
|

|
TA suspects should have an immediate work up, including pupil assessment, color vision, dilated exam and blood work (CBC w/differential, ESR and CRP). The CBC can rule out other causes of inflammation (e.g., infection, anemia, leukocytosis) and/or may yield the diagnosis due to elevated platelet levels. If the ESR is elevated, refer for a temporal artery biopsy to conclusively diagnose TA. Also consider biopsy if the ESR is normal and the CRP is high, along with associated clinical findings—a small number of cases do not manifest elevated ESR. The biopsy should be performed by a neurologist or neuro-ophthalmologist within one week after starting systemic steroids. A biopsy is especially important in diabetics because corticosteroids have relative contraindications.
The procedure is typically performed in a minor operating room. After topical and injectable anesthesia, the superficial temporal artery is marked by palpating the pulse or using a Doppler ultrasound, followed by antisepsis and draping. Using a #15 blade, an incision is made directly over the artery, penetrating only skin and subcutaneous tissue to avoid injuring the underlying vessel. Further dissection with a hemostat is carried out into the superficial temporal fascia, where the temporal artery is found.
Hemostats with electrocautery are used to minimize hematoma risk. The vessel is clamped, exposing a 2cm-to-5cm length of the artery. The two ends of the artery are tied with suture and the intervening segment is removed and sent to pathology, where it is checked for both acute inflammation and disruption of the internal elastic lamina (indicating healed chronic inflammation). Once adequate hemostasis is ensured, the subcutaneous tissue is closed, followed by the superficial wound, which is dressed with petroleum ointment for several days until sutures dissolve.
Multimedia
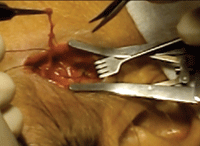
Click
here to view a narrated video of a temporal arterial biopsy.
Photo and video courtesy of ocuplastics surgeon Thomas Joly, MD, PhD
Potential risks and complications include hematoma, incisional alopecia, nerve damage, scar formation and wound infection. Negative results from the biopsy (likely due to small sample size) may necessitate an additional biopsy to the opposite artery.
Once TA is diagnosed, systemic steroids are required to preserve vision; untreated, it can progress to bilateral vision loss. Start steroids immediately, either intravenously (methylprednisolone 250mg IV, Q6H for 12 doses) or orally (prednisone 80mg to 100mg PO, QD). Patients will continue prednisone for six to 12 months, depending on the ESR levels and disease suppression. Antiulcer meds are often given along with systemic steroids to manage GI issues.
Patient education is of the utmost importance, due to the potentially visually devastating consequences. Let your patient know that you will call them with the results and communicate your findings with the consulting physician and their primary care doctor. In cases of high suspicion or abnormal lab findings, a TA biopsy will confirm or rule out the diagnosis.

