No one walks into Starbucks and says, “Give me a cup of coffee.” You have to specify tall, grande or venti. You have to ask for room for cream or fill it up. Decaf or regular. Bold roast or medium. And that’s just for a cup of hot coffee—if you want iced coffee, espresso or a specialty drink, you’ll need to request a number of additional options. (Triple-grande-sugar-free-no-whip-extra-hot-cinnamon-dolce-latte, anyone?)

Before the patient steps foot into the surgeon’s practice or the surgery center, the optometrist should discuss the various options and give the patient a specific IOL recommendation to help the patient make a decision.
So, if you take that kind of trouble with your coffee, shouldn’t you take that kind of care with your cataract surgery patients—especially those interested in premium IOL technology?
Why? Because cataract surgery has changed. The days of sending the patient off to the surgeon and letting the surgery center take care of all the details are over.
On the bright side, getting more involved in the finer points of the cataract procedure is a great opportunity for optometrists—and a real help to patients.
How do you do it? Here are some specific tips for comanaging cataract patients who are interested in the option of a premium IOL.
1. You Make the Call
You know the patient best, so you make the call (in terms of the IOL options). Don’t just drop the patient in the surgeon’s lap.
“We get a few patients referred to our practice who haven’t been presented with all or even any of their IOL options, and the surgeon has to be the first one to break the news to them,” says Paul C. Ajamian, O.D., of Omni Eye Services of Atlanta, the nation’s most established comanagement center. “The patient’s question is naturally going to be, ‘Why didn’t my optometrist tell me about these things?’”
“O.D.s very often ask, ‘Which lens should we
recommend?’ It’s just not that easy,” Dr. Cunningham says. “Just like
there’s no one contact lens for everybody, there’s no single IOL that’s
going to be universally good for everybody.” For example, the accommodating Crystalens HD IOL (Bausch + Lomb)
provides exceptional and distortion-free distance and intermediate
vision, but patients may still require reading glasses for near vision. On the other hand, diffractive multifocal IOLs, such as AcrySof ReSTOR
(Alcon) and Tecnis (Abbott Medical Optics), are great for distance and
near vision, but are not optimal for intermediate distance and may cause
minor amounts of distortion. Again, this is an opportunity for the optometrist to provide key
information about the patient’s lifestyle and visual needs. For
instance, a patient who reads a lot of paperback novels may be a better
candidate for the ReSTOR, while a heavy computer user might be best
served with a Crystalens.
Well before the patient steps foot into the surgeon’s practice or the surgery center, the optometrist should not only discuss the various options with patients—whether a standard IOL or a premium one—but give the patient a specific recommendation and help the patient make a decision.
One Size Does Not Fit All
“Who knows more about the refractive status, eye health and complete eye care of the patient than the optometrist?” Dr. Ajamian asks. “So, in many cases, the final decision should be made between the patient and the optometrist, and then that decision should be communicated to the surgeon.”
Won’t the surgeon be offended by an optometrist who calls the shots?
Just the opposite, Dr. Ajamian says. “We love it when an O.D. sends us a patient and gives us the preferred visual parameters, because we don’t really know the patient’s ocular history. And we don’t know their lifestyle preferences, like whether they read books more than use the computer, or watch TV across the room.”
And, “if a surgeon ignores your advice, find another surgeon,” Dr. Ajamian states emphatically. Will patients be put off by your surgical recommendation?
Not at all, says Walter O. Whitley, O.D., of Virginia Eye Consultants, an ophthalmic surgery practice in Norfolk, Va.
“Go ahead and make a recommendation from the chair. We do it for glasses, contact lenses, AR coating, polarized lenses, progressive addition lenses—we need to do the same thing for IOL technology,” Dr. Whitley says. “And then, of course, make those preferences and your recommendation known to the surgeon.”
That is, write it down and send it to the surgeon. Don’t rely on the patient to convey the message.
2. Refer to Your Mom’s Surgeon
These are your patients, so not just any surgeon will do. Just as you give patients advice about specific IOLs, you must also advise them on who can implant it.


No one lens fits every patient’s needs. For instance, a patient who reads a lot of paperback novels may be a better candidate for the ReSTOR (left), while a heavy computer user might be best served with a Crystalens (right).
“Patients come to us for our professional opinion,” Dr. Whitley says. “They want to know who would we go to if we were getting cataract surgery. Or if our parents needed surgery, who would we refer them to?”
