 Conjunctival chalasis, or conjunctivochalasis, is a fairly common condition that is observed often in primary eye care. Its symptoms are very similar to those of dry eye; however, the key difference is that the hallmark sign of conjunctival chalasis is localized pain and/or foreign body sensation.
Conjunctival chalasis, or conjunctivochalasis, is a fairly common condition that is observed often in primary eye care. Its symptoms are very similar to those of dry eye; however, the key difference is that the hallmark sign of conjunctival chalasis is localized pain and/or foreign body sensation.
In one very recent study, more than 98% of individuals over the age of 60 (1,388 patients) demonstrated conjunctivochalasis.1 So, it is absolutely critical to understand the signs and symptoms of this exceedingly common condition.
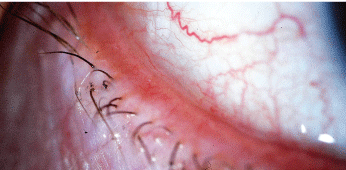
Conjunctival chalasis is characterized by loose or redundant conjunctival tissue.
Courtesy: John P. Herman, O.D.
Chalasis Characteristics
Patients with conjunctival chalasis generally have the ability to pinpoint the location of any associated pain, and they most commonly experience severe discomfort during blinking or eye movement.1 In fact, a clinician can reproduce pain by applying pressure on the lids over the area of conjunctival chalasis while the patient looks in the opposite direction.1
Conjunctival chalasis is characterized by loose or redundant conjunctival tissue and may be associated with the absence or stretching of subconjunctival tenons fascia.2 Mechanical forces between the lower lid and conjunctiva that gradually interfere with lymphatic flow may also be a possible cause.3 Histological slides show the presence of lymphangiectasia, which suggests that the chronic, prolonged mechanical obstruction of lymphatic flow may result in lymphatic dilation.1
Inflammation plays an important role in the pathogenesis of conjunctival chalasis, and the pooling of inflammatory cytokines in tears of patients with chalasis has been shown to compromise ocular surface health.4
The condition may be confused with dry eye disease because many patients who present with conjunctival chalasis experience epiphora secondary to redundant conjunctival prevention of tear flow to the punctum. Dry eye conditions can be exacerbated by the coexistence of conjunctival chalasis, which makes distinction of the two conditions more difficult.5
Almost all cases of conjuctival chalasis occur in the temporal conjuctiva, and more advanced cases of chalasis can result in exposure problems, such as exposure keratophathy.1,3
Risk Factors
The risk factors for conjunctival chalasis are advanced age (older than 50 years), a history of dry eye, prior ocular surgery and a history of conjunctival chemosis.6
Conditions that may cause conjunctival chemosis include longstanding allergic conjunctivitis; dry eye; trauma and inflammatory conditions, such as episcleritis.7 One prospective study found that the prevalence of conjuctival chalasis in patients with autoimmune thyroid eye diseases was as high as 88%.8 So, make sure to rule out any association with thyroid disease. If thyroid disease is present, an endocrinologist should initiate systemic treatment.
Treatment
Treat conjunctival chalasis with medications that target chemosis and inflammation, such as corticosteroids. Studies have also shown significantbut selectiveinflammatory markers in conjunctival chalasis, including pro-matrix metalloproteinase-9 and cytokines IL-6 and IL-1 beta.7 Thus, treatment with lubricants and corticosteroids, such as loteprednol, may be effective on a long-term basis (four to eight weeks).9
If pharmaceutical management is not effective in reducing chalasis, surgical intervention is recommended. Superficial conjunctival cauterization may be an effective treatment for mild or moderate levels of conjunctival chalasis, while moderate to severe cases may be treated by tightening the conjunctiva.10 Also,
consider conjunctival resection or amniotic membrane transplantation.11
Amniotic membrane transplantation facilitates rapid healing and recovery of normal epithelial phenotype in the epithelium, which reduces inflammation, vascularization and scarring in the stroma.12,13 Following surgery, patch the patients eye overnight. Then administer corticosteroids q.i.d., antibiotic drops q.i.d., and both topical and oral non-steroidal anti-inflammatory drugs. Schedule the patient to return for observation in one week.
Conjunctival chalasis is very common, but it is often overlooked because of its association with other conditions, such as dry eye. Or, it is simply dismissed as a side effect of the normal aging process (though the disease can occur at any age).3,16 Conjunctival chalasis is very significant and warrants a unique treatment plan that often includes surgical referral. Increased knowledge about both the diagnosis and management of conjunctival chalasis will facilitate improved patient care.
1. Mimura T, Yamagami S, Usui T, et al. Changes of conjunctivochalasis with age in a hospital-based study. Am J Ophthalmol 2008 Sep 3.
2. Kheirkhah A. New surgical approach for superior conjunctivochalasis. Cornea 2007 Jul;26(6):685-91.
3. Watanabe A, Yokoi N, Kinoshita S, et al. Clinicopathologic study of conjunctivochalasis. Cornea 2004 Apr;23(3):294-8.
4. Wang Y, Dogru M, Matsumoto Y, et al. The impact of nasal conjunctivochalasis on tear functions and ocular surface findings. Am J Ophthalmol 2007 Dec;144(6):930-7.
5. Di Pascuaza MA, Espana EM, Kawakita T, et al. Clinical characteristics of conjunctivochalasis with or without aqueous tear deficiency. Br J Ophthalmol 2004 Mar;88(3):388-92.
6. Francis IC, Chand DG Kim P, et al. Case-controlled clinical and histopathological study of conjunctivochalasis. Br J Ophthalmol 2005 Mar;89(3):302-5.
7. Acera A, Rocha G, Vecino E, et al. Inflammatory markers in the tears of patients with ocular surface disease. Ophthalmic Res 2008 Oct;40(6):315-21.
8. De Almeida SF. Clinic-cytologic study of conjunctivochalasis and its relation to thyroid autoimmune diseases: prospective cohort study. Cornea 2006 Aug;25 (7):789-93.
9. Latkany R. Dry eyes: etiology and management. Curr Op Ophthalmol Jul 2008;19(4):287-91.
10. Haefliger IO, Vysniauskiene I, Figueriredo AR, et al. Superficial conjunctiva cauterization to reduce moderate conjunctivochalasis. Klin Monatsbl Augenheilkd 2007 Apr;224(4):237-9
11. Meller D, Maskin SL, Pires RT, et al. Amniotic membrane transplantation for symptomatic conjunctivochalasis refractory to medical treatments. Cornea 2000 Nov;19(6):796-803.
12. Kruse FE, Meller D. Amniotic membrane transplantation for reconstruction of the ocular surface. Ophthalmologe 2001 Sep; 98(9):801-10.
13. Meller D, Tseng SC. Reconstruction of the conjunctival and corneal surface. Transplantation of amniotic membrane. Ophthalmologe 1998 Dec;95(12):805-13.
14. Meller D, Tseng SC. Conjunctivochalasis: literature review and possible pathophysiology. Surv Ophthalmol 1998 Nov-Dec; 43(3):225-32.

