|
|
History
A 47-year-old white female presented to the clinic and reported pain, photophobia and lacrimation, in both eyes, upon waking. Her ocular history was significant for previously diagnosed dry eye.
Diagnostic Data
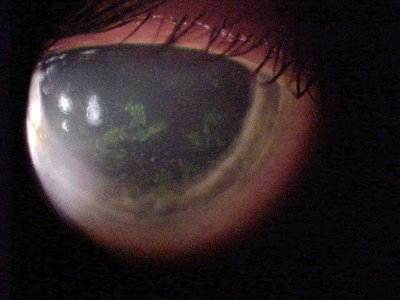
Her best-corrected acuities were 20/40 O.U. at distance and near. External examination findings were normal with no evidence of afferent pupillary defect. The pertinent anterior segment findings are illustrated in the photographs
 |
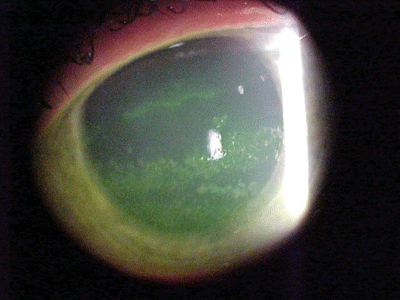 |
| A 47-year-old white female presented with this appearance O.D. (left) and O.S. (right). |
Goldmann intraocular pressures measured 14mm Hg in both eyes. Dilated funduscopy was within normal limits in both eyes.
Your Diagnosis
How would you approach this case? Does this patient require additional tests? What is your diagnosis? How would you manage this patient? What is the likely prognosis?
Discussion
The diagnosis in this issue is dry eye with bilateral recurrent corneal erosions.
To confirm this diagnosis, additional testing could include:
Schirmer tear test or the phenol red thread test to evaluate tear volume.
Tear quality analysis.
Sodium fluorescein, lissamine green and/or rose bengal dye tests to confirm and grade the corneal and conjunctival epitheliopathy.
Eyelid strength testing and blink analysis to rule out lagophthalmos secondary to floppy eyelid syndrome or cranial nerve VII palsy.
Additional history to rule out medications capable of causing dry eye.
Systemic laboratory investigations to rule out systemic etiologies.
Many collagen vascular diseases can result in unilateral or bilateral dry eye with noninfectious peripheral corneal inflammation. Rheumatoid arthritis (RA) and secondary Sjgren"s syndrome are probably the most common of these systemic diseases.1-6
Differential diagnosis in this case includes cicatricial pemphigoid, a rare disorder characterized by recurrent blisters or bullae of the skin and mucous membranes that result in scar formation. This disease occurs in older people (mean age of 70 years) and affects women more than men.1 The course of ocular involvement is asymmetrically bilateral and usually progressive. The pathogenesis of the disease is thought to be an autoimmune attack of immunoglobulins (mostly IgG) on the basement membrane of the conjunctiva.
Other differential diagnoses of dry eye include:
Radiation exposure.
Chemical exposure.
Severe atopic keratoconjunctivitis.
Scleroderma.
Erythema multiforme.
Trachoma.
Bechet"s disease.
Sarcoidosis.
Medications-such as systemic birth control pills, practolol, topical epinephrine, idoxuridine, echothiophate iodide, pilocarpine, timolol and dipivefrin-have also been implicated.
For mild erosions, ocular surface lubricants (artificial tears and/or ointments), topical non-steroidal anti-inflammatory agents for pain management and topical antibiotics to prevent infection are the mainstay of treatment. Pressure patches may also be employed to increase comfort when the size of the abrasion/erosion approaches 30%.
The management strategy in this presentation aims to improve patient comfort and reduce the frictional effects of the eyelid during blinking. Hypertonic sodium chloride solutions used three to four times during waking hours and ointment used at bedtime may have a beneficial effect, lubricating the corneal surface while dehydrating unwanted excess fluid from the stroma. Depending on the injury"s severity and the patient"s symptoms, cycloplegics may even be considered. Behavior modification may help patients learn to open their eyes slowly when waking. Long-term use of bland, nonmedicinal ointments at bedtime can prevent "dry" eye opening in the morning, when these injuries typically occur.
In cases involving bigger erosions with loose sheets of epithelium, scraping and debridement with a Weck-Cel sponge, Kimura spatula or a soaked cotton-tipped applicator may help induce efficient healing.
Extended-wear bandage soft contact lenses may provide comfort and support the healing process with minimal compromise of vision. They have the additional benefit of protecting and isolating the fragile, healing epithelium from the windshield-wiper effects of blinking eyelids. These lenses should remain on the cornea for at least 10 days to three weeks to allow the basement membrane and hemidesmosomes time to reorganize. An alternative for short-term relief and epithelial support is a collagen shield. Oral acetaminophen and ibuprofen can provide adequate additional analgesia.
If the erosions are severe or frequent, consider anterior stromal micropuncture or laser superficial keratectomy as therapeutic options.
Punctal occlusion with plugs or cautery can be performed, if scarring does not occur naturally, to increase the lacrimal lake.
Any blepharitis may be controlled with regular lid scrubs and antibiotic drops or ointments; consider oral preparations in recalcitrant cases.
In the worst cases, mucous membrane grafts can replace irreparably scarred conjunctivae.
Systemic immunosuppressive therapies (cyclosporine, cyclophosphamide, Imuran [azathioprine, Prometheus], corticosteroids) are currently being investigated for their potential benefits.1-6
When Restasis (cyclosporine 0.05%, Allergan) was approved by the Food and Drug Administration in December of 2002, it was introduced as the first topical medication to treat the underlying cause of inflammatory-based dry eye.1-3 When compared with chronic use of topical corticosteroids (which may also be considered within the class immunosuppressants), cyclosporine appears to be safer, without association with increasing intraocular pressure and minimal to no association with delayed wound healing. Further, there is no documented significant association of cyclosporine with cataractogenesis.3-6
Topical cyclosporine is an immunomodulator with a well-recognized safety profile. It acts as a selective T-cell immunosuppressive agent. T-cells are lymphocytes (white blood cells) that permit the immune system to guard against infection, aid in antibody production, assist in the response to cancers, as well as play a role in coordinating the activities of other cells within the immune system.3 Topical cyclosporine has demonstrated that it can prevent additional lymphocytes from joining into the inflammatory-destructive cascade.4-6 Because lymphocytes live in the body for approximately 110 days, allow a period of at least that long for cyclosporine to achieve its effect.4-6
1. Dart, J. Cicatricial pemphigoid and dry eye. Semin Ophthalmol 2005 Feb;20(2):95-100.
2. Stonecipher K, Perry HD, Gross RH, Kerney DL. The impact of topical cyclosporine A emulsion 0.05% on the outcomes of patients with keratoconjunctivitis sicca. Curr Med Res Opin 2005 Jul;21(7):1057-63.
3. Gurwood AS, Myers MD. Cyclosporine. Primary Care Optometry News 2004 May;9(5):4-6.
4. Kann G, Ozden O. Therapeutic use of topical cyclosporine. Ann Ophthalmol 1993 May;25(5):182-6.
5. Jannus SD, Lesher GA. Anti-inflammatory drugs. In: Janus SD, Bartlett J. Clinical Ocular Pharmacology, 3rd ed. Newton, Mass.: Butterworth-Heinemann 1995:321-8.
6. Perry HD, Donnenfeld ED. Targeting the pathology of dry eye. Cataract and Refractive Surgery Today 2003 Mar;3(3):68.