You need a go-to surgeon who is also your “phone-a-friend”—someone you trust, who you communicate well with, and who works well with optometry to maximize patient outcomes, Dr. Whitley says. So do your homework to find a good surgeon.
How? Take one for a test drive, Dr. Ajamian says.
“Ask a surgeon if you can spend a half a day in the O.R. with your own patients. Book three, four or five of your cataract patients for the same day, and then put on the scrubs and scrub in,” he says. “Patients eat it up. They love it. They’ll go out and tell 20 people that you assisted in their cataract surgery—which you did!”
“Laser cataract surgery is going to be
taking ‘refractive cataract surgery’ to the next level and increasing
the precision of premium IOL technology,” says Dr. Whitley, whose office
is one of only about a dozen centers in the country to have a LenSx
femtosecond laser (Alcon). “So far, we’ve been very impressed with the outcomes,” Dr. Whitley says. Indeed, ophthalmic surgeons presented promising findings at the recent
American Academy of Ophthalmology meeting in late October. Mark Packer,
M.D., of Oregon Health and Sciences University, noted that laser lens
fragmentation causes zero loss of corneal endothelial cells. William W. Culbertson, M.D., of the Bascom Palmer Eye Institute,
explained that using the laser to fragment the lens reduced the required
amount of ultrasound energy for phacoemulsification by 45%. In
addition, the laser makes a smaller, perfectly circular capsulorhexis.
In addition to being the best marketing that you don’t have to pay for, it also enables you truly see what happens on surgery day, so you’ll know exactly what to tell subsequent patients.
Laser Cataract Surgery
“But you’ll also learn the surgeon’s criteria and preferences for premium lenses, torics, etc. You’ll find out which lenses they use, and which they don’t,” Dr. Ajamian says. “Just as important, you’ll see firsthand what kind of surgeon they are—you’ll observe their temperament, meet their staff and see how patients are treated.”
If the surgeon uses one, and only one, type of IOL, discuss with your surgeon why he or she prefers one technology over another. Also, is the surgeon open to using the other IOL technologies? If not, keep searching. “Be very mindful of the surgeon who uses one product and one product only,” says Derek Cunningham, O.D., of Dell Laser Consultants, an ophthalmic surgery practice in Austin, Texas. “It shows that they may either not understand other technology or they may not be efficient with the other products.”
Successful comanagement is the result of continuous communication. If you feel strongly about a certain IOL for your patient, let your surgeon know.
Likewise, if the O.D. and the surgeon aren’t on the same page, then miscommunication will be the result, he says. And for these high-tech IOLs, there’s no room for error.
3. Clean Up the Ocular Surface
“Every eye you consider sending for surgery should have clean lids and a relatively normal ocular surface,” Dr. Ajamian says. “If they don’t, clean them up!”
Ocular surface disease can have a significant effect on the cornea and throw off the pre-op IOL measurements, Dr. Whitley says. So, dry eye, blepharitis, allergies—all of these common conditions must be addressed prior to multifocal IOL implantation to maximize patient outcomes. And you don’t want to send a cataract patient with dry eyes on a wild goose chase to the surgeon, who’ll either treat the surface or send the patient right back to you, which delays the surgery. This leaves the patient questioning why you didn’t bring it up beforehand. So, treat these patients aggressively to resolve these conditions preoperatively.
4. Pause for Pathology
As with ocular surface disease, any ocular pathology that affects vision is a contraindication for premium IOL implantation. (The only exception is a toric IOL for astigmatism.)
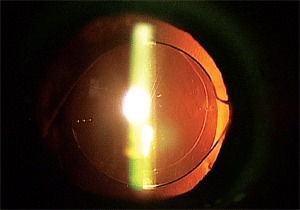
Cylinder can be a contraindication for a diffractive multifocal IOL. So perform topography to check for astigmatism. A toric IOL (seen here) could be a better option.
On the anterior segment, this includes pterygium, Salzmann’s nodules or anterior basement membrane dystrophy, Dr. Ajamian says. A chalazion on the eyelid can cause corneal cylinder, which will affect the final result of the IOL.
On the posterior segment, examples include epiretinal membrane, drusen or glaucoma—anything that affects contrast sensitivity, Dr. Whitley says.
