A 31-year-old black female presented emergently with complaints of visual blur and poor focus in her left eye that began three days earlier. Since initial onset, she noticed a rapid, painless, progressive loss of vision in that eye. Her only other symptom was flashes of light OS.
 |
Her medical history was significant for an episode of bronchitis with sinusitis a few weeks ago. She was prescribed a medication, but never went to the pharmacy to have it filled.
Her ocular history included a painful, red eye OS one year earlier, which was believed to be caused by either scleritis or episcleritis. The presentation quickly resolved with topical steroid eye drops and oral NSAIDs.
On examination, best-corrected visual acuity measured 20/20 OD and hand motion (HM) OS. Ocular motility and cover testing were normal. Confrontation visual fields were full to careful finger counting OD, but HM only OS. Pupils were equally round and reactive, with a trace of afferent defect in the left eye. The anterior segments were unremarkable OU.
Dilated fundus exam of the right eye showed a clear vitreous and normal optic nerves, with good rim coloration and perfusion. The remainder of the right eye appeared completely normal.
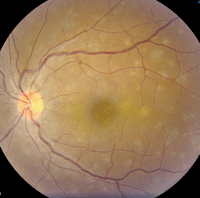
In the left eye, we documented trace vitreous cells and a central macular lesion that appeared granular in nature and consisted of multiple white dots. Similar lesions were scattered throughout the posterior pole (figure 1). We performed a spectral-domain optical coherence tomography (SD-OCT) scan (figure 2), as well as fluorescein and indocyanine green (ICG) angiographies (figure 3).
 |
|
|
1. Fundus images of our patient's left eye. Note the presence of spots throughout the posterior pole.
|
Take the Retina Quiz
1. What is the most likely location of these white lesions?
a. Inner retina.
b. Photoreceptors.
c. Outer retina and retinal pigment epithelium (RPE).
d. Choroid.
2. What is the correct diagnosis?
a. Acute posterior multifocal placoid pigment epitheliopathy (APMPPE).
b. Acute macular neuroretinopathy (AMN).
c. Multiple evanescent white dot syndrome (MEWDS).
d. Diffuse unilateral subacute neuroretinitis (DUSN).
3. How are patients with this condition typically managed?
a. Observation.
b. Oral antibiotics.
c. Anthelmintic drugs (e.g., thiabendazole).
d. Laser photocoagulation.
4. What is the likely clinical course?
a. Progressive, with total vision loss.
b. Chronic and recurrent, with central vision loss.
c. Episodic recurrences, with generally good vision.
d. Self-limiting, with good recovery of central vision.
5. What does the SD-OCT show?
a. Choroidal neovascularization (CNV).
b. Photoreceptor toxicity.
c. Disruption of the outer retinal layers at the level of the inner/outer segment junction.
d. RPE atrophy.
For answers, see the bottom of this article.
Discussion
Our patient has multiple evanescent white dot syndrome (MEWDS). The condition was originally described in 1983 as an acute, unilateral, multifocal retinopathy that affects young adults.1 Approximately 75% of MEWDS cases are documented in females.1
|
2. An SD-OCT scan through patient's left macula. What does it reveal?
|
Nearly half of the patients diagnosed with MEWDS report a preceding flu-like illness or viral infection.1 Interestingly, our patient experienced a bout of bronchitis/sinusitis a few weeks prior to developing ocular symptoms.
The typical age of onset ranges from 14 to 57 years.1 Patients often complain of visual blur, as well as photopsia or flashing lights. Patients also may complain of a temporal scotoma, which will manifest as an enlarged blind spot on visual field testing. This enlarged blind spot has been termed acute idiopathic blind spot enlargement (AIBSE) syndrome, which may be located on the spectrum of MEWDS and other similar conditions, such as acute zonal occult outer retinopathy (AZOOR) and acute macular neuroretinitis (AMN).1
The clinical findings associated with MEWDS include multifocal gray-white patches comprised of small, white dots that are largely concentrated in the paramacular area, at the level of the deep retina or the RPE. Affected individuals also exhibit a granular macular appearance, with tiny, yellow or orange dots in the center of the fovea. This presentation often results in IS/OS disruption, as was the case with our patient. The macular lesion is thought to be distinct from the larger white patches that are seen throughout the posterior pole and retina. Vitreous cells generally are present, as well.
The white patches and granular appearance in the macula will slowly fade over time and become less apparent. This can make the diagnosis even more challenging, depending on when the patient is evaluated. In our patient, the gray-white patches were clearly evident––but, in other cases, it may not be so obvious.
 |
|
|
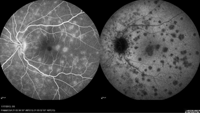
3. Late-stage FA (left) and ICG angiography (right) of her left eye.
|
Ancillary testing can be very helpful in confirming a diagnosis of MEWDS. On fluorescein angiography (FA), the gray-white patches will hyperfluoresce in a cluster or wreath-shaped pattern. Indocyanine green (ICG) angiography is perhaps the best diagnostic test for uncovering multiple hypofluorescent lesions. During the late phases of ICG angiography testing, these lesions will correspond to the white patches in the posterior pole. Take note that ICG angiography will show many more spots than can be seen on clinical examination alone.
The etiology of MEWDS is unknown. Some researchers believe it is caused by an underlying viral illness, but tests for herpes zoster, herpes simplex, mumps and measles have been inconclusive.1 MEWDS is self-limiting, so no treatment is recommended. The patient’s vision will improve over the course of several weeks, with gradual resolution of the retinal lesions.
Because our patient demonstrated such profound vision loss, we started her on 30mg of oral prednisone. Her vision improved to 20/40 OS at the six-week follow-up, with complete resolution of the spots. Further, SD-OCT showed no disruption of the IS/OS junction––so we instructed her to discontinue oral prednisone use.
One year later, her visual acuity measured 20/25 OS.
1.Mirza RG, Jampol LM. White Spot Syndromes and Related Diseases.. Retina, Vol. II––Medical retina, 5th ed. St. Louis: Mosby; 2012:1164-8.

