A 54-year-old Hispanic female presented with complaints of reduced visual acuity in her right eye. More specifically, she reported that the vision in her right eye had been poor for about 12 years; however, she noted a further, painless, progressive decrease during the last three months.

Indeed, a review of her medical records indicated that her visual acuity measured 20/60 O.D. when she was last seen nearly five years ago. At this exam, however, her visual acuity measured just 20/400 O.D. (Her left eye measured 20/20.)
Additional clinical testing revealed full to careful finger counting confrontation visual fields O.U. Both pupils were equally round and reactive, with no afferent defect. The anterior segment was normal O.U. Her intraocular pressure measured 17mm Hg O.U.
Dilated fundus exam of the right eye exhibited the changes seen in figure 1. Her left eye, however, was completely normal. We also took a spectral domain optical coherence tomography (SD-OCT) scan of her right eye (figure 2). Finally, a fundus photograph of her right eye from her initial exam 12 years ago was available for comparison (figure 3).
Take the Retina Quiz
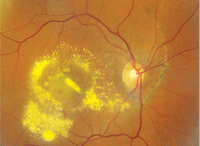
1. A montage view of our patient’s right macula and posterior pole when she presented at her latest visit.
1. How would you classify the changes that were seen in her right eye 12 years ago?
a. Infectious.
b. Congenital.
c. Degenerative.
d. Traumatic.
2. What does the circumferential linear line that is seen in the fundus photograph from 12 years ago represent?
a. Angioid streaks.
b. Laqueor cracks.
c. Choroidal rupture.
d. Larvae or worm tracks.
3. What is the explanation for her reduced acuity at this examination?
a. Choroidal neovascularization (CNV).
b. Branch retinal vein occlusion (BRVO).
c. Retinal telangiectasia.
d. Retinal macroaneurism.
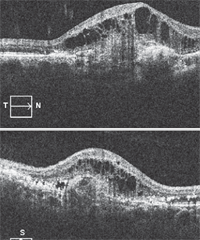
2. A spectral domain OTC through our patient’s right macula. What does it show?
4. What does the SD-OCT show?
a. Chorioretinal scarring.
b. Retinal detachment.
c. Cystoid macular edema (CME) with chorodial neovascularization (CNV).
d. CME with retinal pigment epithelial detachment (PED).
5. How should this patient be managed?
a. Observation.
b. Argon laser photocoagulation.
c. Intravitreal anti-VEGF therapy.
d. Antihelminthic medications (i.e., thiabendazol).
Retina Quiz Answers: 1) d; 2) c; 3) a; 4) c; 5) c.
Discussion
Our patient initially presented 12 years ago after having fallen down a flight of stairs, which resulted in direct trauma to her right eye as well as a concussion. She was seen in the ER at the Bascom Palmer Eye Institute within a few days after the fall, and an ophthalmic examination revealed a large choroidal rupture. The choroidal rupture begins superiorly and extends inferiorly nasal to the optic nerve, where it makes a circumferential turn and bisects the macula. Subretinal hemorrhage can be seen within the choroidal rupture in addition to choroidal folds and retinal striae that extend both above and below her fovea.
Choroidal ruptures develop as a result of mechanical compression to the globe that is followed by sudden hyperextension due to blunt trauma. Bruch’s membrane does not have enough elasticity to withstand the compressive force that can occur from the blunt trauma, so it often ruptures. Such ruptures tend to be radial and often temporal to the macula.
In our patient, the choroidal rupture is much larger than what is typically seen. Clearly, the right eye must have suffered a direct blow from the fall to yield such an
extensive choroidal rupture.
She did recover from the fall and was seen periodically over the years; however, her vision never improved beyond 20/60 due to the scarring that developed in the macula secondary to the choroidal rupture. More recently, her vision had decreased significantly because she developed a CNV at the sight of the choroidal rupture, which resulted in massive leakage and exudation in her macula and posterior pole. The OCT shows an elevated and thickened macula with extensive CME. Directly below the CME, we noted a homogenous area of higher reflectivity, which represents the CNV.
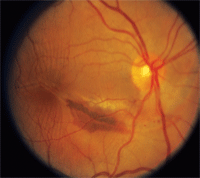
3. A fundus photograph of our patient’s right eye when she initially presented 12 years ago. What changes do you notice?
CNV is a common secondary complication of choroidal ruptures. Much like what is seen with laqueor cracks in high myopia and angioid streaks with pseudoxanthoma elasticum (PXE), CNV can develop and grow through these cracks or defects within Bruch’s membrane and the RPE, where they will eventually leak and bleed, resulting in further scarring (if left untreated).
Our patient underwent two intravitreal injections of Avastin (bevacizumab, Genentech) before being lost to follow-up. At the last exam, her visual acuity improved to 20/100 O.D., and much of the exudate had resolved. However, we still noted considerable retinal thickening and macular edema.