5. Avoid Astigmatism
Another part of your preoperative evaluation: Perform topography to check for astigmatism. “You just don’t know how much corneal cylinder they have until you do topography,” Dr. Ajamian says. “Cylinder can be a contraindication for a multifocal IOL like the ReSTOR (Alcon), but you don’t know until you determine how much of it is corneal astigmatism and how much is lenticular.”
Although more than 1.00D of corneal astigmatism is generally contraindicated for a diffractive IOL, the patient can still be provided a premium toric IOL, he says, if the astigmatism is managed with incisional or laser procedures. On the horizon is a multifocal toric implant, which was recently approved in Europe (see “Coming Soon: Multifocal Toric IOL.”).
Irregular astigmatism, though, does not do well with a multifocal IOL, he adds.
6. Always Mention Glasses and Halos
You’ve heard it before: Set realistic patient expectations. But how do you specifically do that?
Dr. Cunningham informs all premium IOL patients about the shortcomings of the technology: “Nothing’s ever going to work as well as the natural accommodation system, but this is the best available technology at this time.”
You’ve also heard this before: Perfectionists and people with type-A personalities should not be recommended for these implants; they’ll never be satisfied. But even easygoing folks need to be given fair warning.
| Coming Soon: Multifocal Toric IOL |
|
There are two basic types of premium IOLs: those that correct for presbyopia and those that correct for astigmatism. But a newly developed IOL may combine the best of both types of IOLs, although it’s not yet approved in the United States. It’s the AcrySof IQ ReSTOR Multifocal Toric IOL (Alcon), and it was approved in Europe last year. The company has said that it plans to file a pre-market application with the FDA in early 2012 for possible U.S. approval. |
“Never say, ‘You’ll never have to wear glasses again,’” Dr. Whitley advises. “And even if you say, ‘This will reduce your dependency on glasses,’ what they really hear is, ‘You’ll never have to wear glasses again.’”
So, be sure to specifically tell them they may occasionally need a pair of glasses from time to time. For instance, “If you read for long periods of time or in dim illumination, then you may need a pair of reading glasses,” Dr. Whitley tells them.
Also, be sure to specifically discuss with patients their current cataract symptoms of glare and halos, and that they may continue to see halos at night post-surgically, but to a much lesser extent.
Dr. Whitley explains it to patients this way: “With any option that we choose, there’s a compromise—so the compromise for your improved quantity and quality of vision is that less than 5% of patients may see halos at night. But it’s more of an observation than a complication.” With such a warning ahead of time, patients may see halos postoperatively but usually won’t consider them bothersome.
Another word of advice to patients with a diffractive IOL: “Turn the lights up when you read, because brighter light will give you more of near power to see up close,” Dr. Whitley says.
7. ‘Touch Up’ Residual Error In case you were wondering, there’s very little correlation between a
multifocal contact lens and a multifocal IOL, Dr. Cunningham says. (The
main similarity, though, is the importance of patient selection and
willingness to accept some compromise to vision in exchange for the
reduced dependency on glasses.) So, generally speaking, there’s no point
to a multifocal contact lens trial for a potential multifocal IOL
patient. “Don’t even try it,” he says. “Multifocal contacts are hit and miss—some people accept them and some
don’t,” Dr. Cunningham says. “But multifocal IOLs are at the nodal point
of the eye, so they don’t require getting used to, like multifocal
contacts. They’re not the same thing at all.”
Don’t Bother with a Multifocal Contact Lens Trial
Postoperatively, “if the patient has residual myopia, hyperopia or astigmatism—in other words, if you put a trial lens in front of their eyes and they appreciate the overall improvement at most distances—they may be a candidate for a touch-up LASIK or touch-up PRK,” Dr. Whitley says. (The only exception is if the patient is already 20/Happy, he says.) With the advent of premium IOLs, “this is now considered refractive cataract surgery. So anything we can do to optimize their final results is our goal.”
8. Document the Details
If it’s not in the chart, then it was never performed or mentioned (at least for legal purposes). So document every test you run and every discussion you have, Dr. Ajamian says. Even for patients who say no to a premium IOL, protect yourself by writing that you gave them all their options and they denied the multifocal or toric IOL.
Also, for reimbursement purposes, putting this information in the chart corroborates that you earned your fees for specific, relevant services, he says.
Premium IOL implantation is “the fastest growing segment of all refractive eye care, and the patient base is exploding exponentially,” Dr. Cunningham says. “So if eye doctors don’t become familiar with this technology soon, they’ll be left behind.”

