 History
History
A 35-year-old black man presented for a routine examination. He wanted to know what the white lumps on the clear part of his eye were. His systemic history was noncontributory. He was in good health and reported no allergies.
Diagnostic Data
His best-corrected visual acuity was 20/20 O.U. at distance and near. External examination was normal and there was no evidence of afferent pupillary defect. The pertinent anterior segment findings are illustrated in the photograph. His intraocular pressure measured 19mm Hg in both eyes. The dilated fundus findings were normal O.U. Additional examination included sodium fluorescein testing to evaluate corneal integrity, and a corneal sensitivity sweep.
Your Diagnosis
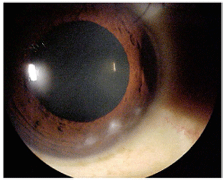
The right eye of a 35-year-old man who presented with "white lumps" on his cornea. What would you diagnose?
How would you approach this case? Does this case require any additional tests? What is your diagnosis? How would you manage this patient? What is the likely prognosis?
The Diagnosis
The diagnosis in this case is Salzmanns corneal degeneration. This unusual degenerative condition may occur at any age; yet, it primarily affects the elderly.1-3 It typically develops in individuals with a history of previous keratitis, often presenting several decades after the initial incidence.1-4
Salzmanns corneal degeneration has been specifically associated with previous bouts of phlyctenular keratitis, but may also follow interstitial keratitis, vernal keratitis, trachoma or Thygeson"s superficial punctate keratitis.4 The condition may also be found in individuals with no prior history of corneal disease. It may be unilateral or bilateral, and occurs more often in women than in men.1-3 Additional examinations for Salzmanns corneal degeneration may include sodium flourescein staining, corneal sensitivity testing and an extended patient history analysis.
Salzmann"s corneal degeneration is characterized by the presence of white-to-gray or light blue nodules that elevate the epithelium in the superficial corneal stroma.1-4 They may appear singly or as clusters in a circular array, often at the edge of old corneal scars. Each nodule is about 0.5mm to 2mm in diameter, separated from other nodules by clear cornea. Typically, there is no vascularization.1-4 An epithelial iron line may surround the base of the lesion. The lesions develop gradually over many years, during which time they increase in both size and number. They may inhibit the patients vision as they encroach upon the central cornea or alter the corneal shape.4 Also, Salzmann"s degeneration may be associated with recurrent corneal erosions.1-3,5
Histological examination of excised nodules will typically show thinned epithelium overlying hyalinized avascular collagen.1 Bowman"s membrane is often damaged or focally absent, replaced by material that is similar to basement membrane. Usually, evidence of old keratitis is seen in the surrounding stroma.4,5
Patients with peripheral Salzmann"s nodules are asymptomatic and require no treatment. If vision is altered or if recurrent erosions are frequent, the patient may either be fit with a rigid gas-permeable scleral contact lens or undergo surgical removal of the nodules. Removal of the nodules is often accomplished by peeling them from the underlying stroma after a plane has developed from scraping around the edge of the lesion, or by Excimer laser phototherapeutic keratectomy.4 Lamellar or penetrating keratoplasty may be used to remove the nodules as well. Recurrences have been reported after all forms of treatment.1-3
This patient was asymptomatic, despite recognizing that something was airy. Therefore, exempting appropriate education and lubrication, no additional treatment was initiated. We scheduled a follow-up examination in six months, or again as needed.
1. Sugar A. Conjunctival and corneal degenerations; Salzmanns corneal degeneration. In: Yanoff M, Duker JS (eds.): Ophthalmology.
2. Biswas S, Brahma A, Tromans C, Ridgway A. Management of pellucid marginal corneal degeneration. Eye 2000 Aug;14(Pt 4):629-34.
3. Romero-Rangel T, Stavrou P, Cotter J, et al. Gas-permeable scleral contact lens therapy in ocular surface disease. Am J Ophthalmol 2000 Jul;130(1):25-32.
4. Das S, Link B, Seitz B. Salzmann"s nodular degeneration of the cornea: a review and case series. Cornea 2005;24(7):772-7.
5. Ramamurthi S, Rahman MQ, Dutton GN, et al. Pathogenesis, clinical features and management of recurrent corneal erosions. Eye 2007;21(3):439-40.

