concern for the patient, Ill prescribe the generic acyclovir, which is much less expensive, he says.
The typical teaching is you have to start the antiviral within the first three days [that shingles develop], Dr. Thomas says. Its not like the medicines become worthless after three days. But the sooner you can start these antiviral medicines when a person develops shingles, then the more positive clinical impact they will have.
The eye becomes involved and inflamed in about half of all cases of ophthalmic division shingles.2 This almost always manifests as keratitis or uveitis. In either case, prescribe a potent corticosteroid such as Lotemax (loteprednol, Bausch & Lomb) or Pred Forte (prednisolone acetate, Allergan), Dr. Thomas says. For severe cases, have the patient administer the drug every two hours until the inflammatory expression comes under control, then taper over a couple of weeks. For less severe cases, prescribe it four times a day for a week, then taper.
Occasionally, a patient will manifest post-herpetic neuralgia after successful treatment of shingles. (Patients younger than 60 have less than 2% risk; patients older than 60 have less than 7% risk. This risk rises as age increases.3) Refer the patient to a dermatologist or good primary-care physician to manage the pain, Dr. Thomas says. The O.D. doesnt need to see the patient again for post-herpetic neuralgia if the herpes zoster has resolved.
Usually, combination therapyincluding analgesics, low-dose tricyclic antidepressants, anticonvulsants or even narcoticsis used indefinitely until the neuralgia subsides, Dr. Tyring says. (Two anticonvulsants, Neurontin [gabapentin, Pfizer] and Lyrica [pregabalin, Pfizer] are specifically approved for post-herpetic neuralgia.) During this time, which could last from months to years, the physician usually sees the patient monthly.
1. Oxman MN, Levin MJ, Johnson GR, et. al.; Shingles Prevention Study Group. A vaccine to prevent herpes zoster and postherpetic neuralgia in older adults. N Engl J Med 2005 Jun 2;352(22):2271-84.
2. Pavan-Langston D. Herpes zoster ophthalmicus. Neurology 1995 Dec;45(12 Suppl 8):S50-1.
3. Helgason S, Petursson G, Gudmundsson S, Sigurdsson JA. Prevalence of postherpetic neuralgia after a first episode of herpes zoster: prospective study with long term follow up. BMJ 2000 Sep 30;321(7264):794-6.

